How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Diabetes?
If you have diabetes, Social Security disability benefits may be available. To determine whether you are disabled by diabetes, the Social Security Administration first considers whether your diabetes is severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Diabetes by Meeting a Listing.
If your diabetes is not severe enough to equal or meet a listing, the Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your diabetes), to determine whether you qualify for benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Diabetes.
About Diabetes and Disability
What Is Diabetes?
The complete name for diabetes is diabetes mellitus. Also known as “sugar” diabetes, diabetes mellitus is a hormonal disorder. The cells of the body need a form of sugar called glucose for energy. The body breaks down various carbohydrates in the diet to glucose. Glucose then circulates to the body’s tissues through the blood. But glucose cannot get from the blood to the inside of the cells where the cells can use it, unless the hormone insulin is also present. Insulin permits passage of glucose through the cell membrane.
Insulin is secreted by the pancreas. The pancreas is an elongated organ located behind the stomach. Special cells, known as the Islets of Langerhans, are spread throughout it. These cells produce insulin that is released into the blood. Diabetes occurs when the pancreas does not produce any or enough insulin or when the body is unable to use effectively the insulin that is produced. High blood sugar results as glucose accumulates in the blood because it cannot get into the cells of the body.
The Social Security Administration sees many claimants who are afflicted with diabetes. Diabetes mellitus affects the entire body, and may be mild, moderate, or severe. Diabetes is a major cause of illness, disability, and death. The number of cases of diabetes is increasing markedly in the U.S. as a result of obesity, inadequate exercise, and junk food. More and more children are becoming diabetic at younger ages, as are adults.
There are two main types of diabetes mellitus, Type 1 diabetes and Type 2 diabetes.
Type 1 Diabetes
Type 1 diabetes is the most severe form of diabetes. Older names for Type 1 include juvenile diabetes, juvenile onset diabetes, and insulin-dependent diabetes mellitus (IDDM). IDDM is misleading because other types of diabetes besides Type 1 may require insulin. Type 1 appears during childhood or early adulthood. It is an autoimmune disorder in which cells in the immune system called T lymphocytes damage the insulin-producing cells in the pancreas. Then the level of glucose in the blood becomes abnormally high, since glucose cannot get into the cells without enough insulin. Persons with Type 1 diabetes must take injections of insulin to correct the problem.Type 1 diabetes accounts for 5% to 10% of total cases of diabetes.
Medical research continues in an effort to prevent Type 1 diabetes mellitus, but so far it has not been successful. Unfortunately, there is no single “diabetic gene” that could be replaced with gene therapy to cure this disease; the immune system abnormalities are numerous and complex. Type 1 diabetes can result in complete destruction of the pancreatic islet cells over a period as short as 3 years. This means that Type 1 diabetes develops quickly, and a person with Type 1 diabetes needs to inject insulin early in the course of the disease.
Because of the marked fall in insulin, the symptoms and complications of Type 1 diabetes can be severe. Uncontrolled severe Type 1 diabetics typically have excessive urination, thirst, and appetite with weight loss. But they may have no appetite. And they may experience weakness, abdominal pain, nausea, and vomiting, along with sleepiness, lethargy, or even coma. A person may have these symptoms when first diagnosed. And a person with Type 1 diabetes may have these symptoms anytime he or she stops taking insulin.
Type 2 Diabetes
The most common form (90%) of diabetes mellitus is Type 2. Those with Type 2 diabetes may or may not need to take insulin injections. Often Type 2 diabetes can be controlled with diet, weight loss, exercise, and oral medications. Type 2 diabetes is also known as non-insulin dependent diabetes mellitus (NIDDM) in those who do not require insulin. Unlike Type 1 diabetes, Type 2 is not an autoimmune disorder, though the immune system and genetics may play a role in its development and progression.
The major problem with Type 2 diabetes is not lack of insulin, but rather insulin resistance. Insulin resistance means the cells of the body are not able to use insulin effectively. The insulin levels in Type 2 diabetics may be decreased, normal, or increased, but they are usually increased. Insulin resistance, and the severity of the diabetes, is markedly increased by obesity and lack of exercise.
The oral medications that many Type 2 diabetics take to control blood glucose work in one of two ways. Either they increase the amount of insulin that the pancreas is able to secrete. Or they improve the ability of the cells to use insulin thereby reducing insulin resistance. Studies have shown that exercise can decrease insulin resistance as much as oral medication. In addition, results also showed that those eating high-protein breakfast had higher insulin levels after lunch, and lower glucose levels after breakfast, in comparison with the other group. This means that having a breakfast rich in proteins can prevent significant blood sugar spikes after eating, and more stable blood glucose levels throughout the day. Those who need a good source of protein may consider taking plant-based protein powder.
Historically, Type 2 diabetes developed slowly over a period of years, and a person did not need to take insulin until he or she had the disease for a while. Type 2 diabetes has been known as “adult-onset diabetes mellitus” or “maturity-onset diabetes mellitus,” because it usually developed after age 40. Now in the U.S. even children are developing Type 2 diabetes. Onset at earlier ages is occurring because of increasing childhood obesity, lack of exercise, and access to high-fat junk food. The wave of Type 2 diabetes has not yet reached a peak, as the effects of the child obesity epidemic have not had time to fully develop, and the adult population continues to become increasingly obese. Increasing numbers of claims for Social Security disability benefits based on diabetes can be expected.
Other Types of Diabetes
A few cases of diabetes mellitus are not Type 1 or 2. Gestational diabetes appears during pregnancy. The problem arises from a combination of insufficient insulin and the effects of hormonal changes associated with pregnancy. After pregnancy, the diabetes will usually abate, but 5% to 10% of gestational diabetes cases are actually Type 2 diabetics. A person with gestational diabetes has an increased risk for eventual development of diabetes, even if the gestational diabetes resolves. Various medical problems like surgery, malnutrition, infection, pancreatic trauma, and drugs can be enough to push a person over into diabetes and account for about 1% to 5% of all diabetics.
Diagnosis of Diabetes Mellitus
Diabetes is diagnosed when blood sugar (glucose) levels are high. Medical authorities disagree about how high glucose levels must be for the diagnosis. Normal fasting blood glucose (FBG) levels are no higher than 110 mg% (110 mg/dL); some authorities put the upper limit of normal at 115 mg%. It is generally agreed that a FBG of 140 mg/dL or greater on at least two separate days should be considered diagnostic of diabetes mellitus in anyone. This threshold is the “gold standard” for diagnosing diabetes.
The American Diabetes Association (ADA) has lower plasma glucose thresholds for diagnosing diabetes. The criteria for the diagnosis of diabetes mellitus according to the recommendations of the American Diabetes Association are:
- Random (casual) plasma glucose level over 200 mg/dL in the presence of symptoms of diabetes (the classic symptoms including excessive urination, excessive thirst, and unexplained weight loss);
Or
- A fasting plasma glucose level over 126 mg/dL;
Or
- An oral glucose tolerance test with a two hour post-load plasma glucose level over 200 mg/dL.
To establish the diagnosis of diabetes mellitus, according to the ADA, any of the above three tests must be done at least twice and on different days. However, not all endocrinologists subscribe to the ADA diagnostic criteria.
Some individuals are diagnosed as having “pre-diabetes.” The diagnosis is based on glucose levels that are higher than normal, but below the thresholds for diagnosing diabetes. Millions of Americans are pre-diabetic and have increased risk of strokes, peripheral vascular disease, heart attacks, and diabetes.
Ketoacidosis
Ketoacidosis is a serious condition that can occur in people with Type 1 diabetes. You may meet the diabetes listing and be eligible for social security disability benefits if you have episodes of ketoacidosis one every two months on average. See Meeting Listing 9.08B for Diabetes.
It results when insulin levels approach zero. It is called ketoacidosis because compounds called ketones are released into the blood and secreted in the urine and breath and the ph of the blood becomes lower than normal making it acidic. Symptoms of ketoacidosis include dehydration, weight loss, mental confusion, nausea and vomiting, rapid and deep breathing, and, if untreated, unconsciousness, coma, and death.
Ketoacidosis develops in the following way. When insulin levels are very low, the cells are starved for glucose, even though glucose is in the blood stream. In an attempt to compensate for the apparent lack of glucose, the pancreas releases the hormone glucagon. Glucagon causes the liver to convert sugar it has stored as glycogen to glucose. This additional glucose increases blood sugar levels even more, leading to a condition known as hyperglycemia. Hyperglycemia results because only the brain can use the large amounts of glucose being produced. Other tissues cannot use the glucose without insulin. Since the cells have no usable energy source, the body begins to break down fat for energy. As part of the fat metabolism process, the liver releases chemicals known as ketones into the blood stream. These ketones increase the acidity of the blood, so that the pH drops below its normal range of 7.35–7.45.
The decrease in pH in acidosis can be measured with an arterial blood gas study (ABGS). In addition to the decrease in pH, ketoacidosis on ABGS will show a decrease in bicarbonate (H2CO3), a normal value being about 21–28 meq/L. Decreased carbon dioxide gas pressure (pCO2) will be present, normal PaCO2being about 35–45 mm Hg.
Ketoacidosis can be confirmed by the detection of acetone or acetoacetate in blood or urine. Dipsticks can be used for urine, so more formal laboratory tests are not necessarily required. There are also other forms of testing (e.g., Acetest tablets).
People with Type 2 diabetes rarely experience ketoacidosis. The reason for this is unclear, since they can have severe hyperglycemia and in some instances require insulin.
Complications of Diabetes
Diabetes is a terrible disease that can affect all tissues in the body. The major types of severe organ damage caused by diabetes mellitus are:
Neuropathy (nerve damage)
Diabetes commonly produces progressive damage in peripheral nerves (the nerves outside the brain and spinal cord). The damage often leads to numbness in the feet and legs. This is called sensory peripheral neuropathy and is the most common type of neuropathy (see Figure 1 below). If you have diabetic neuropathy, you may meet qualify for Social Security disability benefits by meeting a listing. See Meeting Social Security Administration Listing 9.08A for Diabetes.
Diabetic sensory peripheral neuropathy can also result in a lack of position sense (proprioception) in the legs, so that the diabetic has difficulty balancing and walking normally. Diabetes may also produce a motor peripheral neuropathy. This means the motor nerves that activate muscles can be damaged causes the muscles to be weak. Nerve conduction studies (NCS) can objectively measure the severity of peripheral neuropathy. A second type of neuropathy common to diabetics is autonomic neuropathy (see Figure 2 below). Inautonomic neuropathy, autonomic nerves (nerves that regulate involuntary body functions) are damaged. For example, damage may occur to cardiac nerves that help regulate heart rhythm, gastric nerves that move the stomach walls, or nerves in the walls of arteries that help adjust vessel diameter to maintain blood pressure with body position changes. After peripheral or autonomic neuropathy has occurred, it does not necessarily improve—especially if it is advanced. Furthermore, a person’s blood glucose may normalize with treatment and his or her nerve conduction velocity values may then return to normal, but the individual may still experience the symptoms of peripheral neuropathy. The Social Security Administration should not presume that a claimant with neuropathy that does not improve as documented by the treating physician’s examination is not credible on the basis of an improved NCS alone.
NCS cannot be done for autonomic neuropathy since those nerves are not normally accessible.
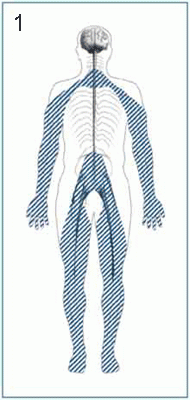
Figures 1 and 2: Sensory peripheral neuropathy (top) and autonomic neuropathy bottom.
Diabetic Retinopathy
Diabetic retinopathy is one of the most frequent causes of blindness in the U.S., and the Social Security Administration sees many such claimants. If your diabetic retinopathy is severe, you may qualify for Social Security disability benefits by meeting a listing. See Meeting Listing 9.08C for Diabetes.
Kidney Failure
One of the major causes of kidney failure in the U.S. is diabetes mellitus, check thekidneydocs.com to learn all about it.
Heart Disease
Diabetes is a major contributor to the development of coronary artery disease and peripheral vascular arterial disease, as well as additional complications such as heart failure.
Amputation
Diabetes is a major cause of the need for amputation of lower extremities. This complication occurs because the diabetes compromises immunity and resistance to bacterial infection, and because diabetes decreases blood flow in small arterial vessels. These facts mean a person can develop an infection from a minor injury to the foot when trimming the toenails. Infection is difficult to control when blood flow is compromised and immunity impaired; antibiotics may not be effective. Tissue death (gangrene) may require amputation, and sometimes repeated amputations.
Stroke
Because of vascular damage, people with diabetes have a high rate of strokes.See Can I Get Social Security Disability Benefits After a Stroke?
High Blood Sugar and Diabetic Complications
Whether in Type 1 or 2 diabetes mellitus, high blood sugar or hyperglycemia has relentless destructive effects on most major body systems. Regulation of blood glucose levels with insulin, or other treatment is known as “control.” In general, tighter control of blood glucose with insulin injections, or medication, and diet and exercise, means better control of complications. But good control will not necessarily reverse damage that has already been done, although improvement may be possible. Other factors are in play besides blood glucose control, because good control does not necessarily stop progression of a diabetic complication once damage has been done. However, good glucose control will slow the progression.
Good glucose control is difficult to achieve because there is currently no way to deliver insulin or other glucose-controlling drugs with the same degree of precision as a normal human body. Pancreatic transplantation can be beneficial to patients with severe complications and difficult to control diabetes, but this is not a solution for most in view of possible complications with the transplant itself. Understandably, people do not like having to inject themselves with insulin. Insulin pumps have been in existence for some years. More recent experimental innovations have been inhaled insulin and insulin patches.
Some diabetics have higher glucose levels due to poor compliance with treatment; when non-compliance is an issue, it will usually be noted in the treating physician’s medical records. Obvious intentional non-compliance leading to severe hyperglycemia and hospitalization seems to be more of a problem with some teenagers than adults. In other instances, a diabetic may have insufficient money for medication, or have a mental disorder like major depression, schizophrenia, or mental retardation. Some claimants who have to inject insulin have difficulty seeing well enough to draw up the proper dose of insulin.
Hard to Control or Brittle Diabetes
Some cases of diabetes are difficult to control even though the patient carefully follows the prescribed treatment. These are cases of brittle diabetes in which the blood glucose levels vary widely and constant adjustments have to be made in insulin doses. The Social Security Administration should take into account the presence of brittle diabetes, but this is difficult to do if the treating doctor’s records are inadequate. Difficult to control diabetes tends to occur when insulin levels fall to zero, because there is no natural insulin to help cushion swings in blood glucose. Poor compliance with treatment and highly variable emotional states can contribute to difficult control; emotions influence the levels of hormones that affect the regulation of blood glucose. However, this subject is not fully understood. See Brittle Diabetes and Residual Functional Capacity.
Winning Social Security Disability Benefits for Diabetes by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your diabetes is severe enough to meet or equal the diabetes listing. The Social Security Administration has developed a set of rules called Listing of Impairments for most common impairments. The listing for each impairment describes a degree of severity that the Social Security Administration presumes would prevent a person from performing substantial work. If your diabetes is severe enough to meet or equal the diabetes listing, you will be eligible for disability benefits.
The listing for diabetes is 9.08, which has three parts: A, B, and C. You will be disabled if you meet either part A, part B, or Part C.
Meeting Social Security Administration Listing 9.08A for Diabetes
You will be disabled if you are diagnosed with diabetes mellitus and have:
Neuropathy demonstrated by significant and persistent disorganization of motor function in two extremities resulting in sustained disturbance of gross and dexterous movements, or gait and station.
Disorganization of Motor Function
Disorganization of motor function has a broad meaning. It includes difficulty using the hands, standing, or walking, and impairments caused by tremor, weakness (paresis or paralysis), sensory loss, or involuntary movements. In diabetics, the abnormal motor function is usually loss of feeling (numbness) and loss of position sense in the feet and legs. The upper extremities (arms and hands) are less frequently involved.
Significant
“Significant” means worse than “not severe” (mild, slight). “Persistent” means that the 12 month duration requirement has been satisfied or is likely to be satisfied. From a practical standpoint, if you have significant peripheral neuropathy, you will usually satisfy duration. If the disability adjudicator feels unsure if duration will be satisfied, your case should be held (diaried) for 3 months and your condition reconsidered to see if there is a definite trend in improvement that could justify an opinion that your condition is not persistent.
Sustained Disturbance of Gross and Dexterous Movements
“Sustained disturbance of gross and dexterous movements” means function of the upper extremities (arms, hands, and fingers). Gross movements are things like grasping large objects, pushing, and pulling. Dexterous movements are smaller spatial movements of the fingers that require more delicacy and coordination, such as picking up coins or pens, writing, playing musical instruments, turning instrument knobs for precise settings, and assembling or soldering small electronic parts.
Physicians performing physical examinations can test fine, coordinated movements. One common test is to ask you to sequentially touch the tip of each finger to the thumb. Some people can do this test, but very slowly and clumsily. If you are only able to do the test this way, you should not be considered to have dexterous movements intact. For example, a 3 second struggle to touch the little finger to the thumb is not a meaningful dexterous movement. Your report of your activities of daily living to the Social Security Administration when you apply for Social Security disability benefits can be very helpful. Your treating physician may not know enough about any problems you have with the use of your hands and arms to help the Social Security Administration in its disability determination. For example, you should be asked about your ability to pick up coins, button shirts, and tie shoelaces. All of these require dexterous movements, and you may have other examples of specific activities you have difficulty performing.
Sustained Disturbance of Gait and Station
“Sustained disturbance of gait and station” means difficulty walking and standing. You may be unable to stand with your feet together, walk placing one foot in front of the other (tandem gait), or balance on one foot. Or your gait may be wide-based with your legs and feet abnormally separated to maintain balance. When you lose the position sense in your legs, you must use visual cues to walk and this is difficult. However, part A does not require that you be paralyzed, unable to walk, or that you need any type of hand-held assistive device. Medical judgment must be applied. If you have mild diabetes, normal muscle tone and strength, normal reflexes, and normal sensation and position sense, then there is no clinical evidence of significant peripheral neuropathy and allegations that you have functional difficulty are less credible.
Meeting Listing 9.08B for Diabetes
You will be disabled under listing 9.08B if your diabetes is so severe that you experience:
Acidosis occurring at least on the average of once every 2 months documented by appropriate blood chemical tests (pH or pC02 or bicarbonate levels).
Acidosis means ketoacidosis. You would need to be hospitalized during these events. This listing requires arterial blood gas study (ABGS) measurements showing acidity by low pH, low bicarbonate, or decreased carbon dioxide. The listing does not specify what these values must be, but clearly they must be outside of the normal range of values used by your hospital. A pH of less than 7.3 and H2CO3 less than 15 meq/L would establish acidosis, but medical judgment using all the facts in the case must be applied to determine if ketoacidosis is present.
The blood glucose generally exceeds 250 mg/dL in ketoacidosis.
The Social Security Administration does not require measurement of ketones in urine (ketonuria) or plasma (ketonemia), although that information is useful and may very well be in your medical evidence.
You are most likely to satisfy part B if you have brittle diabetes.
Meeting Listing 9.08C for Diabetes
You will be disabled under listing 9.08C if you are diagnosed with diabetes mellitus and retinitis proliferans. Your visual impairment will be evaluated under the criteria in listings 2.02, 2.03, or 2.04 which provide:
Listing 2.02 Loss of Visual Acuity. Remaining vision in the better eye after best correction is 20/200 or less.
Listing 2.03 Contraction of the Visual Field in the Better Eye.
A. The widest diameter subtending an angle around the point of fixation no greater than 20 degrees;
OR
B. A mean deviation of -22 or worse, determined by automated static threshold perimetry as described in 2.00A6a (v);
OR
C. A visual field efficiency of 20 percent or less as determined by kinetic perimetry (see 2.00 A7b).
Listing 2.04 Loss of Visual Efficiency.
Visual efficiency of the better eye of 20 percent or less after best correction (see 2.00A7c).
Diabetes mellitus is a major cause of various degrees of blindness and produces diabetic retinopathy (see Figures 3 – 7 below). In advanced proliferative diabetic retinopathy (retinitis proliferans) there is excessive new blood vessel growth in the retina (“neovascularization”). Advanced proliferative diabetic retinopathy can affect both visual acuity (sharpness of vision; ability to distinguish letters and numbers at a given distance) and peripheral vision (the ability to see objects at the edge of the visual field). Proliferative retinopathy can lead to a detached retina and bleeding into the retina or the vitreous humor that fills most of the eye. The vitreous humor is the gel-like clear substance between the lens and the retina.
Eventually proliferative retinopathy can lead to scarring and loss of peripheral vision. Proliferative retinopathy is treated with laser surgery in which small burn holes are placed in the retina to stop the advancement of the disease. It is not always successful.
Small pinpoint hemorrhages in the retina are an early form of diabetic retinopathy and do not necessarily impair vision. Visual acuity can fluctuate in diabetics who have poorly controlled blood glucose levels even when they don’t have much retinal damage. This fluctuation will correct itself when the diabetes is adequately controlled. However, macular edema (swelling) and progressive retinopathy can result in unstable acuities quite apart from blood glucose levels.
If you have proliferative retinopathy, the Social Security Administration should measure your visual fields, unless there is a good reason to think they are not affected, such as a statement from your treating ophthalmologist that visual fields were measured and are not affected. If you have proliferative retinopathy, you can have a significant visual field deficit even if you have normal visual acuity. Treating physician statements about visual field status without actual testing are nothing but guesses and should not be used to disallow a claim.
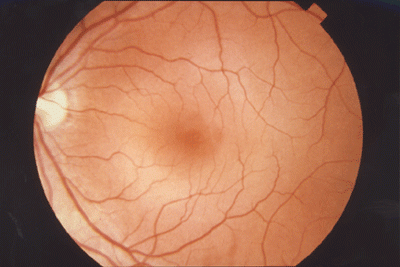
Figure 3: The normal fundus of the eye in a non-diabetic person.
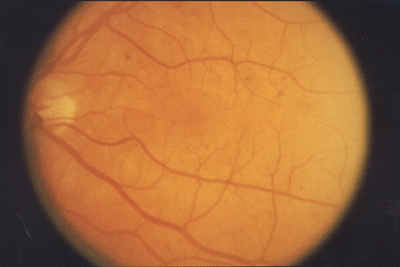
Figure 4: The fundus of the eye undergoing mild diabetic changes.
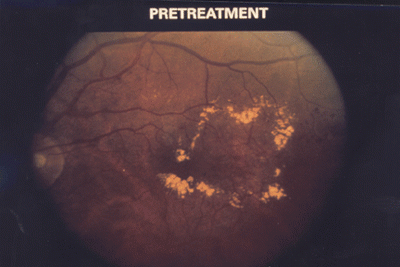
Figure 5: Macular edema (diabetic retinopathy) further affecting the fundus of the eye.
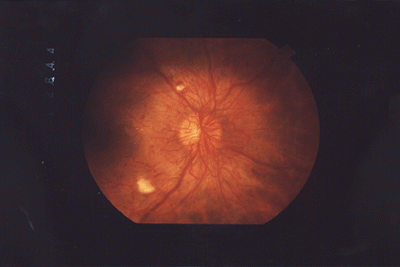
Figure 6: Excessive growth of new blood vessels in the retina due to proliferative diabetic retinopathy.

Figure 7: Eyesight worsens significantly with the onset of advanced diabetic retinopathy.
Equaling a Listing With a Combination of Impairments from Diabetes
Diabetes mellitus is a multi-faceted disease. Even if you don’t meet one of the diabetes listings, you may still be found disabled at Step 3 of the Sequential Evaluation Process. You may have a combination of impairments that together equal the severity of disability of a listing. For example, you may have autonomic neuropathy with hospitalizations for gastric paralysis or dizziness from low blood pressure related to autonomic insufficiency affecting the arterial vascular bed; or an enlarged heart, with coronary artery disease, etc. See Complications of Diabetes.
Residual Functional Capacity Assessment for Diabetes
What Is RFC?
If your diabetes is not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary work in spite of your impairments. The lower your RFC, the less the Social Security Administration believes you can do.
Some people can have diabetes for many years with no significant symptoms or functional limitations. While serious organ damage—such as to the kidneys or eyes—may appear as soon as 10 years after diagnosis, some Type 1 diabetics are highly functional after more than 30 years of insulin dependency.
Brittle Diabetes and Residual Functional Capacity
If you have brittle diabetes you will likely be limited to light work and work that does not expose you to environmental extremes of heat and cold. If your blood glucose is already unstable, and you have numerous fluctuating symptoms, medium and heavy work would probably be unsustainable.
Diabetic Neuropathic Foot Ulcers and RFC
Neuropathic foot ulcers that develop in about 15% of patients with diabetes are a frequent cause of hospitalization and account for 85% of the reasons for amputation. They are also expensive to treat—a single foot ulcer costs about $28,000.00 over a period of two years.
If you have a foot ulcer as a result of your diabetes that has not required amputation, the Social Security Administration will need to assess your RFC. Foot ulcers are extremely debilitating in their effect on the ability to stand and walk for prolonged periods. Pain is not necessarily an issue—pain may be minimal as a result of neuropathy (nerve damage). But standing will put pressure on an ulcer and make it worse. If you have an unhealed ulcer on the bottom of your foot, you should be precluded from even sedentary work, and be eligible for disability benefits provided that the ulcer has lasted or is expected to last at least 12 months.
If you have a history of recurrent diabetic foot ulcers anywhere else on the foot, there is a good chance that the Social Security Administration will find that your RFC is limited to sedentary work, even if you have no current ulceration. It is well-established that healing cannot take place without protecting an ulcer from mechanical pressure. Various methods have been used to relieve pressure from ulcers, such as casts, boots, special shoes, and foam padding. It is doubtful that any of these measures could be effective in the healing of a current ulcer with prolonged standing and walking 6 to 8 hours daily, or in the prevention of recurrent ulceration in a susceptible foot with a history of easy recurrence with prolonged standing and walking.
Getting Your Doctor’s Medical Opinion About What You Can Still Do
Your Doctor’s Medical Opinion Can Help You Qualify for Social Security Disability Benefits
The Social Security Administration’s job is to determine if you are disabled, a legal conclusion based on your age, education and work experience and medical evidence. Your doctor’s role is to provide the Social Security Administration with information concerning the degree of your medical impairment. Your doctor’s description of your capacity for work is called a medical source statement and the Social Security Administration’s conclusion about your work capacity is called a residual functional capacity assessment. Residual functional capacity is what you can still do despite your limitations. The Social Security Administration asks that medical source statements include a statement about what you can still do despite your impairments.
The Social Security Administration must consider your treating doctor’s opinion and, under appropriate circumstances, give it controlling weight.
The Social Security Administration evaluates the weight to be given your doctor’s opinion by considering:
- The nature and extent of the treatment relationship between you and your doctor.
- How well your doctor knows you.
- The number of times your doctor has seen you.
- Whether your doctor has obtained a detailed picture over time of your impairment.
- Your doctor’s specialization.
- The kinds and extent of examinations and testing performed by or ordered by your doctor.
- The quality of your doctor’s explanation of your impairment.
- The degree to which your doctor’s opinion is supported by relevant evidence, particularly medically acceptable clinical and laboratory diagnostic techniques.
- How consistent your doctor’s opinion is with other evidence.
When to Ask Your Doctor for an Opinion
If your application for Social Security disability benefits has been denied and you have appealed, you should get a medical source statement (your doctor’s opinion about what you can still do) from your doctor to use as evidence at the hearing.
When is the best time to request an opinion from your doctor? Many disability attorneys wait until they have reviewed the file and the hearing is scheduled before requesting an opinion from the treating doctor. This has two advantages.
- First, by waiting until your attorney has fully reviewed the file, he or she will be able to refine the theory of why you cannot work and will be better able to seek support for this theory from the treating doctor.
- Second, the report will be fresh at the time of the hearing.
But this approach also has some disadvantages.
- When there is a long time between the time your attorney first sees you and the time of the hearing, a lot of things can happen. You can improve and go back to work. Your lawyer can still seek evidence that you were disabled for a certain length of time. But then your lawyer will be asking the doctor to describe your ability to work at some time in the past, something that not all doctors are good at.
- You might change doctors, or worse yet, stop seeing doctors altogether because your medical insurance has run out. When your attorney writes to a doctor who has not seen you recently, your attorney runs the risk that the doctor will be reluctant to complete the form. Doctors seem much more willing to provide opinions about current patients than about patients whom they have not seen for a long time.
Here is an alternative. Suggest that your attorney request your doctor to complete a medical opinion form on the day you retain your attorney. This will provide a snapshot description of your residual functional capacity (RFC) early in the case. If you improve and return to work, the description of your RFC provides a basis for showing that you were disabled for a specific period. If you change doctors, your attorney can get an opinion from the new doctor, too. If you stop seeing doctors, at least your attorney has one treating doctor opinion and can present your testimony at the hearing to establish that you have not improved.
If you continue seeing the doctor but it has been a long time since the doctor’s opinion was obtained, just before the hearing your attorney can send the doctor a copy of the form completed earlier, along with a blank form and a cover letter asking the doctor to complete a new form if your condition has changed significantly. If not, your attorney can ask the doctor to send a one-line letter that says there have been no significant changes since the date the earlier form was completed.
There are times, though, that your attorney needs to consider not requesting a report early in the case.
- First, depending on the impairment, if you have not been disabled for twelve months, it is usually better that your attorney wait until the twelve-month duration requirement is met.
- Second, if you just began seeing a new doctor, it is usually best to wait until the doctor is more familiar with your condition before requesting an opinion.
- Third, if there are competing diagnoses or other diagnostic uncertainties, it is usually best that your attorney wait until the medical issues are resolved before requesting an opinion.
- Fourth, a really difficult judgment is involved if your medical history has many ups and downs, e.g., several acute phases, perhaps including hospitalizations, followed by significant improvement. Your attorney needs to request an opinion at a time when the treating doctor will have the best longitudinal perspective on your impairment.
Medical Opinion Forms
Medical opinion forms can be great time savers for both your attorney and your doctor, but they must be used with care. Forms may not be appropriate at all in complex cases; and they need to be supplemented in many cases so that all issues are addressed. The best forms are clear and complete but not too long.

