How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Ischemic Heart Disease?
If you have ischemic heart disease, Social Security disability benefits may be available to you. To determine whether you are disabled by your ischemic heart disease, the Social Security Administration considers whether your heart disease is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing. If you meet or equal a listing because of ischemic heart disease, you are considered disabled.
If your ischemic heart disease is not severe enough to equal or meet a listing, the Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your heart disease), to determine whether you qualify for disability benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Ischemic Heart Disease.
About Ischemic Heart Disease and Disability
What Is Ischemic Heart Disease?
Ischemic heart disease (IHD) is a major medical problem disabling and killing millions of people in the U.S. yearly, and therefore a frequent basis for allegations of disability. Heredity plays an important role, but so does lifestyle. Many IHD deaths are preventable and associated with poor control of hypertension and diabetes mellitus, smoking, lack of exercise, obesity, and poor diet resulting in elevated blood lipids (fats such as cholesterol).
Ischemia means that the heart (or other body tissue) is not receiving enough oxygen to function normally. The oxygen demands of the heart change with heart rate (see Figure 1 below). So increased heart rates require increased blood flow to the heart to deliver the oxygen and glucose needed for the extra work. Ischemia not present at rest may appear when the heart rate increases, and this is the basis for cardiac stress testing. See Cardiac Stress Testing.
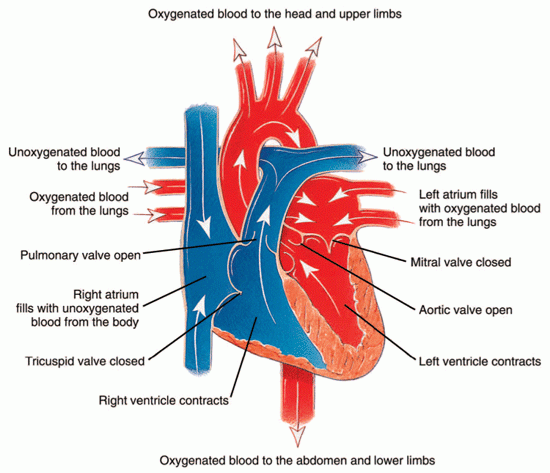
Figure 1: The path of oxygenated and unoxygenated blood in the heart during contraction.
Causes of Ischemic Heart Disease
Most IHD results from obstruction of the coronary arteries that supply the myocardium (heart muscle) with blood. This condition is known as coronary artery disease (CAD). Other cardiac abnormalities can also cause myocardial ischemia. The underlying mechanism is still the same: restriction of blood flow to the myocardium. For example, marked narrowing of the aortic valve (aortic stenosis) (see Figure 2 below) can cause angina (chest pain) because the coronary arteries originate right above the valve (see Figure 3 below) and may not receive sufficient blood flow to supply the heart. However, the great majority of claimants have myocardial ischemia because of CAD.
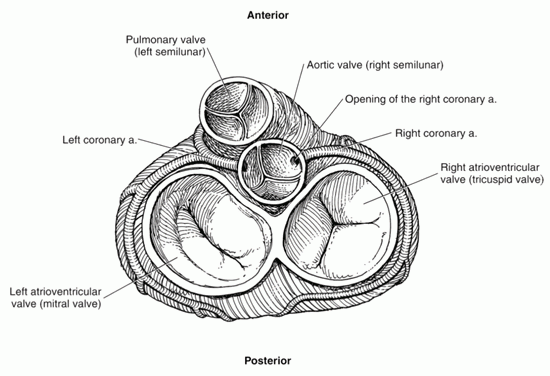
Figure 2: Closed heart valves.
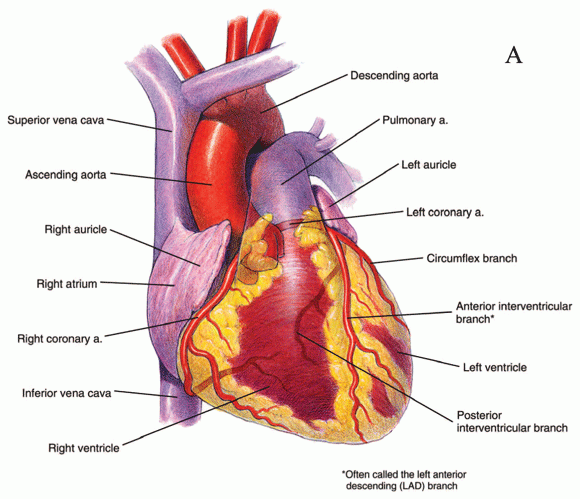
Figure 3: Anterior view of the heart, including main arteries.
How Severe Does Coronary Artery Disease Have to Be to Produce Ischemia?
Blood flow to the myocardium served by a particular coronary artery is not significantly decreased until a lesion blocks about 70% of the diameter of the artery. It is frequently possible for a person to be comfortable at rest with a 90% blockage in a large epicardial artery.
Lesions of less than 50% are generally considered to not be significant CAD, because the heart will still be able to obtain sufficient blood flow both at rest and with exercise. However, this conclusion must be made in context of all of the medical evidence. Long segments of obstruction rather than discrete lesions, involvement of the left main coronary artery, or involvement of multiple arteries could cause significant ischemia with blockages as low as 50%.
Detecting Ischemia
Ischemia can be indicated by:
- Electrocardiograms (ECGs, ECGs);
- Imaging studies that show the movement of the cardiac ventricular walls;
- Imaging studies that show relative blood flow within the heart muscle; and
- Imaging studies that measure amounts of blood moved by the heart’s ventricles.
Cardiac Stress Testing
Cardiac stress testing raises heart rate to determine:
1) Whether ischemia can be induced,
2) The level of exertion producing ischemia, and
3) The severity and location of the ischemia.
Cardiac stress testing is also used to determine the exercise capacity of individuals in regard to physical conditioning, but the Social Security Administration never purchases testing for that purpose alone.
The only type of cardiac stress testing mentioned by the Social Security Administration is exercise stress testing, in which physical exertion is used to raise the patient’s heart rate.
In exercise stress testing, your baseline ECG is obtained. Then you begin with a low level of exercise, either by walking on a treadmill, or pedaling a stationary bicycle. Every two to three minutes, the level of exertion is increased. At each stage of exercise, your pulse, blood pressure and ECG are monitored are recorded, along with any symptoms you may be experiencing.
The exertion level is gradually increased every 2 to 3 minutes until you cannot keep up any longer, or until your symptoms (chest pain, shortness of breath, or lightheadedness) prevent further exercise, or until changes on your ECG indicate a cardiac problem.
There are other means of raising heart rate for testing purposes, such as pharmacologic stress testing in which drugs are used to raise the heart rate. Pharmacologic stress testing can be used with patients who, for some reason, cannot perform exercise stress testing.
Both exercise testing and pharmacologic testing can be used in conjunction with various types of imaging studies of the heart’s response to increased heart rate—such as radionuclide scans or echocardiograms that are done at the same time.
Left Ventricular Ejection Fraction
The most important performance test for blood moved by cardiac ventricles (see Figure 4 below) is the percentage of blood pumped out of the left ventricle (LV) with each beat—the left ventricular ejection fraction (LVEF). The left ventricle is of major interest, because it pumps blood into the systemic circulation that supplies the tissues of the body and is the major site of damage by ischemic heart disease, such as heart attacks.
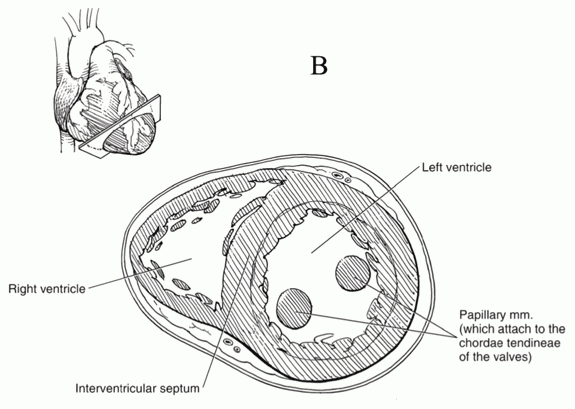
Figure 4: Cross-section of the ventricles of the heart, which are important to blood movement.
The LVEF is normally about 55-65%, and is not usually considered abnormal unless it falls under 50%.
Angina Pectoris and Ischemic Heart Disease
What is Angina Pectoris?
When the myocardium receives inadequate blood flow, sensory nerve fibers (cardiac afferents) from the heart to the brain carry impulses for pain known as angina pectoris. The Social Security Administration also refers to angina as “chest discomfort of myocardial ischemic origin.”
In a significant number of people with myocardial ischemia, the pain activation system is defective for no obvious reason. These people have no warning when blood flow to the heart is inadequate and they are at particular risk for sudden death. Without warning pain, such individuals may continue to exercise after the onset of ischemia. Ischemic heart muscle is electrically unstable, so that it carries an increased risk of a lethal arrhythmia.
Angina and Disability
Angina is relevant to disability determination. To meet the listing for ischemic heart disease, you must have symptoms due to myocardial ischemia. See Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing. Angina is one such symptom. See Symptoms Due to Myocardial Ischemia.
Angina is also relevant to disability determination because chest pain limits exertion. In disability adjudication, the Social Security Administration frequently must evaluate the status of claimants after a myocardial infarction. See Heart Attacks (Myocardial Infarctions or MIs).
Many allege chest pain that may or may not be of cardiac origin.
However, there are too many unknown variables, conflicting descriptions, and other confounding factors to use the absence or presence of chest pain—even classic, angina-compatible chest pain—as controlling either treatment or disability decision-making.
Objective Data Are Necessary for Diagnosis of Angina
Objective data (test results) supporting the angina diagnosis are necessary. A diagnosis of angina based on a patient’s description alone is not reliable. Many claimants who describe chest pain that could be angina based on the description they provide (angina-compatible chest pain), turn out to have nothing wrong with their hearts after thorough examination.
A number of medical conditions can cause chest pain closely resembling angina. Esophageal spasm, for example, can feel just like angina—even be relieved with drugs used to treat angina—except for one thing: the absence of relation to exertion. A good history of chest pain that covers the possible non-cardiac types of pain requires a careful approach and professional medical training. Shortness of breath may occur with angina, but shortness of breath alone is not angina.
The Social Security Administration must obtain cardiac exercise testing on claimants with angina-compatible chest pain when there is no other means of allowance and there is no contraindication to such testing. See Cardiac Stress Testing.
Characteristics of Angina
Angina is described in terms of:
- Location,
- Quality,
- Precipitating causes,
- Duration, and
- Mode of relief.
The general characteristics of these factors are as follows:
Location – Central Chest (Substernal)
Angina pain sometimes radiates down one or both arms or up into the neck or jaw. Angina is much less likely if the pain is only outside of the central chest area, such as in the jaw alone, or abdomen. Pain in a small area on the side of the chest is probably not angina. The more unusual the location of pain, the less likely that angina is actually the cause. However, if other characteristics fit the diagnosis of angina then it should be accepted despite an atypical location—especially if there is objective evidence of significant ischemic heart disease. In fact, the Social Security Administration is willing to accept atypical locations—even pain isolated to a hand, jaw, or neck—if everything else fits the angina diagnosis.
Quality – Dull, Aching, Squeezing, Heavy
Most claimants describe their pain as “sharp.” For some reason, this is the first word that enters the mind for many people when asked the quality of a pain. Therefore, a diagnosis of angina should not be discarded because a claimant uses the word “sharp.” Less-educated claimants are particularly likely to use words for the quality of chest pain that actually do not describe what they are experiencing. Because of the subjective nature of “quality”—what something feels like—the Social Security Administration adjudicator should only reject the characteristic if the quality described is something that is never associated with angina.
Rhythmic pain is never angina. Rhythmic pain is something that rapidly varies in intensity, especially stabbing, jabbing and poking sensations that quickly come and go (also see the discussion of Duration below). It is important for the interviewer to carefully communicate with the patient in this regard to make sure that there is mutual understanding of the meaning. For example, sticking or “pins-and-needles” sensations are also not compatible with angina.
Precipitating Causes – Exertion, Emotion
Exertion and emotion (excitement, anxiety, fear) raise heart rate, which can induce cardiac ischemia and the onset of ischemic chest pain—angina. Chest pain that always occurs with particular activities, such as walking a certain distance or climbing a certain number of stairs is characteristic of angina.
Chest pain with exertion does not always indicate angina. Chest pain that occurs randomly, sometimes during exertion and sometimes during rest, does not suggest ischemia since the cause-and-effect element is missing.
Chest pain associated with emotion, but occurring at rest, could be angina. On the other hand, chest pain that occurs only with emotion and not with exertion is suspect for being of non-cardiac origin.
Although there should be a general cause and effect relationship between angina and exertion or emotion, that does not mean that angina will always occur at a specific level of exertion since multiple factors (e.g., emotional state, physical health, drugs, temperature) can influence it. The absence of chest pain during exercise testing is not sufficient, in itself, to rule out ischemic heart disease. Nor is it sufficient to eliminate a claimant’s subjective report of chest pain during activities of daily living from consideration. Also, some individuals may show evidence of ischemia during stress testing, but have no pain.
Ischemia and reported symptoms are not predictably associated. Similarly, ischemia at any particular level of exercise cannot be closely predicted on the basis of the underlying coronary artery lesions.
The important piece of information needed for either treatment or disability determination is objective, exercise-induced ischemia.
Vasospastic Angina
There is an important exception to the relationship between exertion and ischemic cardiac chest pain: vasospastic angina (variant angina) occurs when a coronary artery narrows in a particular location, thereby decreasing blood flow to heart muscle past the point of narrowing. The word “vasospastic” means that the narrowing is temporary, and usually results from some irritative focus that causes the smooth muscle inside the coronary artery to constrict at a specific place. The irritative focus is something that triggers the muscle spasm and that is often the fibro-fatty, sometimes calcified, plaque of coronary artery disease.
Drugs like cocaine are particularly likely to induce coronary artery spasm. In fact, cocaine can cause such severe constriction that blood flow is completely cut off to an area of the heart, with a resultant heart attack in a young person who would otherwise not have such an event. The risk is probably even greater for a middle-aged person who already has an irritative focus like a fatty lesion in a coronary artery and then also takes cocaine.
Angina in the Resting State
It is possible to have cardiac ischemia so severe that angina occurs in the resting state. But these people are so ill that they have been evaluated for heart disease by their treating physicians and severe abnormalities have been documented. Angina occurring in the resting state either results in medical treatment or death. No one with angina at rest is going to be in that state very long without medical care. Furthermore, angina in such cases will still be characteristically precipitated by exertion and worsened by exertion, so that important cause-and-effect relationship is still intact.
Duration
Typical angina lasts only a couple of minutes after the precipitating cause is stopped. It is quite common for claimants to say that their chest pain lasts for hours at a time on a regular basis. This is not anginal chest pain. Chest pain lasting for hours is more compatible with a heart attack than angina. Even if a person has particularly severe and worsening angina—a condition known as unstable angina—there is no way such prolonged angina could be occurring on a regular basis, because the individual would be dead or in a hospital.
Attempting to continue exertion with angina will cause further worsening until the person stops the inducing activity, which will happen quickly after the onset of pain; no one ignores angina.
Chest pain lasting less than a minute is usually not angina. Chest pain lasting less than 10 seconds or more than 30 minutes would be considered non-anginal by most cardiologists. In the unusual cases in which 30 minute durations are caused by ischemic heart disease, they are more characteristic of unstable angina, than typical angina. Unstable angina is a serious condition and not something a person has very long without coming under medical care. Nevertheless, the Social Security Administration is usually generously flexible in this regard. If all of information is supportive of the diagnosis, durations of up to 30 minutes will generally be accepted in disability determination as angina, rather than requiring a more realistic 3 to 5 minutes of duration. Perhaps this is because the Social Security Administration realizes that many people are poor at estimating the time their chest pain lasts. Of course, the optimum situation is one in which patients have actually measured the duration of pain after cessation of the precipitating cause, but claimants usually have not done so.
Relief of Angina
Angina caused by exertion is relieved by rest; emotionally induced angina is relieved by lessened emotional arousal.
A number of long-acting drugs improve cardiac ischemia and decrease the over-all frequency and severity of anginal attacks. For example, beta-blocker drugs like propranolol will keep the exertional and emotional heart rate down. Long-acting nitrates will help keep coronary arteries widened to maximize blood flow.
Treatment of high blood pressure (HBP) will decrease the work the heart has to do and therefore improve angina.
Nitroglycerin taken as a small white tablet dissolved under the tongue (not swallowed) has long been a standard treatment for acute relief of angina by dilating coronary arteries. Nitroglycerin will typically relieve angina in 30 seconds to several minutes. Unfortunately, nitroglycerin tablets also relieve the non-cardiac pain of esophageal spasm—a common disorder—so that an improvement with nitroglycerin, which is suggestive of possible angina, is not diagnostic.
Syndrome X
Syndrome X refers to angina-compatible chest pain in people with normal epicardial coronary arteries. Around 10% to 20% of individuals with angina-compatible chest pain have normal epicardial coronaries. The dilemma is determining which ones have some true cardiac basis for such pain (Syndrome X) and which have some other physical disorder or psychiatric impairment.
Unlike classic angina (associated with ischemia from epicardial artery obstructions) and vasospastic angina (associated with ischemia from reversible epicardial artery spastic narrowing), individuals with Syndrome X have no obvious cause of ischemia to explain their chest pain symptoms. Some of these individuals have objective evidence of ischemia on exercise test ECGs, as well as on radionuclide scans for cardiac ischemia and positron emission tomographic (PET) scans.
Individuals with Syndrome X are speculated by some authorities to have microvascular angina resulting from spasms in the smaller arteries (see Figure 5 below) within the heart muscle (intra-myocardial arteries), or perhaps an inability of these arteries to adapt to needed changes in blood flow. Very small coronary arteries cannot be directly visualized by coronary angiography—only the epicardial arteries and their branches.
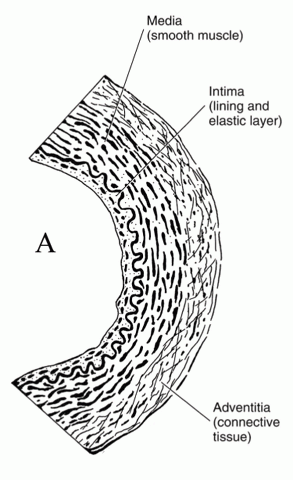
Figure 5: The micro-structure of an artery.
Some authorities believe that ischemic dysfunction in Syndrome X occurs on a cellular level that cannot be adequately categorized without even further refinement of imaging techniques to a molecular level.
The significance of Syndrome X for disability determination is that the Social Security Administration should not ignore objective evidence for cardiac ischemia because the medical evidence shows normal coronary arteries visualized by cardiac catheterization and cardiac angiography.
Some treating physicians simply speculate that a patient has Syndrome X without documenting objective evidence of ischemia. The Social Security Administration is not obligated to consider such individuals disabled on the basis of alleged symptoms alone.
There has to be some objective cardiac basis for chest pain symptoms before allowance under the listing is possible, but that evidence may take several forms and the normality of one form of evidence—such as coronary angiography of the large epicardial coronary arteries—is not sufficient basis to rule out ischemia demonstrated by other means. See Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing.
Heart Attacks (Myocardial Infarctions or MIs)
Heart attacks (myocardial infarctions, MI) result when blood flow to a part of the myocardium decreases so much that the tissue dies. Unlike ischemic tissue, infarcted tissue cannot recover. MIs may be of any size, from one so small that there is no significant long-term impairment to events involving so much heart muscle that the heart cannot pump enough blood to maintain life.
MIs killing half or more of the myocardium are not compatible with life. Fortunately, most heart attacks are much smaller.
Although MIs can affect the right ventricle of the heart, they most often occur in and damage the pumping ability of the left ventricle. If severe enough, the left ventricular ejection fraction will decrease.
In some individuals, heart attacks are so massive that cardiogenic shock develops, a life-threatening condition in which the heart’s function is not good enough to maintain blood flow. A heart attack resulting in cardiogenic shock should cause a Social Security Administration adjudicator to suspect a large heart attack occurred.
In the past, if a heart attack appeared in a claimant’s medical records, it was considered significant. However, with the development of supersensitive biochemical tests for cardiac muscle damage, even very small amounts of heart damage (as little as 1 gram of heart muscle) will give a positive test result. This means that a technical diagnosis of a MI provides little information about the amount of heart damage. The impairment could range from none to marked. This has become a real problem because of patient self-perception and the effect on employability and health insurance.
Heart attacks do not necessarily result in disability, or limitation to light or sedentary work, or the need for prolonged recuperation and rehabilitation. The Social Security Administration assumes a 3 month interval for recovery from an MI before making a disability determination. It is now known that small heart attacks reach maximum healing in about 5 weeks, and large heart attacks in about 2 months.
The concept that all heart attacks are devastating events is not correct; each case must be evaluated on its own evidence. The very sensitive troponin cardiac enzyme tests now routinely used to diagnose heart attacks will nearly double the frequency of a diagnosis of acute MI compared to the past when less sensitive tests were available. This also means much smaller volumes of cardiac damage will be detected resulting in more diagnoses of MI, which emphasizes the need for professional medical judgment in adjudicating such claims.
Winning Social Security Disability Benefits for Ischemic Heart Disease by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your ischemic heart disease is severe enough to meet or equal the ischemic heart disease listing. The Social Security Administration has developed rules called Listing of Impairments for most common impairments. The listing for a particular impairment describes a degree of severity that the Social Security Administration presumes would prevent a person from performing substantial work. If your ischemic heart disease is severe enough to meet or equal the listing, you will be considered disabled.
The listing for ischemic heart disease is listing 4.04, which has three parts, A, B, and C. To meet the listing you must satisfy any one of the three parts despite receiving prescribed treatment.
Symptoms Due to Myocardial Ischemia
To satisfy any of the three parts of the ischemic heart disease listing, you must have symptoms of myocardial ischemia. These are:
- Typical angina pectoris. This is chest pain brought on by effort or emotion and promptly relieved by rest, sublingual nitroglycerin (that is, nitroglycerin tablets that are placed under the tongue), or other rapidly acting nitrates. Typically, the discomfort is located in the chest (usually under the breast bone) and described as pressing, crushing, squeezing, burning, aching, or oppressive.
- Atypical angina. This is discomfort or pain from myocardial ischemia that is felt in places other than the chest. The common sites of cardiac pain are the inner left arm, neck, jaw, upper abdomen, and back, but the discomfort or pain can be elsewhere. To represent atypical angina, your discomfort or pain should have precipitating and relieving factors similar to those of typical chest discomfort.
- Anginal equivalent. This means shortness of breath (dyspnea) on exertion without chest pain or discomfort. Your shortness of breath should have precipitating and relieving factors similar to those of typical chest discomfort. In these situations, it is essential to establish objective evidence of myocardial ischemia to ensure that you do not have effort dyspnea due to non-ischemic or non-cardiac causes.
- Variant angina. Variant angina (Prinzmetal’s angina, vasospastic angina) refers to the occurrence of anginal episodes at rest, especially at night, accompanied by transitory ST segment elevation (or, at times, ST depression) on an ECG. It is due to severe spasm of a coronary artery, causing ischemia of the heart wall, and is often accompanied by major ventricular arrhythmias, such as ventricular tachycardia (rapid heart beat).
- Silent ischemia. Myocardial ischemia, and even myocardial infarction, can occur without pain or any other symptoms. Pain sensitivity may be altered by a variety of diseases, most notably diabetes mellitus and other neuropathic disorders. Individuals also vary in their threshold for pain.
See Angina Pectoris and Ischemic Heart Disease.
Although the whole listing has a basic requirement for angina, a finding that your impairment equals the listing might be appropriate, if the other combined symptoms are just as limiting in the absence of any angina.
Meeting Social Security Administration Listing 4.04A for Ischemic Heart Disease
You will meet Part A of Listing 4.04A if you have ischemic heart disease, with symptoms due to myocardial ischemia, while on a regimen of prescribed treatment, with:
A. Sign-or-symptom limited exercise test demonstrating at least one of the following manifestations at a workload equivalent to 5 METs or less:
1. Horizontal or down-sloping depression, in the absence of digitalis glycoside treatment or hypokalemia, of the ST segment of at least -0.10 millivolts (-1.0 mm) in at least 3 consecutive complexes that are on a level baseline in any lead other than aVR, and depression of at least -0.10 millivolts lasting for at least 1 minute of recovery; or
2. At least 0.1 millivolt (1 mm) ST elevation above resting baseline in non-infarct leads during both exercise and 1 or more minutes of recovery; or
3. Decrease of 10 mm Hg or more in systolic pressure below the baseline blood pressure or the preceding systolic pressure measured during exercise (see §4.00E9e) due to left ventricular dysfunction, despite an increase in workload; or
4. Documented ischemia at an exercise level equivalent to 5 METs or less on appropriate medically acceptable imaging, such as radionuclide perfusion scans or stress echocardiography.
Part A concerns abnormalities appearing during exercise stress testing. Exercise testing is important in disability determination, because exercise can unmask cardiac ischemia that is not present at rest.
METS
The abnormalities listed in Part A must appear at a level of exercise (workload) that is equivalent to an estimated 5 METs (metabolic equivalents ) or less. Metabolic equivalents are a measure of oxygen use per unit body weight per minute. One MET is the body’s use of 3.5 milliliters of oxygen for each kilogram4of body weight per minute. METs are the standard for expressing how much exertion a person is capable of performing. The higher the physical workload, the higher the MET level required, because more oxygen must used. Activities requiring approximately 5 METs include brisk walking, raking leaves, and light carpentry.
Exercise Test Results
These test results could be obtained from your medical records or through a consultative examination that the Social Security Administration arranges for you. The Social Security Administration should send you for stress testing only when necessary to determine disability. Non-medical doctors, such as disability examiners, claim managers, or disability hearing officers, are unqualified to determine when stress testing is indicated or to evaluate the results.
The Social Security Administration will not use interpretations of resting or exercise ECGs without the actual tracings, or legible copies, for review. Furthermore, the complete report of the test should be available, including the protocol used (time per stage, as well as speed and tilt of a treadmill, for example), blood pressure measurements during testing, and description of any symptoms or physical abnormalities noted during testing. Unfortunately, many cardiac exercise tests are performed in hospitals and hospitals tend to throw away the tracings, only keeping the written narrative of the test results. If so, it is impossible for the Social Security Administration to validate the ECG findings.
Angina
Although angina is a general requirement of the listing, angina does not have to be induced during exercise testing for part A to be satisfied. However, angina may occur during testing and be relieved promptly by cessation of exercise and administration of sublingual nitroglycerin under the observation of a physician. This event would further strengthen the diagnosis of very limiting ischemic heart disease.
Parts A.1 and A.2 Technical Electrical Abnormalities
Parts A.1 and A.2 specify the technical electrical abnormalities that must be present on your ECG at 5 METs or less to meet the listing. The hallmark of ischemia on ECG is what is called ST segment depression, a phrase that is frequently seen in the medical records of individuals with ischemic heart disease. Ischemia can also be demonstrated by an elevation of the ST segment (part A.2), although this is less common.
An ECG is a line that changes in accordance with one cycle of the heart’s electrical activation and recovery, i.e., one heart beat. An actual ECG plots a line of these cycles, one after the other. The standard ECG has 12 leads, which means that 12 different electrodes are placed over different parts of the central and left chest and each records a slightly different view of the heart’s electrical activity.
A resting ECG is the least sensitive method of detecting cardiac ischemia. An ECG done during exercise is much more likely to provoke ischemia, but is still much less effective than testing done with both ECGs and some type of imaging study of the heart during exercise, like an exercise radionuclide study (e.g., thallium treadmill stress test) or exercise echocardiogram (part A.4).
Part A.3 Inability to Increase Systolic Blood Pressure
Part A.3 recognizes that an inability to adequately increase systolic blood pressure (SBP) with exercise even at a low 5 MET level implies severe heart disease, because the heart cannot pump well enough to maintain blood pressure.
This is the same finding required by listing 4.02B3c.
Part A.4 Radionuclide Exercise Testing
Thallium-201 is an example of a radioactive isotope that can be used with exercise testing; technetium is another frequently used radionuclide. Thallium emits x-rays and is not taken up as well by heart tissue that has a poor blood flow (perfusion defect), relative to normal parts of the heart. When the chest is scanned, an image can be constructed from the x-rays. Ischemic perfusion defects are reversible—they appear with exertion and disappear at rest. Fixed defects may indicate scar tissue form a prior heart attack, but can also be “stunned” muscle that is not actually irreversibly dead.
Combining thallium with exercise ECGs—whether a treadmill or bicycle ergometer—greatly increases accuracy in detecting ischemia. The Social Security Administration does not require the actual test films showing a perfusion; the full report and medical interpretation are sufficient. The Social Security Administration refers to “documented” thallium abnormalities, and means an expert interpretation by a cardiologist or radiologist. Second-hand reports of test results written in treating source medical records are not reliable. If judged necessary for accurate evaluation, Social Security Administration medical consultants can request that you undergo exercise testing with radionuclides such as thallium.
If a stress radionuclide study is done, there will always be accompanying ECGs. This situation leaves several possibilities:
1. Both the radionuclide perfusion study and the ECGs are negative for ischemia.
2. Both the perfusion study and the ECGs are positive for ischemia.
3. The perfusion study is positive for ischemia, but the ECGs are negative for ischemia.
4. The perfusion study is negative for ischemia, but the ECGs are positive for ischemia.
5. The perfusion study and/or ECGs are equivocal for ischemia.
Possibilities 1 and 2 could reliably be interpreted as normal and abnormal studies, respectively. Possibility 3 should be interpreted as an abnormal study, because one of the reasons a perfusion study is done along with ECG tracings is that an ECG alone may not be sensitive enough to detect significant ischemia.
Possibility 4 is a little more problematic. Although it is possible to have false negative perfusion results in rare instances, it is much more likely that the ECG tracings are false positive. This is particularly true in electrolyte imbalances, presence of drugs such as digitalis, or women (natural or supplemental estrogens can cause false positive ECG changes).
Possibility 5 requires the most medical judgment; other evidence of heart disease should have considerable weight in these instances. The ability to make judgments regarding test validity is implicit in disability adjudication. Obviously, this judgment should be done only by individuals with professional medical training.
Resting ECG Abnormalities
Part A does not mention the possibility of an abnormal resting ECG showing cardiac ischemia. A resting ECG performed while a person has angina will show myocardial ischemia about half the time.
If you have chest pain compatible with angina and resting ECG changes that are compatible with ischemia, the Social Security Administration should give serious consideration to a finding of equivalent severity to part A without requiring exercise testing. A concurrent exercise test already in the medical evidence that shows no ischemia would take priority over resting changes, because true ischemia on a resting ECG would worsen with exertion.
Medical judgment must be applied on a case by case basis in regard to how resting ECG abnormalities are adjudicated.
Meeting Social Security Administration Listing 4.04B for Ischemic Heart Disease
You will meet Part B of Listing 4.04 if you have ischemic heart disease, with symptoms due to myocardial ischemia, while on a regimen of prescribed treatment, with three separate ischemic episodes, each requiring revascularization or not amenable to revascularization, within a consecutive 12-month period.
Part B recognizes that repeated episodes of clinical deterioration as a result of ischemic heart disease can be disabling.
To count as an episode you must have had revascularization either by angioplasty (with or without stenting) or bypass surgery. If surgery is not done, the ischemic episode can still qualify if not amenable to surgery. “Not amenable” means that the revascularization procedure could not be done because of another medical impairment or because the vessel was not suitable for revascularization. Re-occlusion of a vessel during the same hospitalization does not count for listing purposes.
If you satisfy this part of the listing, you could be found to have had significant medical improvement and no longer be disabled at a future continuing disability review once your condition has stabilized, if you don’t meet any other part of this listing or another listing.
Meeting Social Security Administration Listing 4.04C for Ischemic Heart Disease
You will meet Part C of Listing 4.04 if you have ischemic heart disease, withsymptoms due to myocardial ischemia, while on a regimen of prescribed treatment, with:
- Coronary artery disease,
- Demonstrated by angiography (obtained independent of Social Security disability evaluation) or other appropriate medically acceptable imaging, and
- In the absence of a timely exercise tolerance test or a timely normal drug-induced stress test,
- An MC, preferably one experienced in the care of patients with cardiovascular disease, has concluded that performance of exercise tolerance testing would present a significant risk,
- With both 1 and 2:
1. Angiographic evidence revealing:
a. 50 percent or more narrowing of a non-bypassed left main coronary artery; or
b. 70 percent or more narrowing of another non-bypassed coronary artery; or
c. 50 percent or more narrowing involving a long (greater than 1 cm) segment of a non-bypassed coronary artery; or
d. 50 percent or more narrowing of at least 2 non-bypassed coronary arteries; or
e. 70 percent or more narrowing of a bypass graft vessel; and
2. Resulting in very serious limitations in the ability to independently initiate, sustain, or complete activities of daily living.
Coronary artery disease (CAD) is by far the most common cause of ischemic heart disease (see Figure 6 below). The term is understood to refer to obstructive lesions in the largest coronary arteries, known as the epicardial arteries because they lie near the surface of the heart. These arteries arise from the aorta just as blood is ejected from the left ventricle through the aortic valve into the systemic circulation, so that the heart itself is the first organ to receive oxygenated blood.
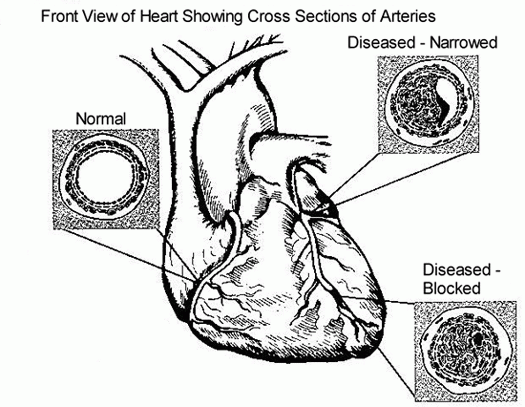
Figure 6: Detail of arteries in a normal heart and in a heart with coronary artery disease.
Part C applies only when no timely exercise tolerance test (ETT) or other cardiac stress test is available and when a Social Security medical consultant concludes that stress testing would present a significant risk to the claimant. If these conditions are fulfilled, then Part C has both angiographic criteria (C.1a-e) and functional loss criteria (C.2). Both must be satisfied.
Part C.1 Angiographic Criteria
A re-obstructed artery following prior angioplasty or bypassing is non-bypassed for purposes of the listing.
In prior listings, the Social Security Administration would have required cardiac catheterization done independently of the Social Security Administration to demonstrate the severity of coronary artery lesions. Currently, less invasive procedures are fully satisfactory imaging modalities, including electron beam computed tomography, high-resolution CT scanning, and magnetic resonance imaging. In some instances, echocardiography can be used to image parts of larger coronary arteries. Of course, the Social Security Administration does not have to accept inappropriate imaging that does not reveal the nature, location, and severity of the lesions sufficiently to allow reasonable application of the listing.
The new high-resolution 64-slice CT scanners are capable of providing excellent imaging of coronary arteries and are increasingly being used to screen patients who have chest pain for coronary artery disease. Although some radiation is delivered to the patient, such CT angiography can provide a faster and more cost-effective way for diagnosing coronary disease as the probable cause of chest pain, compared to stress testing with radionuclides or conventional angiography by cardiac catheterization. As the resolution of cardiac MRI scanners improves, it is likely that the future will permit imaging of the heart without any X-rays. Conventional angiography exposes the patient to X-rays, as well as being invasive and more risky and expensive. However, if intervention is eventually needed (such as stenting a coronary artery), then cardiac catheterization is unavoidable.
Part C.2 Functional Loss Criteria
Part C.2 provides guidance on functional loss as a result of limitations caused by ischemic heart disease. At this level of severity, a claimant would normally have significant amounts of medical records, including hospitalization records to support the credibility of markedly limiting symptoms: fatigue, palpitation, dyspnea (shortness of breath), or angina. Angina alone is a sufficient symptom for allowance under part C.2, if severe enough. If not, additional symptoms of fatigue, palpitations, or dyspnea combined with angina, are sufficient for allowance under part C.2.
It cannot be over-emphasized that specific examples of limitations in activities of daily living are much more helpful to the Social Security Administration than generalizations.
Residual Functional Capacity Assessment for Ischemic Heart Disease
What Is RFC?
If your ischemic heart disease is not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary work in spite of your impairments. The lower your RFC, the less the Social Security Administration believes you can do.
Adult ischemic heart disease that is significant but does not meet or equal the listing will require some type of residual functional capacity.
RFC Guidelines Regarding Exercise Test Performance
The Social Security Administration generally applies the following RFCs regarding exercise test performance:
- An abnormal test workload equivalent to an estimated 5 METs or less – Meets listing 4.04 part A if other criteria are satisfied. See Meeting Social Security Administration Listing 4.04A for Ischemic Heart Disease.
- A normal test workload equivalent exceeding 5 METs, but test positive at 6 METs or claimant unable to complete duration of 6 MET stage – sedentary work RFC.
- A normal test workload equivalent of 6 METs or more, but test positive at 7 METs or claimant unable to complete duration of 7 MET stage – light work RFC.
- A normal test workload equivalent of 7 METs or more, but test positive at 8 METs or claimant unable to complete duration of 8 MET stage – medium work RFC.
- A normal test workload equivalent of 8 METs or more, negative test for completing full 8 MET stage or more – heavy work or “not severe.”
Environmental Restrictions
Once the general RFC is determined, further downward modification of the RFC may be indicated on the basis of environmental restrictions.
Factors that increase the heart’s work can cause the onset of ischemia and symptoms like angina, shortness of breath (SOB) and fatigue to occur at earlier levels of exertion than would otherwise be the case. An increase in blood pressure will have that effect. Environmental extremes like very hot or cold environments will increase physiological stress that does not occur from exercise testing in a nice, cool hospital or doctor’s office. For instance, heat or cold alone will drive up heart rate and leave less cardiac reserve for exertion.
An individual who can do medium work at a comfortable room temperature could reasonably be expected to be capable of no more than light work in hot or cold environments. Even healthy people are compromised in their exertional capacity in hot or cold environments, and individuals with heart disease are even more fragile in this regard.
Psychological stress can have the same effect, because it also increases the heart rate even before exertion begins. While it is obvious that certain occupations, such as being a police officer, are generally associated with high psychological stress, this is a rather murky area because such stress depends not only on the environment but the individual’s reaction to that environment. For example, some attorneys find litigation in a courtroom extremely stressful while others feel hardly a twinge of anxiety or even feel exhilarated by the experience.
Environmental limitations are sometimes overlooked by adjudicators. For example, if avoidance of temperature extremes is not mentioned on the RFC form, then the disability examiner or vocational analyst citing jobs you can still do will not apply that limitation. The consequences are that you may be cited a job that you cannot perform. If you are cited a job in which environmental extremes are involved, the RFC should be lowered one level from what it would otherwise be based on stress test results.
Environmental limitations that result in the elimination of your ability to return to prior work, restriction of applicable other work, lowering of RFC, and elimination of the “Grid” all present the opportunity for allowance of claims that would otherwise be erroneously denied.
Medications
Environmental work capacity is not just influenced by physiological stress, but also by medications. For example, consider a claimant with ischemic heart disease who has had heart failure. He takes a number of medications, including diuretics, that are carefully adjusted. The diuretics accelerate urinary fluid loss. If this person is exposed to extreme heat causing a lot of sweating, he may go into fluid imbalance and end up in the hospital. It is not reasonable to think that he can reliably adjust his water intake under changing conditions, although this can be accomplished to some degree. And it’s not just water that has to be replaced. Electrolytes (sodium, potassium) are likely to be moved out of normal range with possible serious consequences such as cardiac arrhythmias, increased weakness, and impairment in thinking.
Drugs known as beta-blockers, frequently used to treat hypertension and ischemic heart disease, suppress the ability to increase heart rate. This drug effect can affect the body’s ability to respond to the increased stress of temperature extremes.
Silent Cardiac Ischemia
It is possible to have very severe cardiac ischemia caused by marked coronary obstructive lesions and yet have no chest pain, weakness, or any other symptoms, i.e., “silent ischemia.” The Social Security Administration recognizes that silent ischemia must be considered in disability determination.
Severe silent ischemia appearing in the early stages of an exercise test is ominous. Even if a claimant has no history of symptoms such as angina that would qualify under the listing, an RFC limitation would be appropriate.
Other claimants may have abnormal ischemic resting ECGs that appear during routine monitoring of the heart for other purposes—such as 24-hour monitoring for an arrhythmia with a Holter monitor. Or they may simply have an abnormal resting ECG for the presence of ischemic heart disease even though they have no angina or other cardiac symptoms. In these instances also, some degree of RFC limitation in proportion to the severity of the abnormality should be given even if there are no symptoms.
Environmental stressors, especially extreme heat or cold, can make silent ischemia worse and perhaps even provoke symptoms such as angina or life-threatening arrhythmias that otherwise might be absent.
Cardiac Arrhythmias
Arrhythmias are most often related to the presence of ischemic heart disease in the adult claimant population. If a life-threatening arrhythmia appears at a particular stage of exertion on a cardiac stress test, that test should be considered positive and a factor in limiting RFC to a level of exertion at which the threat does not appear. As in other manifestations of ischemic heart disease, adverse environmental conditions such as heart or cold can produce further limitations.
Cognitive Losses After Coronary Artery Bypass Grafting
Problem of Cognitive Decline After Surgery
A great danger of coronary artery bypass grafting (CABG) (see Figure 7 below) is brain damage resulting in stroke (cerebrovascular accident, CVA). Some of these strokes result from surgical cross-clamping of the arch of the aorta during the operation when small pieces of atherosclerotic fatty matter can come loose and be pumped to the brain, where it lodges in an artery and blocks blood flow to some part of the brain.
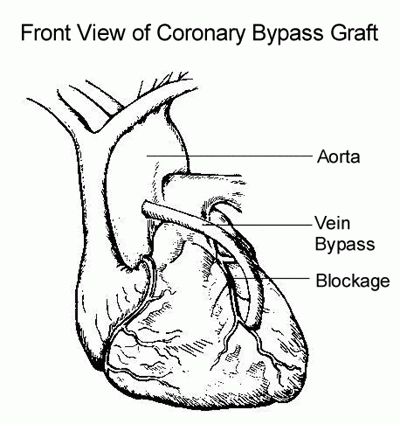
Figure 7: Revascularization via coronary artery bypass graft using a vein.
Even when no obvious stroke occurs, a person may have decreased reasoning ability (cognitive dysfunction) after CABG. While large strokes are likely to be obvious and included in the disability determination, significant cognitive dysfunction resulting from lesser degrees of brain damage, or brain damage to areas not involved in movement, can be missed.
Cognitive decline after CABG affects 16-42% of patients. The possibility of brain damage is not emphasized to patients by cardiologists and cardiac surgeons, because they do not want patients to be afraid of having needed surgery.
Causes of Post-CABG Cognitive Dysfunction
Most people having CABG will have at least microscopic particles of clotted blood (microthrombi) pumped into the cerebral circulation. In addition to fatty material dislodged from arterial walls and particles of clotted blood, microemboli often contain toxic material associated with surgical equipment. For example, a high prevalence of aluminum (Al) and silicon (Si) in microemboli enter the cerebral circulation, undoubtedly from surgical equipment or instrumentation. The elements Al and Si are both very toxic to the brain and anatomical damage to cerebral arteries may also be present post-surgically.
Cognitive dysfunction after CABG is likely to have multiple contributing causes, including some nonspecific effect of surgery, anesthesia, and decreased perfusion of the brain with blood (cerebral hypoperfusion), in addition to the microemboli already discussed.
Not all research agrees on the issue of whether long-term cognitive decline is actually associated with CABG. It may be that any effects associated with the surgery itself are reversible. Some research suggests that long-term cognitive decline has nothing to do with CABG, but is related to underlying or progressive disorders present in the patient such as cerebrovascular disease, prior strokes, diabetes, or hypertension.
Why Cognitive Dysfunction May Be Overlooked
MRI scans have demonstrated areas of brain damage post-CABG even in the absence of neurological abnormalities. Yet MRIs are not a standard part of post-operative evaluation.
Unless the claimant makes a specific allegation of cognitive problems, the Social Security Administration is likely to not even consider the possibility of cognitive dysfunction. However, the lack of an allegation by a claimant should not sufficient basis for disregarding the possibility of cognitive dysfunction; one cannot reasonably expect a person with impaired judgment to have an optimal ability to act in his or her own interest. The claimant’s spouse is most likely to notice personality changes and decline in thinking ability after CABG.
The Social Security Administration adjudicator should generally not rely on the cardiac surgeon’s notes to determine that the claimant has no post-operative cognitive dysfunction. Surgeons are mostly interested in surgical results involving the heart and do not perform neuropsychological tests that would be required to detect less than marked cognitive abnormalities.
After any cardiac or vascular procedure, a claimant’s representative should always consider the possibility of cognitive dysfunction. If the claimant appears normal mentally, the medical records negative, and the claimant and spouse feel there is no problem then further pursuit of this possibility probably will not be productive. However, significant numbers of cognitive dysfunction cases probably slip through the disability determination process as adjudicators concentrate only on the physical impairment.
Evaluation of Cognitive Dysfunction for Disability Purposes
Cognitive dysfunction would primarily be evaluated under the criteria for organic mental disorders, listing 12.02. Other, pre-existing mental disorders, such as personality disorders (listing 12.08) may be worsened.
Any neuropsychological testing should be done at least 3 months post-CABG, to allow clearing of any shorter term cognitive deficits.
Getting Your Doctor’s Medical Opinion About What You Can Still Do
Your Doctor’s Medical Opinion Can Help You Qualify for Social Security Disability Benefits
The Social Security Administration’s job is to determine if you are disabled, a legal conclusion based on your age, education and work experience and medical evidence. Your doctor’s role is to provide the Social Security Administration with information concerning the degree of your medical impairment. Your doctor’s description of your capacity for work is called a medical source statement and the Social Security Administration’s conclusion about your work capacity is called a residual functional capacity assessment. Residual functional capacity is what you can still do despite your limitations. The Social Security Administration asks that medical source statements include a statement about what you can still do despite your impairments.
The Social Security Administration must consider your treating doctor’s opinion and, under appropriate circumstances, give it controlling weight.
The Social Security Administration evaluates the weight to be given your doctor’s opinion by considering:
- The nature and extent of the treatment relationship between you and your doctor.
- How well your doctor knows you.
- The number of times your doctor has seen you.
- Whether your doctor has obtained a detailed picture over time of your impairment.
- Your doctor’s specialization.
- The kinds and extent of examinations and testing performed by or ordered by your doctor.
- The quality of your doctor’s explanation of your impairment.
- The degree to which your doctor’s opinion is supported by relevant evidence, particularly medically acceptable clinical and laboratory diagnostic techniques.
- How consistent your doctor’s opinion is with other evidence.
When to Ask Your Doctor for an Opinion
If your application for Social Security disability benefits has been denied and you have appealed, you should get a medical source statement (your doctor’s opinion about what you can still do) from your doctor to use as evidence at the hearing.
When is the best time to request an opinion from your doctor? Many disability attorneys wait until they have reviewed the file and the hearing is scheduled before requesting an opinion from the treating doctor. This has two advantages.
- First, by waiting until your attorney has fully reviewed the file, he or she will be able to refine the theory of why you cannot work and will be better able to seek support for this theory from the treating doctor.
- Second, the report will be fresh at the time of the hearing.
But this approach also has some disadvantages.
- When there is a long time between the time your attorney first sees you and the time of the hearing, a lot of things can happen. You can improve and go back to work. Your lawyer can still seek evidence that you were disabled for a certain length of time. But then your lawyer will be asking the doctor to describe your ability to work at some time in the past, something that not all doctors are good at.
- You might change doctors, or worse yet, stop seeing doctors altogether because your medical insurance has run out. When your attorney writes to a doctor who has not seen you recently, your attorney runs the risk that the doctor will be reluctant to complete the form. Doctors seem much more willing to provide opinions about current patients than about patients whom they have not seen for a long time.
Here is an alternative. Suggest that your attorney request your doctor to complete a medical opinion form on the day you retain your attorney. This will provide a snapshot description of your residual functional capacity (RFC) early in the case. If you improve and return to work, the description of your RFC provides a basis for showing that you were disabled for a specific period. If you change doctors, your attorney can get an opinion from the new doctor, too. If you stop seeing doctors, at least your attorney has one treating doctor opinion and can present your testimony at the hearing to establish that you have not improved.
If you continue seeing the doctor but it has been a long time since the doctor’s opinion was obtained, just before the hearing your attorney can send the doctor a copy of the form completed earlier, along with a blank form and a cover letter asking the doctor to complete a new form if your condition has changed significantly. If not, your attorney can ask the doctor to send a one-line letter that says there have been no significant changes since the date the earlier form was completed.
There are times, though, that your attorney needs to consider not requesting a report early in the case.
- First, depending on the impairment, if you have not been disabled for twelve months, it is usually better that your attorney wait until the twelve-month duration requirement is met.
- Second, if you just began seeing a new doctor, it is usually best to wait until the doctor is more familiar with your condition before requesting an opinion.
- Third, if there are competing diagnoses or other diagnostic uncertainties, it is usually best that your attorney wait until the medical issues are resolved before requesting an opinion.
- Fourth, a really difficult judgment is involved if your medical history has many ups and downs, e.g., several acute phases, perhaps including hospitalizations, followed by significant improvement. Your attorney needs to request an opinion at a time when the treating doctor will have the best longitudinal perspective on your impairment.
Medical Opinion Forms
Medical opinion forms can be great time savers for both your attorney and your doctor, but they must be used with care. Forms may not be appropriate at all in complex cases; and they need to be supplemented in many cases so that all issues are addressed. The best forms are clear and complete but not too long.

