How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Multiple Sclerosis?
If you have multiple sclerosis (MS), Social Security disability benefits may be available. To determine whether you are disabled by MS, the Social Security Administration first considers whether your MS is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Multiple Sclerosis by Meeting a Listing. If you meet or equal a listing because of your MS, you are considered disabled. If your MS is not severe enough to equal or meet a listing, Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your MS), to determine whether you qualify for disability benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Multiple Sclerosis.
About Multiple Sclerosis and Disability
What Is Multiple Sclerosis?
Multiple sclerosis is a slowly progressive disease of the central nervous system (CNS), i.e., the spinal cord (see Figure 1 below) and brain. The incidence of multiple sclerosis in the U.S. is not reliably known—estimates vary between 250,000 to 350,000 people. In MS a substance known as myelin, which serves as the electrical insulating coating of nerve fiber tracts, is destroyed. Nerve tracts (bundles of communicating fibers) make up the “white matter” of the CNS. Therefore, white matter lesions (wounds or injuries) are characteristic of multiple sclerosis.
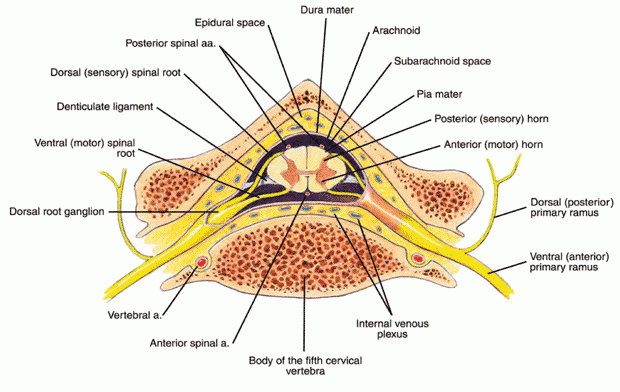
Figure 1: Interior view of the spinal cord.
The brain’s white matter lies beneath the brain’s outer cerebral cortex (see Figure 2 below), or “gray matter” that is composed of brain cells (neurons). Most of the volume of the brain is made up of cerebrospinal fluid-filled cavities and white matter. Since the white matter carries information to and from the cortical neurons composing the gray matter, the function of the gray matter can easily be affected by white matter abnormalities. For example, an impulse to move a leg that starts in the motor cortex of the brain could be disrupted when it enters the white matter for transmission to the spinal cord.
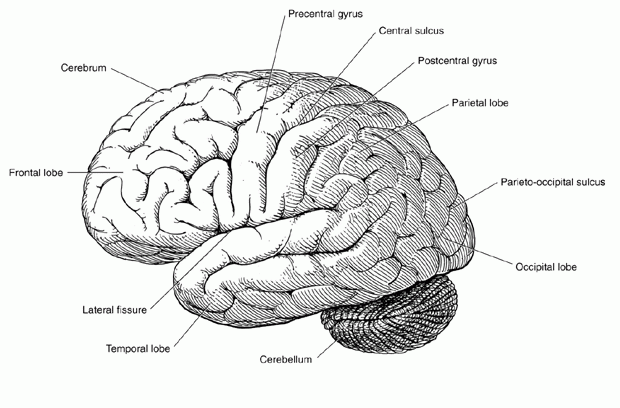
Figure 2: Outer cerebral cortex of the brain.
The myelin destruction associated with multiple sclerosis is called demyelinization. MS is not the only disorder that can result in that abnormality. The white matter lesions of demyelinating disorders are called plaques. The plaques of MS occur in multiple and varied locations in the spinal cord and brain, particularly the brain (see Figure 3 below). Brain cells that make myelin are also damaged, but can regenerate to some extent to produce more myelin.
Most people with multiple sclerosis have a normal lifespan, so it is not known as a fatal disorder.
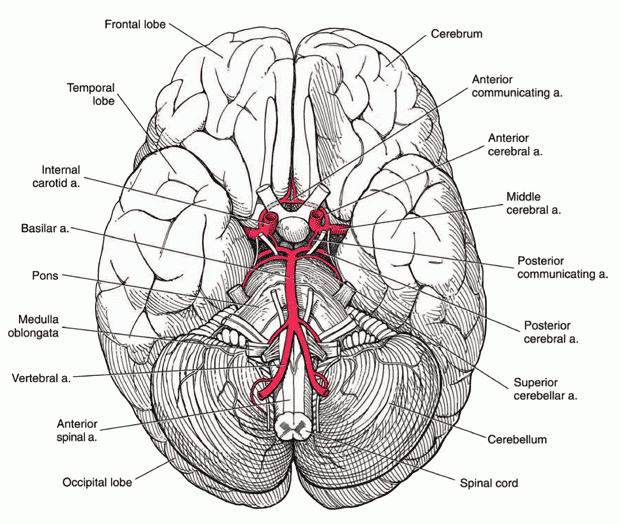
Figure 3: Base of the brain.
Cause of Multiple Sclerosis
The cause of MS is unknown. MS is more common in temperate than tropical areas, and moving between geographic regions at certain ages can affect the risk developing the disorder. Theories as to cause have considered a virus, brain trauma, or a problem in the immune system, but these are little more than speculation. Close relatives of people with multiple sclerosis have a higher incidence of the disorder, and this supports the possibility of a genetic contribution.
Genes on multiple chromosomes are suspected of playing some role in MS. People with multiple sclerosis are more likely to have abnormalities in human leukocyte antigens (HLA), proteins coded from chromosome 6 and important in the functioning of the immune system. If there is a genetic contribution to the development of MS, the path of “cause and effect” is not yet understood. There is no genetic test for multiple sclerosis, and even if there is a genetic contribution to cause, unknown environmental factors (such as a particular virus) may also play a role.
Although the primary cause of MS is not known, dysfunction in the immune system is the mechanism by which MS damages nerve tracts. Immune system cells called T lymphocytes (a type of white blood cell) attack the myelin of white matter nerve tracts while B lymphocytes damage the nerve fibers (axons) themselves. While demyelinated areas caused by T cell attack impair nerve impulse transmission, the B cell damage to axons themselves is more serious and slower to repair itself, if repair is possible.
This dual mechanism could explain the different types of MS discussed below. Relapse and remittance of MS may be caused by T cell activity and progression may be caused by B cell activity. All of the answers will have to await future research.
Types of Multiple Sclerosis
Several patterns are possible in the way MS first appears and the way it manifests over time (its clinical course). A typical exacerbation (worsening) of MS lasts 2 to 4 weeks, and takes several months to resolve or improve. However, this pattern is subject to considerable individual variation.
- Relapsing-remitting MS is the most common type for which Social Security disability benefits are sought. In this form, MS first appears as a series of attacks interspersed with complete or partial improvement (remission), followed by some future relapse.
- Primary-progressive MS is characterized by a slow progression in clinical severity, although there may be minor temporary stabilization or improvement.
- Secondary-progressive MS begins as a relapsing-remitting form, then later becomes a primary-progressive form.
- Progressive-relapsing MS is characterized by worsening, with additional acute exacerbations.
Patients with particularly severe MS might be described as having “malignant MS,” while those with minimal symptoms and limitations for extended periods of time are sometimes referred to as having “benign MS.”
The course of MS can vary significantly from person to person. The Social Security Administration needs detailed medical evidence about how your illness has progressed over time to make the best disability determination.
Diagnostic Categories of Multiple Sclerosis
MS affects women more frequently than men and most often first produces symptoms in the 20 to 40 age range. Disease appearing before age 10 or after age 55 is a strong argument for some other kind of disorder. The diagnosis of MS is still fundamentally clinical—a judgment based on your doctor’s evaluation of the history and physical examination, severity of signs and symptoms over time, and test evidence. The diagnosis cannot be made based on laboratory results alone, and there are no physical abnormalities unique to MS.

Signs and Symptoms of Multiple Sclerosis
There are a large number of possible signs and symptoms of MS. Some patients have no signs or symptoms. The major possibilities are as follows:
- Muscle weakness sometime associated with muscle atrophy.
- Spasticity (uncontrolled muscle contractions) – chronic spasticity can impair gait or use of arms; sudden spasms (paroxysmal dystonia) in arms or legs may occur with changes in posture or even certain kinds of sensation.
- Impairment of pain, temperature, and touch senses – burning, itching, decreased sense of limb position, decreased touch or temperature sensation, etc.
- Pain (moderate to severe) – sharp pains, including severe facial nerve pain (trigeminal neuralgia).
- Ataxia – impaired ability to coordinate movement can range from mild to severe.
- Impaired balance.
- Tremors.
- Decreased dexterity – impairment of fine manipulatory ability.
- Speech disturbances – decreased clarity of articulation (dysarthria) caused by slurring, dyscoordinated speech (speech ataxia), “scanning,” i.e., with unnatural pauses and skipped sounds that result in a staccato-like delivery.
- Aphasia – difficulty in instigating speech, understanding writing, understanding spoken words, etc.
- Vision disturbances – paralysis of eye movement and pupillary function (internuclear ophthalmoplegia); double vision (diplopia), blurry vision (optic neuritis), abnormal eye movements (nystagmus); visual field loss is possible but unusual; color vision sensitivity may be decreased, Uhtoff’s phenomenon may occur (visual blurring after exertion or heat exposure).
- Vertigo – dizziness may be intense, with associated nausea and vomiting; caused by inflammation of the vestibular nerve (vestibular neuronitis).
- Bladder dysfunction – a common problem that may be urge incontinence, frequency, or decreased bladder sensation resulting in overflow incontinence.
- Bowel dysfunction – constipation is common; loss of sensation near the anal sphincter may result in bowel incontinence.
- Sexual dysfunction – frequently present as decreased libido in both sexes; erectile dysfunction in men; decreased vaginal lubrication in women.
- Depression and anxiety – resulting from poor self-image, sexual dysfunction, worry about spousal rejection, and the debilitating nature of chronic disease.
- Euphoria.
- Seizures.
- Cognitive (rational thinking) abnormalities –present in 40–70% of MS cases but profound mental impairment is uncommon.
- Fatigue – easy fatigability is associated with both physical and mental activity, and not necessarily associated with obvious physical impairment or depression.
- Exacerbation with exertion or exposure to heat.
- Multiple sclerosis may produce findings of both upper and lower motor neuron syndrome, depending on location of the lesions.
Treatment of Signs and Symptoms of MS
Each of the signs and symptoms of MS may require separate treatment. For example, antiepileptic drugs (AEDs) would be required to control seizures and are also helpful in the treatment of the exquisitely painful disorder known as trigeminal neuralgia. Spasticity may be helped by muscle relaxants such as Baclofen (Lioresal), diazepam (Valium) and other drugs. Optic neuritis is treated with corticosteroids like prednisone or intravenous methylprednisolone. Pain may require analgesic or antidepressant medication. A number of different agents have been used to treat fatigue, such as amantadine (Symmetrel), pemoline (Cylert), and antidepressants. Self-injected papaverine in the corpus cavernosum of the penis can help temporarily reverse erectile dysfunction. There are also drugs that can help inhibit an over-active bladder, such as dantrolene (Dantrium).
In addition to drugs, physical therapy, occupational therapy, speech therapy, or psychiatric therapy may be needed in individual cases as appropriate.
Current Therapies for Multiple Sclerosis
Therapeutic Goals
The goals of therapy for MS are threefold: to improve recovery from attacks, to prevent or lessen the number of relapses, and to halt disease progression. Numerous therapies have been tried, but so far, treatment of multiple sclerosis designed to cure or stop disease progression has failed.
Therapies for MS under investigation include various treatments to alter or suppress the immune system, therapies to improve nerve impulse conduction, and therapies to reverse the damage to myelin and oligodendrocytes (the cells that make and maintain myelin in the central nervous system).
Many patients do well with no therapy, especially since many medications have serious side effects and some carry significant risks.
Steroids
Until recently, the principal medications used to treat MS were steroids possessing anti-inflammatory properties; these include adrenocorticotropic hormone (ACTH), prednisone, prednisolone, methylprednisolone, betamethasone, and dexamethasone. While steroids do not affect the course of MS over time, they can reduce the duration and severity of attacks in some patients. The mechanism behind this effect is not known. Because steroids can produce numerous adverse side effects (acne, weight gain, diabetes, seizures, hypertension, cataracts, osteoporosis, psychosis), they are not recommended for long-term use.
Interferons
One of the most promising MS research areas involves naturally occurring antiviral proteins known as interferons. Three forms of beta interferon (Avonex, Betaseron, and Rebif) have been approved by the Food and Drug Administration for treatment of relapsing-remitting MS. Beta interferon has been shown to reduce the number of exacerbations and may slow the progression of physical disability. When attacks do occur, they tend to be shorter and less severe. In addition, MRI scans suggest that beta interferon can decrease myelin destruction. However, if a patient develops neutralizing antibodies to a therapeutic drug then its effectiveness will be reduced. Once neutralizing antibodies have appeared, it does no good to switch to another type of beta interferon since the antibodies associated with the three different drugs cross-react. Common side effects of interferons include fever, chills, sweating, muscle aches, fatigue, depression, and injection site reactions.
Fingolimod
An immunomodulating agent known as fingolimod has much less prominent side effects than interferons and can be taken orally. Fingolimod is aimed at treating relapsing MS, and initial trials show a low relapse rate with continuous oral maintenance, decreased symptoms, and decreased number of lesions on magnetic resonance imaging of the brain. Fingolimod has not been approved by the FDA for human treatment outside of clinical trials. However, there is a good chance fingolimod will turn out to be a useful agent.
Natalizumab
A drug known as natalizumab was approved for treating multiple sclerosis in 2004. Natalizumab decreases the ability of white cells to enter the central nervous system. In 2005, use of the drug had to be suspended due to the risk of a rare but fatal disease known as progressive multifocal leukoencephalopathy (PML). Also, other serious problems such as hypersensitivity reactions can develop. In 2006, the drug was again approved, but only for restricted use in relapsing multiple sclerosis. Patients with progressive MS are not treatable with this drug at the present time. Treatment with natalizumab must be given intravenously on a monthly basis at a special infusion centers.
The significance of a person receiving natalizumab is two-fold for disability adjudication:
- The diagnosis must be very secure for the drug to be used; this should suggest to the adjudicator that the claimant has MS beyond any reasonable doubt.
- The drug is dangerous; it can be cleared for use only when severe relapsing MS has not responded to other treatments.
Therefore, if you are receiving this drug for treatment of MS, it should be a red flag to the Social Security Administration adjudicator to allow your case when the medical evidence is developed. If the medical evidence does not support an allowance, there is almost certainly a deficiency in the development of that evidence. Even if you have seemingly improved on natalizumab, exceptionally careful consideration of the evidence should be done before concluding that you have achieved a steady-state of improvement that would permit sustained substantial gainful activity.
Winning Social Security Disability Benefits for Multiple Sclerosis by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your multiple sclerosis is severe enough to meet or equal the MS listing. The Social Security Administration has developed a set of rules called Listing of Impairmentsfor most common impairments. The listing for each impairment describes a degree of severity that the Social Security Administration presumes would prevent a person from performing substantial work. If your MS is severe enough to meet or equal the listing, you will be eligible for disability benefits.
The listing for multiple sclerosis is 11.09, which has three parts: A, B, and C. You will be eligible for disability benefits if you meet any part.
Meeting Social Security Administration Listing 11.09A for Multiple Sclerosis
You will meet Listing 11.09A and qualify for social security disability benefits if you have multiple sclerosis with disorganization of motor function as described in listing 11.04B. Listing 11.04B requires significant and persistent disorganization of motor function in two extremities, resulting in sustained disturbance of gross and dexterous movements, or gait and station.
MS is characterized by exacerbations that vary in frequency, character, severity, and duration. Remissions vary in degree of recovery and duration. The Social Security Administration should consider the course of the disease process during the few years preceding your application for benefits. An attempt should be made to decide if your case under consideration has developed a specific course. However, if you have had two or more severe exacerbations in a year, which prevent any work for more than 1 month, you would be found to have an impairment which meets the listing.
Two Extremities Must Be Impaired
The two major areas of motor limitations are:
- Upper extremity (arm and hand) function including:
- Gross movements.
- Dexterous movements.
- Lower extremity (leg) function including:
- Gait – the manner of walking.
- Station – the manner of standing, i.e., ability to maintain a posture.
Two extremities must be involved to satisfy part A of the MS listing: both legs, both arms, or one arm and one leg.
If a lower extremity alone (i.e., a single leg) is affected, the listing cannot be met. However, if the lower extremity is so weak that a hand-held assistive device such as a quad cane is necessary for walking, then use of an arm would be tied up with the same functional result as paralysis of the arm. Such cases would equal the listing.
If you cannot stand and walk 6 to 8 hours daily and have any significant weakness or inability to manipulate objects with an upper extremity, the listing is satisfied. Inability to stand or walk for such prolonged times does not necessarily depend only on lower extremity strength. An uncoordinated gait, or poor balance that results in an unreasonably slow pace would meet the listing. This is particularly important if you have neurological dysfunction in both lower extremities, but not in the arms.
Evaluating Strength
At a physical examination, a doctor can obtain information regarding strength in the upper and lower extremities with some simple and routine maneuvers. First, the examining physician can estimate strength loss by comparing the strength of muscle contraction on your the weak side to your normal side.
Physicians frequently report subjective determination of strength by using a scale of 0 to 5 with 5 being normal. For example a doctor might ask you to try to straighten out your leg while the doctor resists such movement. A weaker leg might be reported as 3/5 for the quadriceps muscle (muscle on the front of the thigh) compared to an expected normal of 5/5. Zero means no movement. One means a trace of movement. Two means movement with the help of gravity. Three means movement is possible against gravity, but not against resistance. Four means movement against gravity and resistance by the examining physician. Five means normal.
Errors in this type of subjective testing can be caused by the person’s motivation, variations among people in “normal” strength, and differences in the doctor’s subjective assessment.
More objectively, a doctor can test your ability to walk on your heels and toes and squat and arise. Ability to walk on the toes means you can lift your body weight by contraction of your gastrocnemius (calf) muscles and implies significant strength. Ability to walk on the heels indicates that the muscles in the front leg (opposite the calf muscles) that flex the foot still have good strength. Ability to squat and arise implies good strength of the quadriceps muscles of the thighs.
Determination of lower extremity strength is very important, because if you cannot stand 6 to 8 hours a day and an upper extremity is significantly affected, then the listing will be fulfilled. If you cannot stand or walk 6 to 8 hours a day, you can do only sedentary work, but if you also have limited use of an upper extremity, you cannot even do sedentary work. If you cannot walk on heels or toes in the affected lower extremity, it is not reasonable to expect that you would have the strength to stand 6 to 8 hours daily. If you can do such testing well, it is not likely you will qualify under listing 11.09A on the basis of strength deficit. However, you still may qualify based on severe lack of balance or coordination in walking.
Evaluating Walking and Balance
In evaluating how well you stand and walk, the Social Security Administration requires a detailed description from a medical doctor. This involves factors such as how weak your legs are, how much difficulty you have in keeping your balance, how fast you walk, how much help you need walking, and so forth. To meet the listing, you do not have to use a cane, crut ch, brace, walker, or other assistive device to move about. Of course, if you need such devices, that would indicate a very severe limitation. However, the use of an assistive device such as a cane or crutch, or even a wheelchair, does not establish a severe limitation without supporting objective medical data. This is true, even if your treating doctor says you need the device.
Evaluating Arm and Hand Use
The use of the arms and hands is evaluated by looking at gross and dexterous movements. Dexterous movements are those like writing, picking up small objects, or other types of fine movements. Gross movements involve larger motions with the arms and hands. Movements can be influenced by weakness, or loss of control over the way an arm or hand moves, such as tremors or poor coordination. The ability to oppose fingertips to the thumb successively can give some idea as to the intactness of fine manipulatory (dexterous) ability. However, if you can do finger-thumb opposition only slowly and clumsily, then you should not be considered capable of dexterous movements. Also, your activities of daily living (ADLs) can be helpful in assessing functional severity when they describe specific inabilities or abilities (e.g., turning doorknobs, dressing, climbing stairs, shaving, etc.).
Meeting Social Security Administration Listing 11.09B for Multiple Sclerosis
Part B states that visual disorders are to be evaluated under the appropriate visual impairment listings, and mental disorders under the appropriate mental impairment listings. Concerning mental disorders, note that part B only refers to listing 12.02 for organic brain syndrome. This is a peculiar omission of mental disorder listings that involve depression and anxiety, but there is no reason you cannot be evaluated under whatever mental disorder listing, or combination of listings, is appropriate.
Meeting Social Security Administration Listing 11.09C for Multiple Sclerosis
You will meet Listing 11.09C and qualify for social security disability benefits if you have multiple sclerosis and:
- Significant, reproducible fatigue of motor function with
- Substantial muscle weakness on repetitive activity, that is
- Demonstrated on physical examination,
- Resulting from neurological dysfunction in areas of the central nervous system known to be pathologically involved by the multiple sclerosis process.
Part C attempts to take into account easy fatigability caused by multiple sclerosis, although brief muscle strength on testing may be normal. There are several problems with part C that make it difficult to use by Social Security Administration adjudicators.
Part C refers to increased muscle weakness detected on physical examination, as measured by repetitive activity. Required would be some type of repetitive effort against a measurable resistance, such as moving a given weight through a given distance a given number of times, or measurement of grip strength force to see if it decreases with repetition. No test is meaningful without standardization. The Social Security Administration has never offered any testing guidelines for objectively measuring fatigability in multiple sclerosis.
Part C also requires that the easy fatigability be related to areas of the brain that have been demonstrated to be involved with multiple sclerosis. Yet, one cannot correlate the areas of abnormality on a MRI brain scan with fatigue. While fatigue may affect a specific limb when associated with muscle weakness, fatigue usually affects the entire body. It cannot easily be separated out into pieces.
In the evaluation of fatigue in MS, the Social Security Administration provides a medical policy explanation which states:
“Fatigue can be a factor in individuals with MS. However, fatigue is difficult to assess because, … there are no objective tests to measure it. The individual must demonstrate some objective ongoing neurological deficit; a claim cannot be allowed on the basis of fatigue alone. Clinical and laboratory data and a well-documented medical history must establish findings which may reasonably account for fatigue.
“The best means of assessing fatigue is by inference in terms of documentation of the claimant’s activities of daily living, the extent of physical activity before fatigue occurs, and the frequency at which the claimant requires periods of rest. Individuals either living with the claimant (e.g., spouse, son, daughter) or individuals in close contact with the claimant should be good sources of such information. After such information is obtained, an inference in terms of documentation of the claimant’s activities of daily living to see what effect fatigue plays in his or her overall physical activities should be made. However, conclusions about the intensity and persistence of fatigue and the effect on the person’s work capacity must be drawn from the clinical and laboratory data and other evidence. In effect, a judgment is required as to whether findings relative to fatigue are consistent with the clinical course of the disorder and substantiated by the medical and other evidence. A judgment must be made on an individual case-by-case basis.”
Rather than disregarding part C because of its impossible requirement that damaged brain (or spinal cord) areas match manifestations of fatigue, a finding that you equal the listing whenever the Social Security Administration policy is otherwise satisfied. There is no doctor on earth who can correlate particular brain lesions with fatigue in MS.
Residual Functional Capacity Assessment for Multiple Sclerosis
What Is RFC?
If your multiple sclerosis is not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary workin spite of your impairments. The lower your RFC, the less the Social Security Administration believes you can do.
Limitations on Lifting and Walking
When assessing your RFC, the Social Security Administration should consider the weight that you are able to lift and carry. To be able to do medium work, which requires you to lift and carry up to 50 lbs and stand and walk 6 to 8 hours daily, you should have no more than very modest deficits in strength, coordination, and balance.
If you have some difficulty in walking on your heels and toes, or squatting and arising, during medical examination, you might still be able to do light work (lifting no more than 20 lbs and still standing and walking 6 to 8 hours daily). But you probably would not realistically be able to do even light work if you cannot walk on your heels and toes while carrying no weight during a physical.
In evaluating upper extremity function, the Social Security Administration should consider whether you have insufficient strength to operate arm or leg controls more than occasionally in the affected limbs.
Of course, all factors have to be considered: whether your muscles appear weak and limp on exam or spastic (in spasm), whether you are overweight etc. Thus, your RFC could be reduced to sedentary work requiring no more than 2 hours standing and walking daily. If you also have significant upper extremity dysfunction, you would be disabled under a listing.
If both your legs are impaired, and your upper extremities are functionally intact, the impairment will meet Listing 11.09A and you will be disabled if your gait and station are impaired to a significant degree—that is, if you cannot stand and walk 6 to 8 hours daily, and you have a problem standing because of balance sufficient for sedentary work. If gait and station are fully functional for sedentary work, except for enough stamina or strength to stand and walk for more prolonged periods, and your upper extremity function is fully intact, then you are capable of a sedentary work RFC.
Limitations on Activities of Daily Living
You—or family members—should be asked in detail about your ability to carry out activities of daily living (ADL). Of particular interest is your ability to walk up and down steps, the speed at which you walk, and how easily you tire. If you cannot walk a block, you certainly cannot stand and walk 6 to 8 hours daily. You should also be asked what tasks you could do before your stroke that you cannot do now. Can you dress without assistance? Manipulative functions are important. Can you turn a doorknob? Can you pick up coins and button shirts?
High-quality description of your ADLs is very important.
Other Issues Relevant to the Listings and RFC
Certain important issues should also be kept in mind regarding meeting or equaling the listing, or determination of RFC:
- The Social Security adjudicator is likely to under-rate allegations of fatigue.
- The Social Security adjudicator may fail to develop your claim for a mental impairment, unless you specifically mention in your application for social security disability benefits that you are depressed. Because of the frequent presence of depression in MS, failure to ask the claimant specifically about depression or other mental problems is a mistake.
- The Social Security adjudicator may not be aware that exertion can increase the severity of MS signs and symptoms, quite apart from the issue of fatigue.
- The Social Security adjudicator is very likely to be unaware that hot environments, or getting hot from overexertion, can precipitate a worsening of signs and symptoms in MS. Consequently, appropriate environmental restrictions, such as avoiding work at temperatures over 75° F, are not given.
- The Social Security adjudicator may not appreciate the overall severity of a combination of impairments that should result in a finding of equivalent severity to the listing.
- The Social Security adjudicator is likely to not adequately appreciate the debilitating effect of severe bowel or bladder incontinence.
Getting Your Doctor’s Medical Opinion About What You Can Still Do
The Social Security Administration’s job is to determine if you are disabled, a legal conclusion based on your age, education and work experience and medical evidence. Your doctor’s role is to provide the Social Security Administration with information concerning the degree of your medical impairment. Your doctor’s description of your capacity for work is called a medical source statement and the Social Security Administration’s conclusion about your work capacity is called a residual functional capacity assessment. Residual functional capacity is what you can still do despite your limitations. The Social Security Administration asks that medical source statements include a statement about what you can still do despite your impairments.
The Social Security Administration must consider your treating doctor’s opinion and, under appropriate circumstances, give it controlling weight.
The Social Security Administration evaluates the weight to be given your doctor’s opinion by considering:
- The nature and extent of the treatment relationship between you and your doctor.
- How well your doctor knows you.
- The number of times your doctor has seen you.
- Whether your doctor has obtained a detailed picture over time of your impairment.
- Your doctor’s specialization.
- The kinds and extent of examinations and testing performed by or ordered by your doctor.
- The quality of your doctor’s explanation of your impairment.
- The degree to which your doctor’s opinion is supported by relevant evidence, particularly medically acceptable clinical and laboratory diagnostic techniques.
- How consistent your doctor’s opinion is with other evidence.
When to Ask Your Doctor for an Opinion
If your application for social security disability benefits has been denied and you have appealed, you should get a medical source statement (your doctor’s opinion about what you can still do) from your doctor to use as evidence at the hearing.
When is the best time to request an opinion from your doctor? Many disability attorneys wait until they have reviewed the file and the hearing is scheduled before requesting an opinion from the treating doctor. This has two advantages.
- First, by waiting until your attorney has fully reviewed the file, he or she will be able to refine the theory of why you cannot work and will be better able to seek support for this theory from the treating doctor.
- Second, the report will be fresh at the time of the hearing.
But this approach also has some disadvantages.
- When there is a long time between the time your attorney first sees you and the time of the hearing, a lot of things can happen. You can improve and go back to work. Your lawyer can still seek evidence that you were disabled for a certain length of time. But then your lawyer will be asking the doctor to describe your ability to work at some time in the past, something that not all doctors are good at.
- You might change doctors, or worse yet, stop seeing doctors altogether because your medical insurance has run out. When your attorney writes to a doctor who has not seen you recently, your attorney runs the risk that the doctor will be reluctant to complete the form. Doctors seem much more willing to provide opinions about current patients than about patients whom they have not seen for a long time.
Here is an alternative. Suggest that your attorney request your doctor to complete a medical opinion form on the day you retain your attorney. This will provide a snapshot description of your residual functional capacity (RFC) early in the case. If you improve and return to work, the description of your RFC provides a basis for showing that you were disabled for a specific period. If you change doctors, your attorney can get an opinion from the new doctor, too. If you stop seeing doctors, at least your attorney has one treating doctor opinion and can present your testimony at the hearing to establish that you have not improved.
If you continue seeing the doctor but it has been a long time since the doctor’s opinion was obtained, just before the hearing your attorney can send the doctor a copy of the form completed earlier, along with a blank form and a cover letter asking the doctor to complete a new form if your condition has changed significantly. If not, your attorney can ask the doctor to send a one-line letter that says there have been no significant changes since the date the earlier form was completed.
There are times, though, that your attorney needs to consider not requesting a report early in the case.
- First, depending on the impairment, if you have not been disabled for twelve months, it is usually better that your attorney wait until the twelve-month duration requirement is met.
- Second, if you just began seeing a new doctor, it is usually best to wait until the doctor is more familiar with your condition before requesting an opinion.
- Third, if there are competing diagnoses or other diagnostic uncertainties, it is usually best that your attorney wait until the medical issues are resolved before requesting an opinion.
- Fourth, a really difficult judgment is involved if your medical history has many ups and downs, e.g., several acute phases, perhaps including hospitalizations, followed by significant improvement. Your attorney needs to request an opinion at a time when the treating doctor will have the best longitudinal perspective on your impairment.

