How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Lung Disease?
If you have lung disease, Social Security disability benefits may be available. To determine whether you are disabled by your breathing problems, the Social Security Administration first considers whether your lung disease is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Lung Disease by Meeting a Listing. If you meet or equal a listing because of lung disease, you are considered disabled. If your breathing problems are not severe enough to equal or meet a listing, Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your lung disease), to determine whether you qualify for benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Lung Disease.
About Lung Disease and Disability
How Respiration Occurs
Red blood cells must be brought as closely as possible to the air we breathe, so that hemoglobin in the cells can give up waste carbon dioxide from cellular metabolism and take on oxygen. To accomplish this, the lungs have millions of tiny air sacs (alveoli) with very thin walls (alveolar membranes) containing microscopic blood vessels (capillaries) (see Figure 1 below). This anatomy of the lungs allows exposure of a large surface area of the blood to the air. Oxygen (O2) and carbon dioxide (CO2) gases diffuse (move) across the one cell thick alveolar membrane in opposite directions with the oxygen entering the blood and the carbon dioxide leaving it. This process is known as gas exchange.
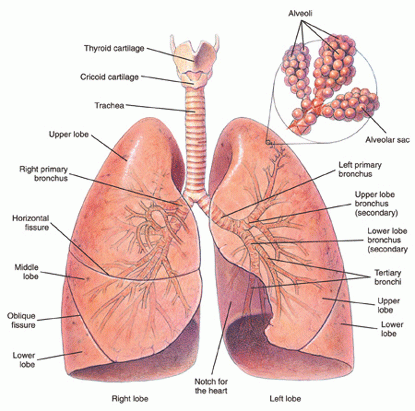
Figure 1: Bronchi and lungs.
The gas exchange part of the lungs is known as the lung parenchyma (see Figure 2 below). Air is delivered to the parenchyma of the lungs through the bronchial tree — a repetitively branching tubular system for air conduction. It consists of the trachea, from which arises a right and left main (primary) bronchus to the right and left lungs. Smaller bronchi branch from the main bronchus of the right or left lung, then to smaller bronchi to the various lobes of the lungs, then to even smaller bronchi (bronchioles) that eventually reach the alveoli.
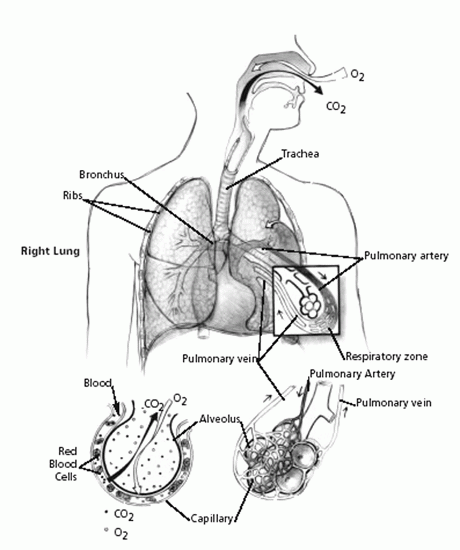
Figure 2: Mechanism of gas exchange.
How Respiration Is Impaired
Many diseases can affect breathing. The most useful classification of respiratory disorders is based on the manner in which the ability of air to come into contact with the hemoglobin in red blood cells (RBCs) is disrupted.
There are only two ways in which respiration can be impaired, regardless of the exact nature of the disorder:
1. Disease that prevents adequate amounts of air from reaching the gas-exchange level of the lungs (obstructive lung disease).
2. Disease of the lung tissue itself that reduces gas exchange (restrictive lung disease).
Thus, physicians have found it broadly useful to classify respiratory disorders as obstructive or restrictive, or a combination of the two.
Chronic Obstructive Lung Disease (COPD)
Chronic obstructive pulmonary disease (COPD) is the most common type of lung disease seen by the Social Security Administration. “Obstruction” refers to the fact that air flow in and out of the lungs is impeded. The three most frequent types of COPD in adults are:
- Emphysema.
- Chronic bronchitis.
- Asthma.
In emphysema, lung tissue itself is destroyed. Damaged lung tissue forms non-functional spaces that trap air, and the lungs expand. The effect of these abnormalities is to obstruct air flow to and from the lungs. Emphysema and chronic bronchitis often occur together usually in people with a history of cigarette smoking.
Chronic bronchitis can also occur from long exposure to chemical fumes associated with a particular occupation. Inflammation of the inner surface of bronchi results from exposure to irritating substances. This inflammation, along with excessive secretion of bronchial mucous glands, results in bronchial narrowing. Thus, bronchial tree resistance to air flow increases—there is obstruction of air flow. For patients with COPD and airflow blockage issues, using hospital beds can be beneficial. These beds allow patients to find positions that ease breathing difficulties. Consider exploring elegant hospital beds that combine style and comfort to enhance the overall experience for individuals managing COPD.
Other less common causes of COPD include cystic fibrosis and bronchopulmonary dysplasia (BPD). These disorders, as well as asthma, have separate specific listings. See Can I Get Social Security Disability Benefits for Asthma? and Can I Get Social Security Benefits for Cystic Fibrosis?
Restrictive Lung Disease
The hallmark of restrictive lung disease is loss of usable lung volume, either due to:
1. Disease of the gas exchange part of the lungs (lung parenchyma), or
2. Some disorder outside of the lungs (extrapulmonary) that prevents air from adequately ventilating normal lung parenchyma.
Examples of Parenchymal Restrictive Lung Diseases
- Infections (bacterial, fungal, viral, parasitic). Chronic infections that damage lung tissue, such as severe bronchiectasis or advanced pulmonary TB, could result in some degree of restrictive impairment.
- Radiation, such as used for treatment of cancer, can damage lungs. Radiation lung damage is less of a problem than in the past, because modern equipment can direct therapeutic radiation in beams precisely delivered to the tumor. To the extent that this is impossible because of the size or location of the tumor, it is possible to have fibrotic lung damage caused by radiation.
- Inhalation of damaging substances into the lung. Pneumoconiosis is a non-specific term that refers to lung damage from inhaling small particles of some kind. Examples of pneumoconiosis include that caused by asbestos (asbestosis) (see Figure 3 below), coal dust (anthracosis), beryllium (berylliosis), silicon dust (silicosis), aluminum, iron, tin (stannosis) and talc. Inhalation of toxic chemicals—such as acidic fumes—can also damage lung tissue.
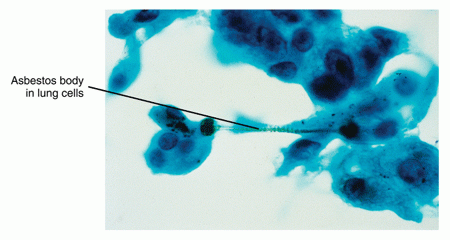
Figure 3: Asbestos in lung cells.
- Drug side-effects.
- Autoimmune diseases. Autoimmune disorders such as sarcoidosis, scleroderma, systemic lupus erythematosus (SLE), rheumatoid arthritis (RA), polymyositis, ankylosing spondylitis, and mixed connective tissue disorders can cause pulmonary disease. In all of these disorders, some kind of immune system dysfunction damages the lungs. See Can I Get Social Security Disability Benefits for Lupus? and Can I Get Social Security Disability Benefits for Arthritis and Joint Damage?
- Idiopathic diffuse interstitial pulmonary fibrosis (cryptogenic fibrosing alveolitis). This condition causes progressive scarring of the lungs on a microscopic level. This damage can result in decreased gas exchange capacity of the lungs, increasingly severe hypoxemia (lack of oxygen in the blood) and eventually death from respiratory failure. The rate of progression is highly variable, but median survival is less than 3 years. Some cases remain slowly progressive for a number of years, then are triggered by some unknown event to become rapidly more severe.
- Other diseases. Examples of other diseases that can cause pulmonary fibrosis include alveolar proteinosis, acquired immunodeficiency syndrome (AIDS), acute respiratory distress syndrome (ARDS), amyloidosis, bone marrow transplantation, cancer, eosinophilic granuloma, eosinophilic pneumonia, lipoid pneumonia, genetic metabolic diseases caused by enzyme deficiencies (Gaucher’s disease, Niemann-Pick disease), Hermansky-Pudlak syndrome, pulmonary vasculitis, tuberous sclerosis, and neurofibromatosis. See Can I Get Social Security Disability Benefits for HIV / AIDS?
Examples of Extrapulmonary Restrictive Lung Diseases
- Abnormal spinal curvatures. Abnormal curvatures of the spine can interfere with normal breathing movements. Scoliosis is a common spinal disorder, but will not compromise breathing until the major abnormal curve reaches about 60 degrees. Kyphosis is an abnormal curvature of the upper (thoracic) spine that causes a bent-forward or “hunched-over” posture. Kyphoscoliosis is a combination of both kyphosis and scoliosis.
- Surgical resection. Removal of lung tissue limits the surface area available for gas exchange.
- Spondyloarthropathies. Inflammatory disorders of the spine, such as ankylosing spondylitis, can make the spine more rigid by increased calcification of the spine and associated soft tissue ligaments. The ribs attach to the spine and their movement is impeded during expansion and relaxation of the chest during breathing. This limitation will decrease breathing capacity. See also Can I Get Social Security Disability Benefits for Back Pain?
- Thoracoplasty. Thoracoplasty, usually involving removal of one or more ribs, distorts the normal shape of the chest. The intercostal muscles between the ribs help expand the chest during inspiration. However, mechanical distortion of the chest wall is probably more important in decreasing ability to ventilate the lung during respiratory movements of the chest.
- Obesity. Marked obesity can result in a significant reduction in ventilation capacity. Because of the weight of fat on the chest wall, the work of breathing is increased during inspiration. Furthermore, abdominal subcutaneous fat as well as intra-abdominal fat resists movement of the diaphragm—a respiratory muscle consisting of two sheets of muscle separating the chest and abdominal cavities (see Figure 4 below). The diaphragm must be able to move downward with inhalation in order to maximally expand the chest.
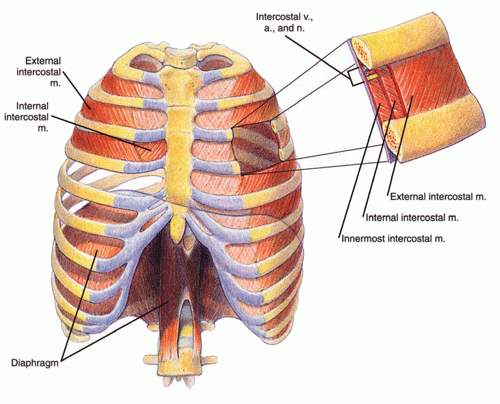
Figure 4: Chest cavity and diaphragm.
- Other important causes of restrictive respiratory impairment. Many disorders can result in weakness affecting the muscles of respiration (diaphragmatic muscles or intercostal muscles). Myasthenia gravis is an autoimmune disease that causes weakness through a biochemical interruption of the body’s ability to excite muscles, including the muscles of respiration. In fact, respiratory failure is usually the cause of death in myasthenia. There are a large number of muscle diseases (myopathies) that can affect respiration, although fairly rare in the general population.
Strokes and Breathing Problems
Strokes (cerebrovascular accidents, CVAs) are frequently adjudicated by the Social Security Administration. See Can I Get Social Security Disability Benefits After a Stroke? However, most of the time the treating source—even if a neurologist—does not consider the possibility of a breathing deficit resulting from the stroke. However, paralysis of half of the diaphragm is a definite possibility with resultant decreased ability to ventilate the lungs. Because treating sources, or consulting neurologists paid by the Social Security Administration, usually do not specifically address the possibility of diaphragmatic paralysis, SSA adjudicators are also likely to not even think of the possibility. Claimants themselves, following a stroke, may have thinking difficulties and neurological problems that occupy their attention as well as the attention of their family. The claimant cannot be counted on to mention breathing difficulty—especially since he or she may not even have symptoms in a resting state. The Social Security Administration adjudicator should ask treating doctors, especially neurologists, regarding possible breathing deficits in post-stroke patients.
Pulmonary Function Studies
Pulmonary function study (PFS) is a general term that applies to any type of respiratory testing. The basic types of PFS are:
- Spirometry
- Arterial Blood Gas Study (ABGS)
- Carbon Monoxide Diffusing Capacity (DLCO)
Shortness of breath is one of the most common allegations by claimants seeking Social Security disability benefits. The Social Security Administration pays for many PFS tests (especially spirometry) to address allegations of shortness of breath.
The results of these tests determine whether you qualify for disability benefits under a listing. See Winning Social Security Disability Benefits for Lung Disease by Meeting a Listing.
Spirometry
No pulmonary function study is more useful or more frequently performed than spirometry. Spirometry is the most important test for evaluating the severity of obstructive pulmonary disease. Spirometry requires you to inhale then exhale into a device called a spirometer. The device measures the volume of air that you can inhale and exhale and displays the result as a breathing curve on a graph called a spirogram.
If you have lung disease, but have not had a spirometry test, the Social Security Administration may arrange for you to have one. Even if you have had the test, the Social Security Administration may require you to be retested because the test must be administered in accordance with strict rules. Accurate testing must be done to assure you are treated fairly.
The test results must include the actual breathing curves. Spirometry test results in medical records often do not include the actual breathing curves, just the numerical results.
If there is no clinical evidence that you have significant lung disease and the reported spirometric values in your medical records are not significantly abnormal, the Social Security Administration will not send you for retesting. In fact, the Social Security Administration is not obligated to obtain spirometry on claimants who have no evidence in their medical records of a respiratory disorder, even if there are no spirometric values of any kind in the file.
Arterial Blood Gas Study (ABGS)
ABGS is the most important test used for the evaluation of the restrictive pulmonary disorders that involve a decrease in gas exchange—the parenchymal restrictive lung diseases. ABGS is performed on a sample of blood from the radial artery in the wrist or brachial artery in the arm, unlike most blood samples that are taken from a superficial vein just under the skin.
An ABG test checks how well your lungs are doing in moving oxygen into the blood and removing carbon dioxide from it. ABGS measures arterial oxygen pressure (PaO2), also known as oxygen tension, carbon dioxide pressure (PaCO2), and acidity (pH).
The Social Security Administration should not send you for ABGS, unless absolutely necessary to determine whether you are disabled, because it is invasive. Although complications are unusual, the person sticking a needle in the radial artery could damage the artery or other structures in the wrist; use of the brachial artery carries additional risk and should be done only when the radial artery cannot be used. The needle stick is also painful in either method.
Carbon Monoxide Diffusing Capacity (DLCO)
DLCO is a test used to evaluate of the severity of parenchymal restrictive lung diseases. It is of little value in assessing severity in COPD. The test measures how well your lungs can transfer carbon monoxide (CO) into the blood. By measuring how easily CO moves across the alveolar membrane of the lungs, doctors can deduce whether there is also a problem limiting the exchange of oxygen and carbon dioxide between blood and the atmosphere.
Two different methods are used for this test. The single-breath method is the one required by the Social Security Administration. This method requires you to take a breath of air containing a very small amount of carbon monoxide from a container while measurements are taken. (The other method, the steady-state method, requires you to breathe air containing a very small amount of carbon monoxide. The amount of carbon monoxide in the breath you exhale is then measured.)
DLCO can be abnormal in emphysema, if the disease is very advanced, because lung tissue is damaged. However, DLCO is not an accurate enough means of determining the severity of emphysema; spirometry is more appropriate. In some instances, more applicable to clinical medicine than disability determination, DLCO testing can help distinguish between emphysema and asthma, because asthma will have normal values.
Winning Social Security Disability Benefits for Lung Disease (Chronic Pulmonary Insufficiency) by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your breathing difficulties are severe enough to meet or equal the chronic pulmonary insufficiency listing. The Social Security Administration has developed rules called Listing of Impairments for most common impairments. The listing for a particular impairment describes a degree of severity that Social Security Administration presumes would prevent a person from performing substantial work. If your lung disease is severe enough to meet or equal the chronic pulmonary insufficiency listing, you will be considered disabled.
The listing that applies to chronic pulmonary insufficiency is 3.02. It has 3 parts, A, B, and C.
Part A applies to chronic obstructive pulmonary disease. Part B applies to chronic restrictive ventilator disease. Part C applies to chronic impairment of gas exchange.
Important to note for all three parts of the listing is that:
- Chronic impairment must be present, and
- All pulmonary diseases can potentially qualify.
The Social Security Administration will first consider whether your lung disorder will satisfy the 12-month duration requirement that all impairments must meet. Once impairment duration is established or expected, the severity of your impairment can be determined by several methods of testing. The real question that all these tests seek to answer is how well you can oxygenate your blood and remove waste carbon dioxide gas. If your lung disease meets or equals a listing, the Social Security Administration presumes that these vital respiratory functions would be too severely impaired to permit you to carry out even sedentary work activities. The nature of your respiratory disorder determines which part of this listing is most appropriate to evaluate the severity of the impairment.
Meeting Social Security Administration Listing 3.02A for Chronic Pulmonary Insufficiency
Part A involves evaluation of the results of spirometric testing of chronic obstructive pulmonary disease. According to this listing, if you are diagnosed with chronic obstructive pulmonary disease due to any cause, you will be disabled if you have an FEV1 equal to or less than the values specified in Table I corresponding to your height without shoes. FEV stands for forced expiratory volume. FEV1 is the amount of air you can exhale with force in one breath measured at 1 second.
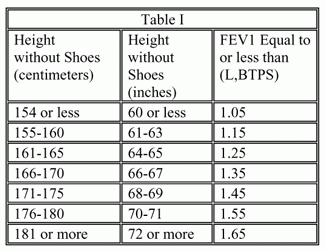
FEV1 is the important measurement for COPD and it decreases in proportion to the severity of the lung disease.
In reality, gender and age affect normal values but they are not taken into account in part A. Since older women have somewhat lower normal predicted values for a given height than men, failure of the table to make a distinction is to the advantage of older women.
For the test results to be valid, your height must be measured without shoes. Taller people have larger lungs, so normal values for FEV1 are higher for those individuals and this fact is reflected in the spirometric tables. It is not unusual for the Social Security Administration to have to send a claimant to a consultative examination just to get an accurate height.
If your height measured in inches falls between the whole number values in the respective tables, it should be rounded off to the nearest inch by whole number. If the fraction is precisely one-half inch, the height measured should be rounded off to the next highest whole number. The importance of the above rounding policy cannot be overstated. This is a perfect example of how attention to detail can make the difference between allowance and denial of benefits, since FEV1 values are exactly specified.
Meeting Social Security Administration Listing 3.02B for Chronic Pulmonary Insufficiency
Part B involves evaluation of the results of spirometric testing of restrictive pulmonary disease. You will meet part B of the listing if you have chronic restrictive ventilatory disease due to any cause, with the FVC equal to or less than the values specified in Table II corresponding to your height without shoes. FVC stands for forced vital capacity. It is the amount of air you can exhale with force after you inhale as deeply as possible.
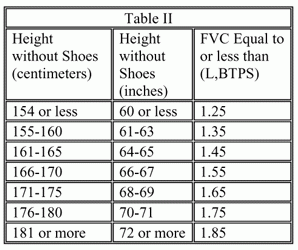
FVC is the most important measurement for restrictive lung disease and it decreases in proportion to the severity of the lung disease. The FEV1 used to determine severity in COPD may be normal in restrictive lung diseases.
In reality, gender affects normal values but that is not taken into account. Women have somewhat lower normal predicted values for a given height than men, so failure of the table to make a distinction is to the advantage of women.
If your height measured in inches falls between the whole number values in the respective tables, it should be rounded off to the nearest inch by whole number. If the fraction is precisely one-half inch, the height measured should be rounded off to the next highest whole number. The importance of the above rounding policy cannot be overstated. This is a perfect example of how attention to detail can make the difference between allowance and denial of benefits, since FVC values are exactly specified.
Meeting Social Security Administration Listing 3.02C for Chronic Pulmonary Insufficiency
You will meet part C of the listing if you have chronic impairment of gas exchange due to clinically documented pulmonary disease. With:
- Single breath carbon monoxide diffusing capacity (DLCO) less than 10.5 ml/min/mm Hg or less than 40 percent of the predicted normal value. (Predicted values must either be based on data obtained at the test site or published values from a laboratory using the same technique as the test site. The source of the predicted values should be reported. If they are not published, they should be submitted in the form of a table or nomogram); or
- Arterial blood gas values of PO2 and simultaneously determined PCO2 measured while at rest (breathing room air, awake and sitting or standing) in a clinically stable condition on at least two occasions, three or more weeks apart within a 6-month period, equal to or, less than the values specified in the applicable Table III-A or III-B or III-C:


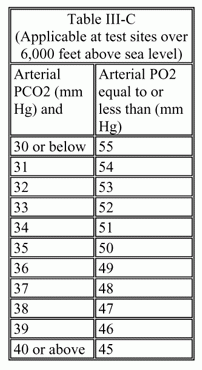
Or
3. Arterial blood gas values of PO2 and simultaneously determined PCO2 during steady state exercise breathing room air (level of exercise equivalent to or less than 17.5 ml O2 consumption/kg/min or 5 METs) equal to or less than the values specified in the applicable Table III-A or III-B or III-C in listing 3.02 C2.
ABGS done during acute respiratory distress of any kind are not reliable for determination of chronic impairment and cannot be used to evaluate severity under the listing.
The three tables in part C have different values, because normal arterial oxygen pressure decreases with altitude. In medical records or elsewhere, reports of ABGS should always specify the percentage of oxygen the patient is breathing (FIO2) when the ABGS is done. The normal atmosphere consists of about 21% oxygen. FIO2 21% or 0.21 means the person is breathing normal air without oxygen supplementation. RA (room air) means the same thing, and is a commonly used abbreviation.
Part C.1
Part C.1 is satisfied if 10.5 milliliters of carbon monoxide gas per minute, or less, diffuses into the blood for each millimeter of pressure. Alternatively, if the result is 40% or less than the predicted normal value used by the testing laboratory, then part C.1 is fulfilled. Failure to satisfy one of these criteria does not preclude allowance under the other.
Part C.2
Part C.2 can be satisfied by resting oxygen and carbon dioxide pressures adjusted for altitude. The Social Security Administration may send you for a resting ABGS when there is a question of whether your impairment meets or is equivalent in severity to a listing, and the claim cannot otherwise be favorably decided. If the results of a DLCO study are greater than 40% of predicted normal but less than 60% of predicted normal, the Social Security Administration should consider a resting ABGS. In other words, you must have had spirometry and DLCO testing prior to the resting ABGS, and there must be no possibility that your claim will be allowed based on these tests. A further restriction is that the DLCO must be greater than 40%, since lower values would qualify under part C.1. Finally, values of 60% or more for the DLCO would generally preclude purchase of ABGS, because values that high would not be expected to be associated with abnormal ABGS.
Part C.3 Exercise ABGS
Part C.3 provides for ABGS to be done during exercise. Individuals with a DLCO greater than 60% of predicted normal would not usually be considered for exercise testing with measurement of arterial blood gas studies; they are unlikely to have an abnormal exercise result. Exercise ABGS are not often done by the Social Security Administration, but represent an important testing procedure in selected cases. With a parenchymal restrictive lung disease like idiopathic fibrosis, exercise puts a demand on the lungs for more oxygen to supply the muscles but the disease limits gas exchange. Direct measurement of PaO2 is done during exercise as specified by methodology in part C.1.
Exercise ABGS should not be ordered if you have the following conditions:
- Unstable angina pectoris.
- Congestive heart failure.
- Uncontrolled arrhythmias.
- Uncontrolled severe systemic arterial hypertension.
- Marked aortic stenosis.
- Severe pulmonary hypertension.
- Chronic or dissecting aortic aneurysm.
- Acute illness.
- Limiting neurological or musculoskeletal impairments.
- Contraindications due to the type of medication(s) prescribed.
How does the Social Security Administration decide when purchase of exercise ABGS is relevant to the disability determination? Claimants with DLCO values of 41–60% of predicted normal and not allowable with resting ABGS, or by any other means, should be considered for exercise ABGS. Such a decision is not automatic; most relevant are cases in which the evidence indicates symptomatology significantly worse than would otherwise be expected from the objective findings. In these instances, exercise can expose underlying severity that otherwise would not be documented.
Further Considerations Regarding Part C.3
Exercise ABGS testing should never be administered by anyone other than a sub-specialist in pulmonary medicine with the requisite expertise. That physician has the final decision about whether it is medically appropriate to carry out testing. The test is invasive; an indwelling arterial catheter must be placed. Therefore, there is some pain, some risk that a piece of the catheter could break in the radial artery, some risk that the artery may be permanently damaged, and some risk of infection. In addition to making a medical determination about the safety of testing, that examining specialist will inform you of any risk and obtain informed consent.
There are also the risks associated with exercise testing of any kind, such as cardiac arrhythmias. Although the low level of exercise makes such cardiac complications unlikely, the presence of dropping arterial oxygen as a result of lung disease (development of hypoxemia) during exercise increases the risk of arrhythmias beyond what would be present in a normal individual. These risks are not great with appropriate pre-test physical examination, review of medical records by a pulmonologist, and expert monitoring during testing.
If exercise ABGS has been done by your treating physician prior to application for disability benefits, that information should be used, if possible. If your treating physician states to the Social Security Administration that exercise ABGS testing is contraindicated, there is a good chance the Social Security Administration will not request such testing. However, the treating physician should be willing to provide an explanation for that judgment.
Use of Supplemental Oxygen
Use of supplemental oxygen is common among claimants with lung disease. Your use of oxygen in itself is not proof of impairment, just as use of a crutch does not demonstrate inability to walk. The Social Security Administration will need to obtain your doctor’s reasons for prescribing supplemental oxygen to determine if you truly need it.
A claimant truly needing supplemental oxygen would easily qualify under part C.2 of the listing. The use of supplemental oxygen becomes mandatory at a resting PaO2 of about 55 mm Hg. In individuals with severe co-existing heart disease, supplemental oxygen might be needed for values up to 59 mm Hg. Such values are not absolutes, but must be tailored to the individual.
If you need oxygen you should not be sent for spirometry or DLCO testing.
To obtain resting ABGS, your oxygen would need to be terminated for a few minutes to determine your natural PaO2. If the Social Security Administration is contemplating sending you for ABGS and you use oxygen, the Social Security Administration should contact your treating physician and ask:
1) Why you are receiving oxygen;
2) For clinical and laboratory evidence regarding your pulmonary disease; and
3) Whether it is safe for you to receive ABGS without oxygen flow if this information has not already been received into the file.
If your treating physician does not cooperate or the information obtained is vague, the Social Security Administration can send you to an internal medicine specialist, preferably a pulmonary sub-specialist, who can provide a professional evaluation of your pulmonary condition and appropriateness of further testing without the use of oxygen.
Determination of Equivalence in COPD
The FEV1 is the most important test for assessment of chronic severity of emphysema, chronic bronchitis, asthma, and other forms of obstructive pulmonary disorders. However, claimants with advanced lung disease—particularly emphysema—can demonstrate severity equivalent to the requirements of the listing without spirometry. These individuals have had numerous ABGS done that reflect their chronic condition and are associated with adjustments in supplemental oxygen requirements. They are also usually malnourished, because of loss of appetite associated with chronic disease and the added respiratory effort required to ventilate. They very well may have heart disease associated with their lung disease (cor pulmonale). Additionally, they frequently have ischemic heart disease associated with a history of cigarette smoking.
These types of claims characteristically include volumes of medical records. But the file may lack any spirometric results—or the actual breathing curves may not be in the file, if spirometry was done. It is not necessary for the Social Security Administration to send such claimants to spirometric testing, and it is important to bear in mind that ABGS need not necessarily satisfy part C.2 of the listing for a finding of equivalence. Other medical conditions, such as malnutrition, can often provide the basis for a finding of additional severity. Malnutrition in chronic lung disease is an important and common problem.
Residual Functional Capacity Assessment for Lung Disease
What Is RFC?
If your lung disease is not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary work in spite of your impairments. The lower your RFC, the less the Social Security Administration believes you can do. Claimants close to the listing should be restricted to no higher than sedentary exertion.
Claimants with Both Lung and Heart Disease
The close physiological relationship between the cardiovascular and pulmonary systems means an impairment in one of these systems influences the other. For example, it is very common for a claimant with COPD caused or aggravated by cigarette smoking to also have significant cardiac disease or peripheral vascular disease as separate impairments. Thus, if you have both heart and respiratory impairments, you will have a much worse functional restriction than if you had either alone. For example, if you would be restricted to medium work on the basis of cardiovascular disease and medium work because of respiratory disease, you should receive a RFC for no higher than light work.
Removal of Lung Tissue
Removal of lung tissue (pulmonary resection) can also limit the RFC. The most frequent type of pulmonary resection is a lobectomy associated with surgery for lung cancer. Sometimes, a pneumonectomy involving the removal of an entire right or left lung is performed.
In otherwise healthy lungs, a lobectomy usually results in an exertional restriction to medium work when the results of spirometry are evaluated. In cases of pneumonectomy, an RFC is always required, and even with a healthy remaining lung is usually no higher than light work.
As with other pulmonary impairments, environmental restrictions from exposure to excessive dust and fumes would be indicated on the RFC.
The fact that a treating surgeon may say something in his or her medical notes like, “The patient has fully recovered from surgery and has no difficulty breathing,” does not mean that spirometry does not have to be performed. When significant amounts of lung tissue are removed, there will be some degree of pulmonary limitation.
Most claimants with pulmonary resection associated with removal of a lung cancer are operated on because they have cancer caused by cigarette smoking. Claimants who have smoked long enough to develop lung cancer always have chronic obstructive pulmonary disease and will have pulmonary deficits worse than would be expected if the remaining lung tissue were normal (see Figure 5 below). This is another reason it would be improper for the Social Security Administration to guess about remaining lung function without obtaining spirometry (unless the claim is otherwise allowable). Whether or not a claimant post-resection for lung cancer complains of shortness of breath, the Social Security Administration has a responsibility to evaluate the residual breathing impairment.
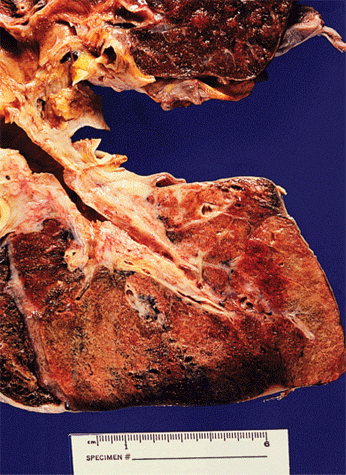
Figure 5: Smoker’s lung.
Lung Disease With Gas Exchange Impairment
If you have a lung disease that produces gas exchange impairment, you should not receive RFC levels of exertion that could cause you to desaturate (lose oxygen from the blood), so that you become so hypoxemic (oxygen deprived) that you are in danger of a cardiac arrhythmia (and consequent sudden death), or in danger of loss of consciousness. Desaturation can happen so quickly that you have no reliable symptom warning signs.
Whether exercise produces hypoxemia depends on the amount of exercise and severity of the underlying disease, as well as environmental factors such as extreme heat and cold. Exercise arterial blood gas studies (ABGS) that produce actual PaO2 measurements correlated with known levels of exercise is useful. In these instances, your RFC determination should be at least one level below the exercise level at which limiting symptoms or hypoxemia appears. In other words, you should never receive a RFC that corresponds to the exercise test exertional level alone, unless there is no hypoxemia.
To further illustrate, suppose claimant A, with heart disease but no lung disease, reaches an exercise level on a treadmill that indicates the ability to perform light level work. Now consider claimant B, with restrictive lung disease but no heart disease, who does as much exercise on the treadmill, but who develops hypoxemia as measured with ABGS. The latter claimant should receive no higher than a sedentary RFC.
In addition to the objective medical evidence, the opinion of your treating physician about your exercise capacity and symptoms and your own observations and those of your family can be helpful in determining RFC.
Information About Your Activities
You should take care to provide the Social Security Administration with a clear picture regarding the speed at which you can carry out various activities, particularly as limited by shortness of breath. If you state you can climb two flights of stairs, the Social Security Administration might use that information but it is incomplete. There are several pieces of information missing: 1) Are the stairs climbed at a normal pace? 2) Do you have to stop and rest on the way up, limited by shortness of breath?
Similarly, it is misleading to say you can walk 1 block or 2 blocks or 3 blocks. If the pace is slow enough, some people with chronic pulmonary disease can walk several miles. But if it’s a slow struggle, it hardly represents any practical functional capacity.
Use of the arms can bring on rapid shortness of breath. So it is important to provide times for completion of daily activities, if possible. If not, comparisons to normal individuals can help define functional limitation. For example, “I can walk a block before I get short of breath, but I can’t keep up with my wife” is a much more revealing statement than “I get short of breath walking.”
The ability to do heavy, medium, light, or sedentary work is not correlated to any particular pulmonary function test results. However, spirometric or other test values of 80% or more of predicted normal are generally considered a strong argument for a “not severe” impairment that requires no RFC limitations. Intermediate results must be interpreted on a case by case basis considering all of the evidence, including your symptoms. The Social Security adjudicator should keep in mind where along the numerical spectrum your test results lie between meet-level severity and normal values.
Symptoms of shortness of breath correlate only loosely with severity of pulmonary disease as measured by pulmonary function studies. For example, a claimant whose lung function would suggest a capacity for medium work might credibly have shortness of breath that limits him or her to light work—symptoms can certainly produce a greater restriction than is present from a purely physiological standpoint. Some SSA adjudicators may mechanically apply particular test values to particular RFCs. This is improper and not supported by any official policy.
Environmental Limitations
All claimants with respiratory disorders severe enough to warrant a RFC should receive limitations from exposure to excessive dust and fumes. Furthermore, work at cold temperatures can increase symptoms of shortness of breath and decrease exercise capacity in individuals with COPD such as asthma, emphysema, and chronic bronchitis.
Getting Your Doctor’s Medical Opinion About What You Can Still Do
Your Doctor’s Medical Opinion Can Help You Qualify for Social Security Disability Benefits
The Social Security Administration’s job is to determine if you are disabled, a legal conclusion based on your age, education and work experience and medical evidence. Your doctor’s role is to provide the Social Security Administration with information concerning the degree of your medical impairment. Your doctor’s description of your capacity for work is called a medical source statement and the Social Security Administration’s conclusion about your work capacity is called a residual functional capacity assessment. Residual functional capacity is what you can still do despite your limitations. The Social Security Administration asks that medical source statements include a statement about what you can still do despite your impairments.
The Social Security Administration must consider your treating doctor’s opinion and, under appropriate circumstances, give it controlling weight.
The Social Security Administration evaluates the weight to be given your doctor’s opinion by considering:
- The nature and extent of the treatment relationship between you and your doctor.
- How well your doctor knows you.
- The number of times your doctor has seen you.
- Whether your doctor has obtained a detailed picture over time of your impairment.
- Your doctor’s specialization.
- The kinds and extent of examinations and testing performed by or ordered by your doctor.
- The quality of your doctor’s explanation of your impairment.
- The degree to which your doctor’s opinion is supported by relevant evidence, particularly medically acceptable clinical and laboratory diagnostic techniques.
- How consistent your doctor’s opinion is with other evidence.
When to Ask Your Doctor for an Opinion
If your application for Social Security disability benefits has been denied and you have appealed, you should get a medical source statement (your doctor’s opinion about what you can still do) from your doctor to use as evidence at the hearing. You may consult your social security disability lawyer about this.
When is the best time to request an opinion from your doctor? Many disability attorneys wait until they have reviewed the file and the hearing is scheduled before requesting an opinion from the treating doctor who can provide evidence if you underwent treatment such as Workers Compensation Injury Physical Therapy, urgent medical care, etc. This has two advantages.
- First, by waiting until your attorney has fully reviewed the file, he or she will be able to refine the theory of why you cannot work and will be better able to seek support for this theory from the treating doctor.
- Second, the report will be fresh at the time of the hearing.
But this approach also has some disadvantages.
- When there is a long time between the time your attorney first sees you and the time of the hearing, a lot of things can happen. You can improve and go back to work. Your social security disability lawyer or workers compensation lawyer can still seek evidence that you were disabled for a certain length of time. But then your lawyer will be asking the doctor to describe your ability to work at some time in the past, something that not all doctors are good at.
- You might change doctors, or worse yet, stop seeing doctors altogether because your medical insurance has run out. When your attorney writes to a doctor who has not seen you recently, your attorney runs the risk that the doctor will be reluctant to complete the form. Doctors seem much more willing to provide opinions about current patients than about patients whom they have not seen for a long time.
Here is an alternative. Suggest that your attorney request your doctor to complete a medical opinion form on the day you retain your attorney. This will provide a snapshot description of your residual functional capacity (RFC) early in the case. If you improve and return to work, the description of your RFC provides a basis for showing that you were disabled for a specific period. If you change doctors, your attorney can get an opinion from the new doctor, too. If you stop seeing doctors, at least your attorney has one treating doctor opinion and can present your testimony at the hearing to establish that you have not improved.
If you continue seeing the doctor but it has been a long time since the doctor’s opinion was obtained, just before the hearing your attorney can send the doctor a copy of the form completed earlier, along with a blank form and a cover letter asking the doctor to complete a new form if your condition has changed significantly. If not, your attorney can ask the doctor to send a one-line letter that says there have been no significant changes since the date the earlier form was completed.
There are times, though, that your attorney needs to consider not requesting a report early in the case.
- First, depending on the impairment, if you have not been disabled for twelve months, it is usually better that your attorney wait until the twelve-month duration requirement is met.
- Second, if you just began seeing a new doctor, it is usually best to wait until the doctor is more familiar with your condition before requesting an opinion.
- Third, if there are competing diagnoses or other diagnostic uncertainties, it is usually best that your attorney wait until the medical issues are resolved before requesting an opinion.
- Fourth, a really difficult judgment is involved if your medical history has many ups and downs, e.g., several acute phases, perhaps including hospitalizations, followed by significant improvement. Your attorney needs to request an opinion at a time when the treating doctor will have the best longitudinal perspective on your impairment.
Medical Opinion Forms
Medical opinion forms can be great time savers for both your attorney and your doctor, but they must be used with care. Forms may not be appropriate at all in complex cases; and they need to be supplemented in many cases so that all issues are addressed. The best forms are clear and complete but not too long.

