How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Chronic Liver Disease?
If you have any type of chronic liver disease, including chronic viral hepatitis, Social Security disability benefits may be available. To determine whether you are disabled by your chronic liver disease, the Social Security Administration first considers whether your liver disease is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Liver Disease by Meeting a Listing. If you meet or equal a listing because of chronic liver disease, you are considered disabled. If your liver disease is not severe enough to equal or meet a listing, the Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your liver disease), to determine whether you qualify for benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Liver Disease.
About Chronic Liver Disease and Disability
What Is Chronic Liver Disease?
Chronic liver disease is characterized by liver cell necrosis (death), inflammation, or scarring (fibrosis or cirrhosis) due to any cause that persists for more than 6 months.
Examples of Chronic Liver Disease
Examples of chronic liver disease include, but are not limited to:
- Chronic hepatitis;
- Alcoholic liver disease;
- Non-alcoholic steatohepatitis (NASH);
- Primary biliary cirrhosis (PBC);
- Primary sclerosing cholangitis (PSC);
- Autoimmune hepatitis;
- Hemochromatosis (liver damage from iron overload, resulting from a defect in the body’s ability to metabolize iron properly);
- Drug-induced liver disease;
- Wilson’s disease (a rare genetic disease caused by a defect in the body’s ability to metabolize copper); and
- Serum alpha-1 antitrypsin deficiency.
There are many other possible causes of liver disease, such as metabolic disorders (e.g., cystic fibrosis, porphyria, glycogen storage disease), vascular diseases (e.g., polymyalgia rheumatica, polyarteritis nodosa), parasitic infections (particularly roundworms, tapeworms, and flatworms), bacterial and fungal infections, toxins and drugs, and autoimmune hepatitis.
Some cases of liver failure are caused by an unknown agent.
Signs and Symptoms of Chronic Liver Disease
Signs of chronic liver disease may include:
- Jaundice (yellowing of the skin),
- Enlargement of the liver and spleen,
- Ascites (fluid in the abdomen),
- Peripheral edema (swelling of extremities), and
- Altered mental status.
Symptoms may include:
- Pruritis (itching),
- Fatigue,
- Nausea,
- Loss of appetite, or
- Sleep disturbances.
Symptoms of chronic liver disease may have a poor correlation with the severity of liver disease and functional ability.
Laboratory Findings Associated With Liver Disease
With liver disease, blood tests may show increased liver enzymes, increased serum total bilirubin, increased ammonia levels, decreased serum albumin, and abnormal coagulation studies, such as increased International Normalized Ratio (INR) or decreased platelet counts.
Abnormally low serum albumin or elevated INR levels indicate loss of liver function, with increased likelihood of cirrhosis and associated complications. However, other abnormal lab tests, such as liver enzymes, serum total bilirubin, or ammonia levels, may have a poor correlation with the severity of liver disease and functional ability.
A liver biopsy may demonstrate the degree of liver cell necrosis, inflammation, fibrosis, and cirrhosis. If you have had a liver biopsy, the Social Security Administration will make every reasonable effort to obtain the results; however, it will not pay for you to have one.
Imaging studies (CAT scan, ultrasound, MRI) may show the size and consistency (fatty liver, scarring) of the liver and document ascites (fluid in the abdomen).
Chronic Viral Hepatitis Infections
Hepatitis means inflammation of the liver. If lasting more than about 6 months, it may be termed chronic. Prolonged hepatitis can lead to cirrhosis.
Although there are several different types of viral hepatitis infections, chronic viral hepatitis infections are commonly caused by hepatitis C virus (HCV), and to a lesser extent, hepatitis B virus (HBV). Usually, these are slowly progressive disorders that persist over many years during which the symptoms and signs are typically nonspecific, intermittent, and mild (for example, fatigue, difficulty with concentration, or right upper quadrant pain).
The spectrum of these chronic viral hepatitis infections ranges widely. Some patients may have no symptoms; others may have only mild to moderate symptoms. Some may develop cirrhosis, end stage liver disease with the need for liver transplantation, or liver cancer.
Chronic Hepatitis B (HBV) Infection
Chronic HBV infection is diagnosed by the detection of hepatitis B surface antigen (HBsAg) in the blood for at least 6 months. The goal of treatment is to suppress HBV replication and thereby prevent progression to cirrhosis and end stage liver disease. Treatment usually includes a combination of interferon injections and oral antiviral agents.
The hepatitis B virus is a highly infectious organism. Worldwide, there are hundreds of millions of carriers. Millions of individuals die yearly from hepatitis B viral infections. HBV may induce a form of liver cancer known as hepatocellular carcinoma that kills many hundreds of thousands of people worldwide every year.
In the U.S., probably less than 1% of the population are carriers. This is much lower than in some other parts of the world where the majority of individuals have been infected. High-risk groups for infection are male homosexuals, IV drug users, and individuals working in healthcare who are exposed to blood or blood products.
There is about a 10% chance of infection of a person who suffers an accidental stick with a needle contaminated with the blood of a HBV carrier. Donated blood is routinely screened for hepatitis B to prevent transmission by transfusion, but this doesn’t protect health workers exposed to blood in the course of a patient’s care. In addition to blood, a carrier has virus in semen, saliva, vaginal secretions, sweat, tears, urine, and breast milk.
If swallowed, the virus is destroyed by pancreatic enzymes in the digestive tract which probably explains why oral transmission is rare and transmission in food has not been documented. In the rare cases of oral transmission, infection probably occurred because of breaks in the oral mucosa or gingiva that allowed the virus to directly enter the bloodstream.
Transmission of the virus from blood or other bodily fluids through small cuts or abrasions in the skin or mucous membranes of which a person is unaware may explain why as many as 50% of infected individuals have no history of high-risk exposure. As many as 80% to 90% of infected individuals are unaware they are carriers.
Maximum symptoms occur at about 3 to 5 months after initial infection and correspond to the greatest liver inflammation as reflected by a peak in transaminase liver enzymes. Once infected, some individuals may die within a matter of weeks from severe and aggressive hepatitis and liver failure, but this outcome involves less than 1% of cases. Most patients (90% to 95%) will have a full recovery, and 5% to 10% will become chronic carriers of the virus.
Carriers with no symptoms who also have normal levels of transaminase enzymes have a good prognosis, because they have no continuing hepatitis. Those who have abnormal transaminases indicative of continuing hepatitis have a poorer prognosis even if they have no symptoms. Such carriers are more likely to develop chronic persistent hepatitis (CPH), chronic active hepatitis (CAH), and hepatocellular carcinoma.
Chronic Hepatitis C (HCV) Infection
Chronic HCV infection is diagnosed by the detection of hepatitis C viral RNA in the blood for at least 6 months. Hepatitis C can be transmitted in blood and can cause both acute and chronic liver inflammation, as well as cirrhosis of the liver. Along with alcohol abuse, hepatitis C is the most common cause of cirrhosis. At least 4 million people in the U.S. are infected, and many are unaware that they are infectious. Risk of infection is increased by sexual intercourse with infected individuals and by intravenous drug use. About half of infected individuals progress to chronic active hepatitis (CAH) and have an associated increased risk of liver cancer.
Treatment usually includes a combination of interferon injections and oral ribavirin. Whether a therapeutic response has occurred is usually assessed after 12 weeks of treatment by checking the HCV viral load. A substantial reduction in HCV viral load (also known as early viral response, or EVR) predicts a sustained viral response with completion of treatment. Combined therapy is commonly discontinued after 12 weeks when there is no early viral response, since in that circumstance there is little chance of obtaining a sustained viral response (SVR). Otherwise, treatment is usually continued for a total of 48 weeks.
Combined interferon and ribavirin treatment may have significant adverse effects that may require dosing reduction, planned interruption of treatment, or discontinuation of treatment. Adverse effects may include: anemia (ribavirin-induced hemolysis), neutropenia (low neutrophil [type of white blood cell] count), thrombocytopenia (low platelet count), fever, cough, fatigue, myalgia (muscle pain), arthralgia (joint pain), nausea, loss of appetite, pruritis (itching), and insomnia. Behavioral side effects may also occur. Influenza-like symptoms are generally worse in the first 4 to 6 hours after each interferon injection and during the first weeks of treatment. Adverse effects generally end within a few days after treatment is discontinued.
Chronic Active Hepatitis
Chronic active (aggressive) hepatitis (CAH) is a very serious disorder whose specific cause is unknown, but may involve some abnormal immune response by the liver to a particular agent. If the CAH is related to intake of a drug, it may rapidly improve with withdrawal of that drug. However, cases associated with viral infections have a much poorer prognosis. Overall, CAH has a high mortality despite treatment, and sometimes can be associated with problems in organ systems other than the liver. These include arthralgia (joint pains), anemia, fibrosis of the lungs, intestinal inflammation, and kidney disease.
Cirrhosis
The most frequent kind seen by the Social Security Administration is cirrhosis of the liver caused by the abuse of alcohol. The term cirrhosis refers to present or past evidence of hepatic (liver) cell necrosis (death), fibrosis (replacement of normal cells with fibrous tissue), and areas of regenerating nodules of liver tissue attempting to recover from previous damage.
Tissue for microscopic evaluation must be removed from the liver (biopsy), which is the only way a certain diagnosis of cirrhosis can be made. The Social Security Administration does not purchase liver biopsies on claimants. When they are done by a treating source, they are usually percutaneous—a needle is inserted into the liver through the skin between the right lower ribs under local anesthesia and can be done at the bedside.
The liver makes and secretes bile into the bile ducts, and these ducts in turn carry bile to the gallbladder for storage, and also to the small intestine (see Figure 1 below). Bile assists in the absorption of fats from the intestine. Biliary cirrhosis results when normal bile flow is interrupted and the liver cells are exposed to it. Primary biliary cirrhosis is usually found in older females and involves obstruction to bile flow in the small biliary ducts inside the liver itself. Secondary biliary cirrhosis involves obstruction of the larger ducts outside the liver (extrahepatic ducts) with a consequent back-pressure of bile into the liver. Gallstones may produce an obstruction, or stricture related to previous surgery, or rarely an obstructing cancer.
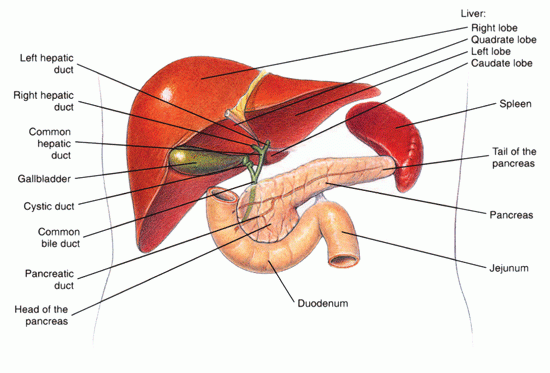
Figure 1: The liver, pancreas, and duodenum.
Toxins as a Cause of Hepatitis
Many toxic substances can cause hepatitis, the most prominent of which is excessive alcohol intake. People vary greatly in the efficiency with which their liver can metabolize alcohol, and there is no way to predict individual capacity in this regard. By far, alcoholic hepatitis is the most frequent form of hepatitis and is usually acutely superimposed upon a more chronic underlying cirrhosis. As a patient is detoxified in a treatment facility, the alcoholic hepatitis improves with progression of residual chronic cirrhosis. Some cases of acute alcoholic hepatitis are fatal and cirrhosis eventually results in the death in many others.
Acute Hepatitis
Alcoholics, in particular those who have been binge drinking, can have an episode of acute alcoholic hepatitis superimposed on an underlying chronic liver disease. When hospitalized where alcohol is unavailable and treated, the acute hepatitis can improve. In these claims, the Social Security Administration can be expected to hold the claim for a few months to determine what degree of improvement will occur with treatment of the acute episode.
Claimants with acute viral hepatitis will be treated similarly, because most will improve over the short term.
Winning Social Security Disability Benefits for Liver Disease by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your liver disease is severe enough to meet or equal the chronic liver disease listing. The Social Security Administration has developed rules called Listing of Impairments for most common impairments. The listing for a particular impairment describes a degree of severity that Social Security Administration presumes would prevent a person from performing substantial work. If your liver disease is severe enough to meet or equal the listing, you will be considered disabled.
The listing for chronic liver disease is 5.05. It has 7 parts, A through G. You will be disabled if you satisfy any part. Regardless of cause, you must establish that you have chronic liver disease to satisfy any part of the listing. The Social Security Administration defines chronic as persisting more than six months.
There are many types and causes of chronic liver disease. Instead of picking out criteria for a huge number of possible liver disorders, the Social Security Administration has created the listing to cover the fundamental complications that could produce functional limitations or death regardless of specific cause.
Meeting Social Security Administration Listing 5.05A for Liver Disease
You will meet listing 5.05A if you have chronic liver disease with:
- Hemorrhaging from esophageal, gastric, or ectopic varices or from portal hypertensive gastropathy;
- Demonstrated by endoscopy, X-ray, or other appropriate medically acceptable imaging;
- Resulting in hemodynamic instability; and
- Requiring hospitalization for transfusion of at least 2 units of blood.
If you meet this listing, you will be considered under a disability for 1 year following your last documented transfusion. Thereafter, you will be evaluated for residual impairments.
Varices
Varices are dilated areas in blood vessels (areas with enlarged diameters). Sometimes varices rupture and bleed. Part A of the listing recognizes that severe liver disease can cause varices and their potential complication of life-threatening bleeding in the esophagus and stomach (gastric varices). The broad term “ectopic varices” also recognizes other less likely locations such as the gallbladder.
Esophageal Varices
The liver is connected to the portal venous system that receives blood from the intestines. The portal vein provides about 75% of the liver’s blood flow (see Figure 2 below).
The esophageal veins drain into the portal system. Cirrhosis of the liver results in increased pressure inside the portal system, known as portal hypertension. Abnormal pressures are transmitted back to the esophageal veins, which are delicate and close to the inner surface of the esophagus. Dilated areas (esophageal varices) can develop in these veins.
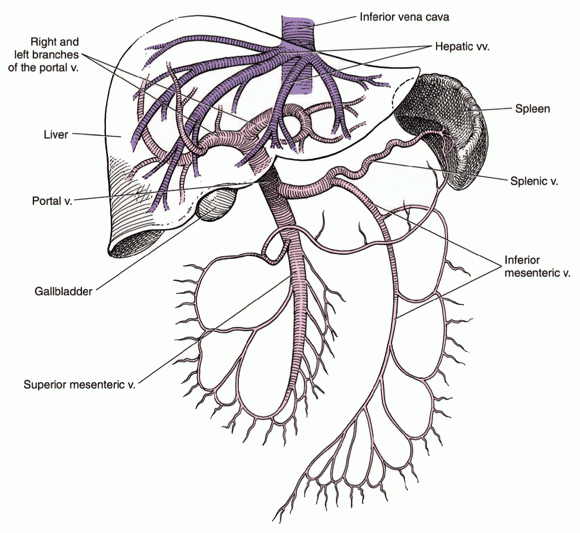
Figure 2: The hepatic portal vein system.
When bleeding does occur, it can be minor, or life-threatening. By far, most of the bleeding esophageal varices seen by the Social Security Administration are in alcoholics. However, since other types of cirrhosis—such as that caused by hepatitis C infection—also can result in varices, bleeding should not result in a presumption of alcoholism.
Fifty to 75% of people who have had bleeding varices will experience re-bleeding within 1 to 2 years of a bleeding episode. Bleeding varices are usually treated with fiberoptic endoscopy. MRIs and CT scans to image varicosed veins in the esophagus and intra-abdominally are also useful tools that may be part of the diagnostic work-up. However, endoscopy is most important for diagnosis of esophageal and gastric varices.
Esophageal varices are frequently treated initially with sclerotherapy, in which a scarring solution is injected into varices as an endoscopic procedure. However, if sclerotherapy does not prevent bleeding, more definitive treatment may be needed, and that is shunt surgery.
Portal Hypertensive Gastropathys
Portal hypertensive gastropathy (PHG) refers to changes in the stomach lining of patients with portal hypertension. The most common cause of PHG is cirrhosis of the liver. In patients with PHG, the the stomach mucosa has a snake skin appearance that is radically different from the mucosa’s usual smooth look. Patients with portal hypertensive gastropathy may experience bleeding from the stomach. When there are red spots throughout the stomach, the term diffuse gastric vascular ectasia is used.
It has been estimated that nearly two-thirds of patients with cirrhosis will eventually develop PHG. This disorder is frequently associated with varices in the esophagus or stomach, but they are not necessary for a diagnosis of PHG. Furthermore, PHG can cause life-threatening bleeding without varices in the esophagus or elsewhere.
PHG is usually diagnosed by endoscopy.
PHG is most often found in the more proximal or upper parts of the stomach closer to the esophagus. It accounts for about 10% of all causes of gastrointestional bleeding and about 25% of cases of bleeding in individuals with portal hypertension.
Beta-blocker drugs have been useful in prevention of chronic blood loss. Iron supplementation is required. A portocaval shunt (requiring surgery) or a transjugular intrahepatic portal-systemic shunt (TIPS) may decrease the risk of bleeding by lowering venous pressures and is used when medications fail. Argon photocoagulation therapy has also been used, and some experiments have been done with carbon dioxide cryotherapy to stop acute bleeding.
Gastric Vascular Antral Ectasia
Gastric vascular antral cctasia (GAVE, GVE) is not mentioned by the listing, but should be considered as of equivalent severity to portal hypertensive gastropathy (PHG). GAVE is associated with bleeding from abnormal vessels in the distal (lower) stomach. It may not have the snakeskin pattern in the mucosa. As with PHG, stabilization of iron stores from blood loss is needed. Estrogen-progesterone combination drug therapy has been of some use when thermoablative argon laser photocoagulation has been ineffective.
Unlike PHG, GAVE may be more related to liver failure than to portal hypertension caused by liver failure, because liver transplantation leads to a cure. If bleeding continues despite thermoablative therapy and hormonal treatment, then surgical resection of the distal stomach (antrum) has been done. Unlike PHG, a shunt (TIPS) is not a treatment for GAVE, because it does not significantly reduce the risk of bleeding and is associated with a much higher risk of hepatic encephalopathy.
Fortunately, GAVE is not as common as PHG.
Bleeding and Transfusion Requirements
GI bleeding can be vomiting blood (hematemesis), tarry stools (melena), or bloody stools (hematochezia). The manner of blood loss is not important. Hospitalization to provide supportive care for life-threatening bleeding must be documented. You must require at least 2 units of blood at least 30 days apart, at least three times in a consecutive 6-month period. You must require hospitalization for each episode.
Signs of Hemodynamic Instability
To further substantiate that blood loss is severe and resulting from bleeding, rather than one of the many causes of anemia, there must be evidence of hemodynamic instability, that is, severe physiological and measurable changes resulting from inadequate perfusion of tissues.
These signs are:
- Pale skin (pallor);
- Profuse perspiration (diaphoresis);
- Rapid pulse (tachycardia);
- Low blood pressure (hypotension);
- Falling blood from the act of standing up from lying down (postural hypotension); and
- Fainting (syncope).
The Social Security Administration should not require all of these signs of hemodynamic instability to be documented, because the reality is that hospital records are not always of the quality they should be. However, in the total context of a patient’s condition, the data should indicate such instability.
Meeting Social Security Administration Listing 5.05B for Liver Disease
You will meet listing 5.05B if you have chronic liver disease with:
- Ascites or hydrothorax not attributable to other causes,
- Despite continuing treatment as prescribed,
- Present on at least two evaluations at least 60 days apart within a consecutive 6-month period.
Each evaluation must be documented by:
1. Paracentesis or thoracentesis; or
2. Appropriate medically acceptable imaging or physical examination and one of the following:
a. Serum albumin of 3.0 g/dL or less; or
b. International Normalized Ratio (INR) of at least 1.5.
Ascites
Ascites means an abnormal accumulation of fluid in the abdomen. If of hepatic origin, ascites is a sign of very serious liver disease. In advanced liver disease, the liver cannot produce a normal amount of albumin, and this can result in a disruption of fluid balance between the body’s internal compartments. If there is enough ascites, a doctor can palpate it in a patient’s abdomen on a physical examination. But this method of detection is not reliable, especially in obese claimants.
In a non-obese person, ascites is often easily demonstrable based on a patient’s history and physical examination when there is severe cirrhosis and the abdomen is large and bulging. It takes about 1.5 liters (1500 ml) of ascitic fluid to be detected on physical examination.
Paracentesis is a procedure by which a physician inserts a needle into the abdomen to remove some of the ascitic fluid. The Social Security Administration never orders this test because of its invasive nature. The clinical basis for paracentesis is to discover the cause of ascites, not prove its presence. If available, however, abdominal fluid obtained by paracentesis is irrefutable proof of ascites and its chemical content may establish that liver disease is the cause of ascites.
Ascites can be caused by cirrhotic liver disease, a condition that in the U.S. most often results from alcohol abuse and hepatitis C infection.
In addition to liver disease, ascites can also be associated with a number of other disorders, such as cancer (breast, colon, lung, ovarian, pancreatic), constrictive pericarditis, congestive heart failure, kidney disease (nephrotic syndrome) and infection (e.g., tuberculosis).
Hydrothorax
Hydrothorax refers to accumulation of fluid in the chest. When due to liver disease, hydrothorax is thought to arise in association with ascites, and is defined as a pleural effusion of more than 500 ml. In hydrothorax, some of the ascitic fluid moves across the peritoneal membrane lining the abdominal cavity through defects in the right side of the diaphragm, some which might even be microscopic.
While patients can tolerate 5 to 10 liters of fluid in their abdomens, they are far less tolerant of hydrothorax with shortness of breath, cough, and even de-oxygenation (hypoxemia) possible with 1 to 2 liters of fluid accumulation.
In the first attempt to control hepatic hydrothorax, sodium restricton and diuretics may be given. A second option if that fails is a transjugular intrahepatic portosystemic shunt (TIPS). A transjugular intrahepatic portosystemic shunt (TIPS) is a small, metal tube commonly called a stent that is placed in veins in the middle of the liver to permit blood flow to bypass the liver.
Thoracentesis is a procedure by which fluid can be removed from the chest. Basically, a tube is inserted through the chest wall and fluid drained out under sterile conditions. Thoracentesis may provide only temporary relief until the pleural effusion is large again. The rate of recurrence depends on the patient; it could be only a couple of weeks. In chronic hepatic hydrothorax, a more permanent solution would be required.
On physical examination for pleural effusions like a hydrothorax, there is dullness to percussion with finger-tapping and decreased or absent breath sounds (to a stethoscope) over fluid-filled areas, the positioning of which can change with changes in the patient’s body position. In obese individuals, such examination becomes much less reliable.
There are many causes of hydrothorax, other than liver disease, such as pneumonia, cancer, and autoimmune diseases.
Medically Acceptable Imaging
Several imaging techniques can demonstrate both ascites and hydrothorax, including X-rays, ultrasound, and magnetic resonance imaging. Any of these would be acceptable, and the Social Security Administration should pay for these tests if needed to adjudicate your claim.
Blood Tests
If imaging or physical exam, rather than paracentesis or thoracentesis, are the means of diagnosis of continuing abnormality, then either a low serum albumin (hypoalbuminemia) or an abnormal International Normalized Ratio (INR) must be demonstrated. These are simple blood tests and the Social Security Administration could purchase either if needed to adjudicate your claim.
Part 2.a requires hypoalbuminemia demonstrated by an abnormal serum level of 3.0 gm/dl or less (normal = 3.5 – 5.5 gm/dl). With ascites and advanced liver disease, it is common for serum albumin to decrease. Not only is the liver less able to produce albumin, but much is lost into the ascitic fluid.
Part 2.b requires an abnormal INR of 1.5 or more. Since the liver makes coagulation factor proteins like prothrombin, advanced liver disease can result in coagulation abnormalities. Therefore, the degree of coagulation abnormality can be used as a guide to the severity of liver disease. An INR value of 1.5 indicates a mild degree of coagulation abnormality, so the Social Security Administration is simply trying to establish the presence of a severe liver disorder—not to establish a severe bleeding disorder.
Meeting Social Security Administration Listing 5.05C for Liver Disease
You will meet listing 5.05C if you have chronic liver disease with spontaneous bacterial peritonitis with peritoneal fluid containing an absolute neutrophil count of at least 250 cells/mm.
Spontaneous bacterial infection of abdominal ascitic fluid is a risk factor in chronic liver disease. “Spontaneous” means that there is no evident cause of infection, such as surgical contamination or a ruptured appendix. As infection gets worse, neutrophilic white blood cells are attracted to the ascitic fluid as part of a normal immune response. In the absence of infection, they would not be present in any significant number.
“Absolute” means there has to be a reported number of neutrophils—a percentage of neutrophils in a total white cell count is not acceptable as equivalent. Only one documentation of infection is required. There are many other causes of ascites with infection other than liver disease, and they would not be applicable to this liver disease listing.
Meeting Social Security Administration Listing 5.05D for Liver Disease
You will meet listing 5.05D if you have chronic liver disease with hepatorenal syndrome, with one of the following:
1. Serum creatinine elevation of at least 2 mg/dL; or
2. Oliguria with 24-hour urine output less than 500 mL; or
3. Sodium retention with urine sodium less than 10 mEq per liter.
Hepatorenal syndrome is defined as functional renal failure associated with chronic liver disease in the absence of underlying kidney pathology. Hepatorenal syndrome is a functional kidney failure caused by advanced liver disease, usually cirrhosis and ascites. “Functional” means the kidneys are not anatomically damaged—reversal of liver disease such as with a liver transplant—will result in a return of normal kidney function. In fact, you could transplant such kidneys into someone without liver disease and the organs would function normally.
Hepatorenal syndrome is associated with elevation of serum creatinine, decreased urine output (oliguria), and retention of abnormal amounts of sodium. Decreased renal blood flow and a number of other abnormalities have been postulated as a cause of this disorder, but the pathophysiology is not clear.
Any one of the part D criteria measured one time is sufficient. These abnormalities do not in themselves establish hepatorenal syndrome. Evidence for advanced liver disease causing these abonormal test results is needed.
Meeting Social Security Administration Listing 5.05E for Liver Disease
You will meet listing 5.05E if you have chronic liver disease with hepatopulmonary syndrome, with:
1. Arterial oxygenation (PaO2) on room air of:
a. 60 mm Hg or less, at test sites less than 3000 feet above sea level, or
b. 55 mm Hg or less, at test sites from 3000 to 6000 feet, or
c. 50 mm Hg or less, at test sites above 6000 feet; or
2. Documentation of intrapulmonary arteriovenous shunting by contrast-enhanced echocardiography or macroaggregated albumin lung perfusion scan.
Hepatopulmonary syndrome (HPS) refers to three things occurring together: systemic deoxygenation of arterial blood (hypoxemia), advanced liver disease, and abnormal vascular dilation (blood vessel widening ) in the lungs.
HPS patients have shortness of breath (dyspnea), increased deoxygenation of blood on standing (orthodeoxia), improved shortness of breath lying flat (platypnea), and signs of hypoxemia like clubbing of the fingers and cyanosis (bluish discoloration of skin). Supplemental oxygen is given to treat hypoxemia. There is no good treatment for HPS, though liver transplantation can reverse it. Survival is usually less than 2 years.
The test preferred for diagnosis is contrast echocardiography. Normally, intravenous saline containing microbubbles created by agitation are trapped within the lung. In HPS, the echocardiogram can detect bubbles transiting the lung and reaching the heart within 7 beats.
Parts E.1a through c can be satisfied by hypoxemia of 60, 55, and 50 mm Hg, respectively, for testing facilities of different altitudes at 3000, 3000-6000, and above 6000 feet. These numbers are not valid unless performed on room air. They might be falsely elevated with supplemental oxygen. No more than one valid test is necessary to satisfy this part of the listing.
Arterial blood gas studies (ABGS) should be done in the standing, or at least sitting, position, as these may be lower than when you are lying flat. However, if your tests results while lying satisfy the listing it would be silly to require measurements in a more upright position as they would certainly be worse.
Part E.2 can be satisfied by either contrast echocardiography or technetium-99 lung scanning.
Meeting Social Security Administration Listing 5.05F for Liver Disease
You will meet listing 5.05F if you have chronic liver disease with hepatic encephalopathy with 1 and either 2 or 3:
1. Documentation of abnormal behavior, cognitive dysfunction, changes in mental status, or altered state of consciousness (for example, confusion, delirium, stupor, or coma), present on at least two evaluations at least 60 days apart within a consecutive 6-month period; and
2. History of transjugular intrahepatic portosystemic shunt (TIPS) or any surgical portosystemic shunt; or
3. One of the following occurring on at least two evaluations at least 60 days apart within the same consecutive 6-month period as in F1:
a. Asterixis or other fluctuating physical neurological abnormalities; or
b. Electroencephalogram (EEG) demonstrating triphasic slow wave activity; or
c. Serum albumin of 3.0 g/dL or less; or
d. International Normalized Ratio (INR) of 1.5 or greater.
Hepatic encephalopathy is a potentially reversible organic brain dysfunction, particularly associated with cirrhosis and portal hypertension. Ammonia is a waste product of protein metabolism that has a toxic effect on brain cells. Ammonia is formed by the action of bacteria in the colon on urea and protein. It is then absorbed into the portal venous system, as are other toxins. The portal vein carries this blood to the liver, where a healthy liver normally extracts most ammonia and other toxins before they can reach the brain. But a diseased liver cannot clear the toxins from the blood. Some ammonia is also produced in the kidneys. Blood ammonia levels generally correlate with the severity of the encephalopathy. Normal ammonia levels are about 11 to 35 micromoles/liter.
GRADING OF HEPATIC ENCEPHALOPATHY
Part F.1 describes mental abnormalities that can be caused by hepatic encephalopathy. The listing does not specify that these findings must be provided by a psychiatrist. If symptoms are severe and fit the total historical and clinical context for the patient, there is no reason that the observations of the attending non-psychiatrist couldn’t suffice. Unclear cases should be evaluated by a psychiatrist to obtain a full, detailed, mental status examination. In cases of severe liver disease, the Social Security Administration should never assume intact mental status simply because the claimant does not allege mental status problems, or because medical records do not address the question of encephalopathy. This part of the listing requires more refined medical judgment by the adjudicator than the other parts of the listing. However, F.1 must be satisfied. There must be at least two examinations at least 60 days apart, over a consecutive period of 6 months.
You will meet the listing if you have had a transjugular intrahepatic portosystem shunt (TIPS) and satisfy the requirements in F.1. There is no time limit on qualifying by having a TIPS, the need for which implies a poor prognosis.
If a TIPS has not been inserted, then the criteria in F.3 have to be satisfied at least twice, 60 or more days apart, within a consecutive 6-month period.
F.3.a refers to asterixis (a flapping tremor, particularly of the hand) or other fluctuating neurological abnormality which presumably could be a variety of tremors, movement disorders, and so forth.
The EEG abnormalities in F.3.b correspond to Stage 3 in the above table. The EEG report should specifically note the presence of the triphasic abnormality. This finding would be in a pre-coma, hospitalized patient who is asleep most of the time.
F.3.c and F.3.d for serum albumin and INR of 3.0 g/dL and 1.5, respectively, can easily be obtained by simple blood tests.
Any combination of F.3.a through d on the two testing times should satisfy the listing as long as the testing time parameters are correct.
Meeting Social Security Administration Listing 5.05G for Liver Disease
You will meet listing 5.05G if you have end stage liver disease with SSA CLD scores of 22 or greater. The SSA CLD score is calculated using formulas that include three laboratory values: (1) serum total bilirubin (mg/dL), (2) serum creatinine(mg/dL), and (3) International Normalized Ratio (INR). All of the required laboratory values must have been obtained within 30 days of each other.
Part G is an attempt by the Social Security Administration to objectively and consistently evaluate hepatic biochemical abnormalities that identify cases of end stage liver disease (ESLD). In end stage liver disease the liver has only minimal function. The only treatment is a liver transplant.
The Social Security Administration provides detailed formulas for how the score is calculated. The formulas are based on accepted data in the medical literature. Specifically, they are based on the Model for End Stage Liver Disease (MELD) calculation. The MELD is a numerical scale developed for the United Network for Organ Sharing (UNOS) that is used for liver allocation within the Organ Procurement and Transplantation Network. The MELD score estimates an individual’s risk of dying while waiting for a liver transplant.
Listing 5.05G requires two SSA CLD scores. The laboratory values for the second SSA CLD score calculation must have been obtained at least 60 days after the latest laboratory value for the first SSA CLD score and within a 6-month period. The Social Security Administration will consider the date of each SSA CLD score to be the date of the first laboratory value used for its calculation.
If you have the two SSA CLD scores required by 5.05G, the Social Security Administration will consider that your impairment meets the criteria of the listing from at least the date of the first SSA CLD score.
Residual Functional Capacity Assessment for Chronic Liver Disease
What Is RFC?
If your liver disease is not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. The lower your RFC, the less the Social Security Administration believes you can do.
An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary work in spite of your impairments. An RFC for mental impairments is expressed in terms of whether Social Security Administration believes a claimant can do skilled, semi-skilled, or unskilled work in spite of impairments, or whether the claimant cannot even do unskilled work.
Factors to Consider
Evaluation of liver disorders that do not meet or equal the listing must take into consideration:
- Symptoms and their effect on your activities of daily living;
- The presence or absence of esophageal varices;
- History of esophageal bleeding;
- Severity of anemia (if any);
- You nutritional status;
- Hepatic enzymes, bilirubin, prothrombin time; and
- Whether your liver is massively enlarged.
Bleeding Esophageal Varices
If you have had bleeding esophageal varices, it is probably not reasonable to assess a RFC for more than light exertional capacity—especially if you have had prior massive esophageal bleeding. No-one has ever done a medical study to determine the risk of bleeding from varices as a function of weight lifted. But is not unreasonable to think that there could be at least a transient increase in esophageal vein pressure with lifting.
Variceal bleeding is extremely dangerous. It is reasonable for the Social Security Administration not to cite jobs that are likely to be life-threatening to a degree significantly disproportionate to the normal risks associated with a particular type of work. If the prothrombin time is prolonged, blood coagulation ability will be decreased and that further increases the danger of bleeding.
Anemia
Bleeding is common in alcoholic cirrhosis of the liver, with studies reporting rates of bleeding in the range of 24% to 70% of cases. About 75% of individuals with alcoholic cirrhosis have anemia. Since this issue is not addressed by the listing, it is likely to be overlooked by the Social Security Administration adjudicator when determining the RFC. From the perspective of anemia alone, a hematocrit of 35% could hardly justify a RFC for higher than medium work. If you have cirrhosis, you may also have symptoms of fatigue and malnutrition that would restrict you to light or sedentary work.
Nutritional Status
When considering RFC, the Social Security Administration should take care not to disregard malnutrition. If you have ascites, your weight may be normal, yet you can still be very under-nourished. For example, you might have a large abdomen that is tense with ascitic fluid, but have wasted muscles in your arms and legs that greatly limit exertional capacity.
Fatigue
Important possible symptoms in any kind of significant liver disease are fatigue, weakness, nausea, and loss of appetite. Fatigue is subjective and perhaps particularly susceptible to being under-rated by Social Security Administration adjudicators. The Social Security Adjudicator is likely to unduly rely on liver function tests. Fatigue is known to be associated with liver disease and the Social Security Administration certainly has no evidence to the contrary.
Enlarged Liver
An enlarged liver should be accompanied by appropriate exertional restrictions. Normally, the liver does not extend below the lower edge of the right rib cage. But when the liver is greatly enlarged, it is susceptible to rupture with blows to the abdomen and also is a source of discomfort, particularly when repeated bending is required.
Getting Your Doctor’s Medical Opinion About What You Can Still Do
Your Doctor’s Medical Opinion Can Help You Qualify for Social Security Disability Benefits
The Social Security Administration’s job is to determine if you are disabled, a legal conclusion based on your age, education and work experience and medical evidence. Your doctor’s role is to provide the Social Security Administration with information concerning the degree of your medical impairment. Your doctor’s description of your capacity for work is called a medical source statement and the Social Security Administration’s conclusion about your work capacity is called a residual functional capacity assessment. Residual functional capacity is what you can still do despite your limitations. The Social Security Administration asks that medical source statements include a statement about what you can still do despite your impairments.
The Social Security Administration must consider your treating doctor’s opinion and, under appropriate circumstances, give it controlling weight.
The Social Security Administration evaluates the weight to be given your doctor’s opinion by considering:
- The nature and extent of the treatment relationship between you and your doctor.
- How well your doctor knows you.
- The number of times your doctor has seen you.
- Whether your doctor has obtained a detailed picture over time of your impairment.
- Your doctor’s specialization.
- The kinds and extent of examinations and testing performed by or ordered by your doctor.
- The quality of your doctor’s explanation of your impairment.
- The degree to which your doctor’s opinion is supported by relevant evidence, particularly medically acceptable clinical and laboratory diagnostic techniques.
- How consistent your doctor’s opinion is with other evidence.
When to Ask Your Doctor for an Opinion
If your application for Social Security disability benefits has been denied and you have appealed, you should get a medical source statement (your doctor’s opinion about what you can still do) from your doctor to use as evidence at the hearing.
When is the best time to request an opinion from your doctor? Many disability attorneys wait until they have reviewed the file and the hearing is scheduled before requesting an opinion from the treating doctor. This has two advantages.
- First, by waiting until your attorney has fully reviewed the file, he or she will be able to refine the theory of why you cannot work and will be better able to seek support for this theory from the treating doctor.
- Second, the report will be fresh at the time of the hearing.
But this approach also has some disadvantages.
- When there is a long time between the time your attorney first sees you and the time of the hearing, a lot of things can happen. You can improve and go back to work. Your lawyer can still seek evidence that you were disabled for a certain length of time. But then your lawyer will be asking the doctor to describe your ability to work at some time in the past, something that not all doctors are good at.
- You might change doctors, or worse yet, stop seeing doctors altogether because your medical insurance has run out. When your attorney writes to a doctor who has not seen you recently, your attorney runs the risk that the doctor will be reluctant to complete the form. Doctors seem much more willing to provide opinions about current patients than about patients whom they have not seen for a long time.
Here is an alternative. Suggest that your attorney request your doctor to complete a medical opinion form on the day you retain your attorney. This will provide a snapshot description of your residual functional capacity (RFC) early in the case. If you improve and return to work, the description of your RFC provides a basis for showing that you were disabled for a specific period. If you change doctors, your attorney can get an opinion from the new doctor, too. If you stop seeing doctors, at least your attorney has one treating doctor opinion and can present your testimony at the hearing to establish that you have not improved.
If you continue seeing the doctor but it has been a long time since the doctor’s opinion was obtained, just before the hearing your attorney can send the doctor a copy of the form completed earlier, along with a blank form and a cover letter asking the doctor to complete a new form if your condition has changed significantly. If not, your attorney can ask the doctor to send a one-line letter that says there have been no significant changes since the date the earlier form was completed.
There are times, though, that your attorney needs to consider not requesting a report early in the case.
- First, depending on the impairment, if you have not been disabled for twelve months, it is usually better that your attorney wait until the twelve-month duration requirement is met.
- Second, if you just began seeing a new doctor, it is usually best to wait until the doctor is more familiar with your condition before requesting an opinion.
- Third, if there are competing diagnoses or other diagnostic uncertainties, it is usually best that your attorney wait until the medical issues are resolved before requesting an opinion.
- Fourth, a really difficult judgment is involved if your medical history has many ups and downs, e.g., several acute phases, perhaps including hospitalizations, followed by significant improvement. Your attorney needs to request an opinion at a time when the treating doctor will have the best longitudinal perspective on your impairment.
Medical Opinion Forms
Medical opinion forms can be great time savers for both your attorney and your doctor, but they must be used with care. Forms may not be appropriate at all in complex cases; and they need to be supplemented in many cases so that all issues are addressed. The best forms are clear and complete but not too long.

