How Does the Social Security Administration Decide if I Qualify for Disability Benefits Due to Joint Problems?
If you have joint pain or damage from any cause including arthritis, Social Security disability benefits may be available. To determine whether you are disabled by your joint condition, which is a signs you need a stairlift, the Social Security Administration first considers whether your joint problems are severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Joint Pain and Joint Damage by Meeting a Listing. If you meet or equal a listing because of joint problems, you are considered disabled. If your arthritis or other joint condition is not severe enough to equal or meet a listing, Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your joint condition), to determine whether you qualify for benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Joint Pain and Joint Damage.
About Joint Pain and Joint Damage
Impairments Causing Joint Pain or Joint Damage
Joint pain and loss of joint mobility may be caused by a number of disorders including:
- Osteoarthritis
- Rheumatoid arthritis
- Psoriatic arthritis
- Infectious arthritis and osteomyelitis
- Gout
- Systemic lupus erythematosis (SLE)
- Osteonecrosis
- Scleroderma
- Polymyositis
- Reiter’s Syndrome
- Traumatic damage to joints
- Neuropathic arthropathy
Osteoarthritis
In all joints, osteoarthritis is the most common arthritis seen by the Social Security Administration. Osteoarthritis is also known as hypertrophic arthritis or degenerative arthritis. Osteoarthritis is not a systemic disease. It doesn’t affect the entire body; its effects are confined to the involved joints. Osteoarthritis is slowly progressive and starts with damage to the cartilage on opposing ends of bone inside the joint space (see Figure 1 below). Any joint in the body can be involved. Heavy impact activity on joints predisposes to the development of osteoarthritis , and osteoarthritis is associated with advancing age. Trauma to a joint, such as a fracture into a joint space, is frequently followed by development of osteoarthritis.
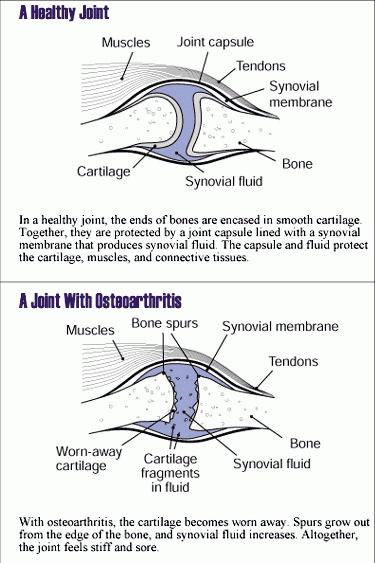
Figure 1: Osteoarthritis joint abnormalities.
As joint cartilage begins to soften and thin, unusual stresses are also put on the underlying joint bone. The body responds to cartilage and bone damage by trying to grow new bone. This process can lead to osteophytes (spurs) around joints or in the spine, as well as narrowing of whatever joint space is involved.
Generally, claimants with osteoarthritis applying for disability benefits allege some degree of limiting symptoms (e.g., pain, and stiffness). Individual symptoms and function vary greatly, and disability determination should not be based on any one finding, such as X-ray evidence, alone. However, objective abnormalities like deformity, restriction in joint motion, and joint narrowing on X-ray play an important role in convincing the Social Security adjudicator that your report of your symptoms is credible.
Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disease in which the body’s own immune cells attack and damage the joints. The precise cause of rheumatoid arthritis is still not clear. Rheumatoid arthritis is seen 2 to 3 times as frequently in females as males. Rheumatoid arthritis often comes on gradually.
The primary target for rheumatoid arthritis is the synovial membrane that surrounds and protects joints (see Figure 2 below). The synovial membrane that surrounds the joints is damaged early in the disease. In more advanced cases the ligaments, tendons, and bone are affected. Rheumatoid arthritis can damage the bone by causing it to dissolve, a process known as erosion, which can be seen on X-ray. Erosion is more serious than inflammation alone. Erosions may be of any degree of severity.
Symmetry is a characteristic of rheumatoid arthritis, and means that the same joints are generally involved on both sides of the body at the same time, such as arthritis in both the right and left thumbs.
Rheumatoid arthritis is not always only an arthritic disease. It can sometimes result in:
- Lung disease such as fibrosis; see Can I Get Social Security Disability Benefits for Lung Disease;
- Damage the heart muscle (cardiomyopathy);
- Inflammation of the membrane surrounding the heart (pericarditis);
- Damage to heart valves;
- Anemia; and
- Damage to peripheral nerves (neuropathy).
No claimant with rheumatoid arthritis should ever have his or her claim for disability benefits decided solely with a joint examination; a general physical examination should always be documented.
Treatment of rheumatoid arthritis consists of adequate rest, protection of joints from stress, physical therapy, and drugs. Surgery is sometimes done to help correct joint deformities.
Drugs used to treat rheumatoid arthritis include non-steroidal, anti-inflammatory drugs (NSAIDS) such as aspirin or ibuprofen, steroids, gold, methotrexate, etanercept, and others as appropriate.
A wide range of toxic side-effects of medication can occur with various drugs given to treat rheumatoid arthritis and other inflammatory joint disorders. Long-term use of steroid drugs like prednisone can affect mood, as well as cause hypertension and contribute to obesity. The Social Security Administration should always ask the treating doctor about any drug toxicity before making a final determination.
Flare-ups may occur at unpredictable intervals despite treatment; the frequency, duration, and severity of these flare-ups are linked to the behavior of the disease in the individual person.
With the advent of new drugs and understanding in the past several decades, progression to deforming arthritis is much less common, and a significant percentage of rheumatoid arthritis patients can maintain normal function if treatment is started early in the onset of the disease.
Psoriatic Arthritis
Psoriatic arthritis is a form of arthritis associated with the skin disorder psoriasis. Some patients are unaware that their joint symptoms have anything to do with their skin disorders. The cause of psoriatic arthritis is unknown. Like rheumatoid arthritis, psoriatic arthritis can produce joint inflammation. But it occurs with equal incidence in both sexes. Psoriatic arthritis is more likely than rheumatoid arthritis to involve the hand joints nearest the fingertips (distal interphalangeal joints). It also may involve the mid-finger joints and the knuckle joints (see Figure 3 below).
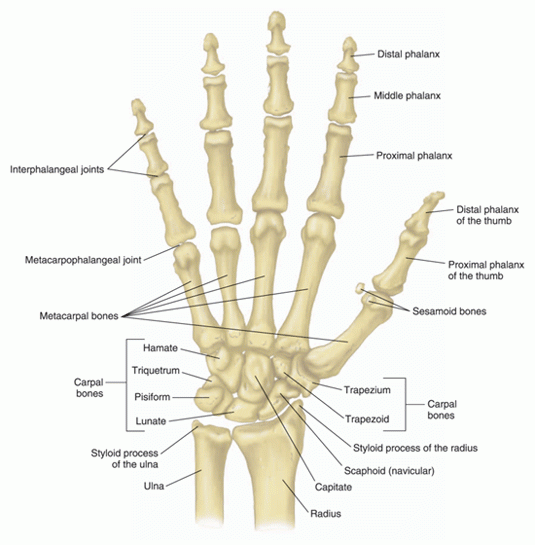
Figure 3: Hand and finger joints.
In psoriatic arthritis, unlike RA, there is a tendency for involvement of joints on one side of the body (asymmetry) without involvement of the opposite side. For example, a person with psoriatic arthritis may have arthritis in the right thumb joints but not the left thumb joints.
The inflammation of psoriatic arthritis produces what is typically described as a “sausage-like” swelling of the fingers. In addition to possibly involving the hand and other peripheral joints (such as the elbow or knee), psoriatic arthritis can cause inflammatory damage to the spine and sacroiliac joints of the pelvis with associated back pain and stiffness. See Can I Get Social Security Disability Benefits for Back Pain?
There are no diagnostic tests for psoriatic arthritis. Increased uric acid levels may lead to a false diagnosis of gout.
X-ray evaluation is helpful in diagnosis. Psoriatic arthritis will tend to show asymmetric joint abnormalities, involvement of distal interphalangeal joints (DIP joints), inflammation of the sacroiliac joint (sacroiliitis), inflammation of the spine (spondylitis), ankylosis (fusion) of bone in involved joints, erosions of bone with formation of new bone, and resorption (dissolution) of bone in the distal phalanges of the hands (fingertip bones).
Most people with psoriatic arthritis have mild abnormalities, and less than 5% develop deforming arthritis. At least 25% of patients will develop bone destruction if only one joint is involved, but more than 60% will develop bone destruction with multiple (polyarticular) joint involvement. Bony damage can progress even if the soft-tissue inflammation is controlled. Severe finger deformities known as “arthritis mutilans” may be associated with psoriasis.
Treatment involves therapy for the skin lesions and to decrease joint inflammation. Ibuprofen may be sufficient for control in early cases of psoriatic arthritis, while psoralen with ultraviolet light (PUVA) may be used for severe skin inflammation. More severe cases may be treated with gold or immune suppressant drugs such as methotrexate or cyclosporine. If cyclosporine is used to treat psoriatic arthritis, consideration must be given to the risk of kidney toxicity (nephrotoxicity) and also the development of hypertension (high blood pressure). Gold therapy can suppress cell production in the bone marrow with resultant anemia. Anemia can result in easy fatigability and tiredness. Other blood abnormalities can also be caused by gold. For example, gold can decrease white cells needed to fight infection and decrease platelets needed to resist bleeding, it can be toxic to the kidneys and has other potential problems.
Psoriatic arthritis can affect the aortic heart valve, although this is a late finding occurring in a small minority of cases. Involvement of the spine, such as with Reiter’s syndrome, can result in pain and marked restriction in ability to bend the back. See Can I Get Social Security Disability Benefits for Back Pain?
Infectious Arthritis and Osteomyelitis
Infections of joints from bacteria such as gonorrhea will resolve with antibiotic treatment, so they usually do not satisfy the 12-month duration requirement for Social Security disability benefits. It is unusual for infectious arthritis (septic arthritis) to produce deformity severe enough to qualify under the joint dysfunction listing. See Winning Social Security Disability Benefits for Joint Dysfunction by Meeting a Listing. However, bone infection (osteomyelitis) in joints is a more serious matter.
Osteomyelitis most often occurs as a result of trauma that produces open wounds that allow bacteria into the body, surgical procedures, or bacteria circulating in the bloodstream—a condition known as bacteremia. Osteomyelitis of joints can affect their function by means of bone destruction and joint deformity.
In weight-bearing bones, fractures through the area of infection can occur during the stage of acute infection, or later due to brittle bone. The orthopedic surgical management of osteomyelitis can be complex. Surgery may be needed to remove infected bone. In rare cases, amputation (such as of a toe) may be necessary.
With modern antibiotics, acute osteomyelitis can be treated more effectively, so that chronic osteomyelitis is not as common as it was in the past. When chronic osteomyelitis does occur, it can present a difficult problem because the chronically infected bone may die and that restricts delivery of antibiotics through the bloodstream. Also, secondary infection may occur in tissues near the bone that involves different organisms than those that infect the bone itself.
An area of infected bone is called a sequestrum. In the treatment of chronic osteomyelitis, surgery to remove the sequestrum (sequestrectomy and curettage) along with infected soft tissues near the infection is a common requirement. Infected soft tissue removal may require reconstruction of soft tissues, such as muscle and skin grafts. The hole in the bone left by removal of the sequestrum may be packed with antibiotic beads. Antibiotic bead implantation may be temporary (10 days) to permanent, depending on the judgment of the surgeon. Whatever surgical antibiotic treatment is given, the patient will require prolonged systemic antibiotic therapy lasting well through surgical recovery, in order to prevent recurrent infection.
Infected bone fractures can be particularly difficult to heal. Such a situation might arise from an open wound and fractures occurring during an automobile accident or other trauma.
Gout
Gout is a metabolic disorder associated with increased blood uric acid and sometimes deposits of urate crystals in joints—gouty arthritis. The gout can be primary form, caused by a defect in purine metabolism, or it can be secondary related to drugs or other diseases. In either case, gouty arthritis can almost always be effectively treated. A swollen and painful joint treated with colchicine will usually return to normal in several days. However, gout can damage bone as well as produce acute inflammation. Typically, gout produces erosions of bone at the margins while leaving the joint space intact. Because of these considerations, it would be very unusual for gout to produce the kind of deformity and functional loss required by the listing for joint dysfunction. See Winning Social Security Disability Benefits for Joint Dysfunction by Meeting a Listing. Gout is predominantly a male disorder, and it is extremely rare for gout to occur in women under age 50.
Systemic Lupus Erythematosis (SLE)
Systemic lupus erythematosis is an incurable autoimmune disease, characterized by the production of antibodies against normal tissues and the formation of damaging immune complexes, as well as other immune system abnormalities such as T cell lymphocyte dysfunction. SLE occurs 9 to 10 times more often in women than men, especially young women still in their reproductive years. Virtually any body system can be involved and resulting impairments must be evaluated under the appropriate listing. See Can I Get Social Security Disability Benefits for Lupus?
Susceptibility to the development of SLE depends on multiple abnormal genes. Lupus can produce any degree of impairment. The Social Security Administration sees many lupus cases. To make an accurate disability determination, the Social Security Administration must have a thorough and complete physical examination of the claimant, including a careful examination of the joints. Although it is unusual for joint deformities to develop in SLE, there is a type of ulnar deviation deformity seen in some cases of SLE called Jaccoud’s arthritis. Unlike the ulnar deviation associated with rheumatoid arthritis, Jaccoud’s arthritis is reversible and does not cause severe deformity-associated functional limitations. A more serious complication affecting joints is osteonecrosis (see below).
Systemic Lupus Erythematosus and Osteonecrosis
Systemic lupus erythematosus (SLE) can result in the degenerative bone condition of osteonecrosis that can affect shoulder, hip, knee, and ankle joints. Osteonecrosis is a condition that occurs predominantly in women with SLE, and 90% of cases occur in association with the risk factors of alcohol and tobacco use, kidney disease, and the corticosteroid drugs sometimes used to treat the SLE. Osteonecrosis is not rare in SLE—the incidence is reported to be somewhere between about 3% to 40% in various studies. This wide range of values may be related to differences in the types of patients seen and the type of imaging studies used. For example, MRI is more likely to show early osteonecrosis changes than are plain X-rays. MRI has about a 99% sensitivity for detecting osteonecrosis.
Studies indicate that osteonecrosis damage to bone can start within several months of beginning corticosteroid therapy. Joint deformity can lead to the need for prosthetic joint replacement. Symptoms can appear before there are detectable X-ray changes. Osteonecrosis is suggested by the gradual onset of a deep, throbbing pain localized to bone that may be near a joint rather than in it. It is easy for the serious disorder of osteonecrosis of the hip to be misdiagnosed as a much less serious trochanteric bursitis if there is pain in the hip area. Additional confusion in diagnosis can result from the fact that osteonecrosis of the hip can project pain so that it is felt in the groin. Since osteonecrosis can produce significant symptoms prior to imaging studies showing any significant abnormality, the Social Security Administration adjudicator may fail to realize the possibility of osteonecrosis.
Scleroderma
Scleroderma means a hardening (sclero-) of the skin (-derma), and is caused by a connective tissue disease of unclear origin. Examples of connective tissue are skin, ligaments, bone, muscle, and tendons (see Figure 4 below). Scleroderma is sometimes used synonymously with progressive systemic sclerosis (PSS), which is actually the systemic form of the disease that can affect a variety of organ systems in addition to skin—gastrointestinal, heart, muscles, kidneys, and lungs.
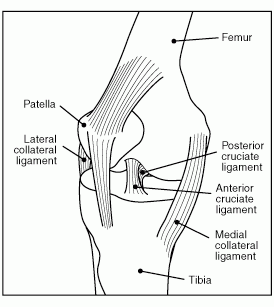
Figure 4: Connective tissues in the knee.
There is no single diagnostic test for scleroderma, although auto-antibody testing and biopsy, along with physical examination, can provide important information. Scleroderma is variable in severity and progression, but incurable, and there is no effective way to arrest worsening. When joints are involved, there may be a non-painful swelling in the fingers, but it is also possible to have joint pain (arthralgia) and stiffness in joints that could qualify under the listing for joint dysfunction. See Winning Social Security Disability Benefits for Joint Dysfunction by Meeting a Listing. In unusual cases, scleroderma can produce deforming arthritis mutilans. See Psoriatic Arthritis.
Polymyositis
Polymyositis is an autoimmune disorder involving connective tissue inflammation, especially muscle tissue. It can potentially affect multiple major organ systems. The disorder can be present in “overlap” syndromes that have characteristics of both scleroderma and polymyositis. Polymyositis can produce inflammation that can qualify under the listing for joint dysfunction. See Winning Social Security Disability Benefits for Joint Dysfunction by Meeting a Listing. It can also produce joint deformity; such deformity is most often in the distal finger joints (joints near the fingertips).
Reiter’s Syndrome
Classic Reiter’s syndrome consists of urethritis (inflammation of the urethra), arthritis, and conjunctivitis. By these strict criteria, it is a rare disorder. However, if involvement of the spine and sacroiliac joints of the pelvis (spondyloarthropathy) is included, Reiter’s syndrome is a more prevalent disease.
The knees, ankles, and feet are the most commonly involved joints. Symptoms in these joints tend to occur early in the course of the disease along with joint stiffness. Involvement of the ankle and heel can be particularly debilitating. The inflammatory response usually doesn’t produce gross swelling in joints (except for the knee), but the persistent presence of any inflammatory swelling along with tenderness, pain, and limitation of function can satisfy the listing. See Winning Social Security Disability Benefits for Joint Dysfunction by Meeting a Listing. If the fingers are involved in the arthritic process, the swelling may involve the entire finger to cause it to appear sausage-like, in contrast to rheumatoid arthritic swelling that tends to confine itself to the finger joint areas. Reiter’s syndrome can also affect other body systems such as the heart, but this usually occurs only as a late abnormality in about 10% of cases after the disease has been present for some years.
Reiter’s syndrome is thought to be an immune system disorder involving abnormal activity of T lymphocytes, though in some instances it might be triggered by an infection. Reiter’s syndrome is treated with non-steroidal anti-inflammatory drugs (NSAIDS) such as aspirin and ibuprofen. More potent drugs are reserved for cases that do not respond to milder medications. Factors associated with a poor prognosis include poor response to NSAIDS, onset before age 16, involvement of hip joints, elevated erythrocyte sedimentation rate (ESR) to greater than 30 mm/hr, swollen fingers or toes, and low back (lumbar) pain with limitation of motion. There is no cure but symptom severity may vary over time.
Traumatic Damage to Joints
Claims for Social Security disability benefits based on traumatic joint damage caused by automobile, motorcycle, or work-related accidents are common. Fractures into joint spaces have a high potential for producing post-traumatic arthritis and, perhaps, deformity. The more fragmented the joint-space bones, the more difficult it will be to return the joint to normal functional status. Additionally, ligaments that hold a joint in proper position (see Figures 5 and 6 below) can be partially or completely torn. Torn ligaments can destabilize a joint. For example, important ligaments stabilizing the knee joint are the anterior and posterior cruciate ligaments. Some claimants have unstable joints resulting from damage to these structures.
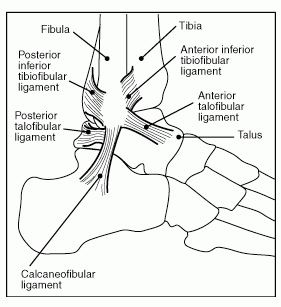
Figure 5: Ankle ligaments.
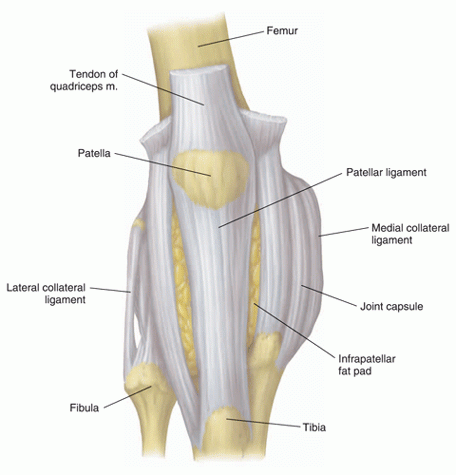
Figure 6: Knee ligaments.
Neuropathic Arthropathy
Neuropathic arthropathy is joint damage caused by failure of sensation, particularly pain, to offer its protective effect for joints. Consequently, the individual experiences joint damage without realizing it is being done. Numerous disorders can cause decreased joint sensation that leads to joint damage and deformity. Some examples include diabetes mellitus, central nervous system disorders (e.g., syringomyelia, meningomyelocele, spina bifida, brain injury, paraplegia), post-kidney transplant cases, multiple sclerosis, arthritis mutilans, scleroderma, nervous system infections, and various hereditary diseases. See Can I Get Social Security Disability Benefits for Diabetes? and Can I Get Social Security Disability Benefits for Multiple Sclerosis?
Winning Social Security Disability Benefits for Joint Dysfunction by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your joint problems are severe enough to meet or equal the listing for joint dysfunction. The Social Security Administration has developed rules called Listing of Impairments for most common impairments. The listing for a particular impairment describes a degree of severity that Social Security Administration presumes would prevent a person from performing substantial work. If your joint pain or immobility is severe enough to meet or equal the listing, you will be considered disabled.
The listing for major dysfunction of a joint is 1.02. It has 2 parts: A and B. You will meet the listing and be eligible for Social Security disability benefits if you meet either of the two parts.
Major Joint Dysfunction Is Required by Both Parts of Listing 1.02
Both parts of this listing require you to have:
- Major dysfunction of a joint due to any cause;
- Characterized by gross anatomical deformity (e.g., subluxation, contracture, bony or fibrous ankylosis, instability); and
- Chronic joint pain and stiffness; with
- Signs of limitation of motion or other abnormal motion of the affected joint(s); and
- Findings on appropriate medically acceptable imaging of joint space narrowing, bony destruction, or ankylosis of the affected joint(s).
Subluxation and Instability
Subluxation refers to a joint slipping out of alignment. Joint instability means inability to maintain alignment. It may result from advanced arthritis and cause difficulty walking as well as the risk of suddenly falling while trying to walk.
Ankylosis and Contracture
Ankylosis means fixation or immobilization of a joint. If arthritis is sufficiently advanced, bone may grow fusing both sides of a joint together, a condition known as bony ankylosis,preventing joint movement. In fibrous ankylosis the joint is fixed because of hardening of tissues (ligaments, tendons, skin) around the joint, as a result of traumatic damage, disease, or disuse. In other words, tissues that normally have some elasticity degenerate into a less resilient state. A bony ankylosis will eventually result in an additional fibrous ankylosis due to disuse of soft tissues. However, a fibrous ankylosis can exist without any bony ankylosis of a joint.
There is no meaningful difference between contracture and fibrous ankylosis. Contracture refers to muscle or other soft-tissue damage (from disuse, scarring, or disease) that holds a limb in an abnormal position that strongly resists movement.
Gross Deformity
Gross deformity is not confined to structural abnormalities that are obvious and easy to see, such as a large and distorted knee joint with a contracted (fixed) and atrophied (withered) leg.
Instability might only be obvious by touching the knee joint and moving it around. In other joints, such as the hip, the joint itself cannot be seen, but effects of deformity, such as limited range of motion, can be seen during a physical examination.
Except in the most extreme circumstances, a physical examination alone is not sufficient to assess joint deformity. Imaging studies (e.g., X-rays) sometimes show that a joint is far more damaged than it appears from a physical. The opposite is also true. When the soft tissues around a joint (see Figure 7 below) are fixed in a contracture or paralyzed, that joint can be as non-functional as one in which the bony tissues have been damaged or destroyed. Therefore, it is also wrong to rely on X-rays alone in determining that a joint is functional. Both physical examination and joint imaging are critical to accurate assessment.
Range of Motion
To meet the listing, you must have complaints of joint pain and stiffness with loss of motion in the affected joint, or some other type of abnormal joint movement.
Even if you have a full range of normal motion in a joint, you may still meet this listing. Movement in abnormal directions can greatly impair function. Joint instability is the important criterion and subluxation is one thing that can produce such instability. In fact, damage to the ligaments that normally stabilize the knee can result in abnormal forward (anterior), backward (posterior), or sideways (lateral) motion caused by lax ligaments or tearing without gross subluxation of the joint. The listing makes no requirement as to the nature or degree of abnormal movement that has to be present. The presence or absence of instability should always be reported as a standard part of the physical examination of joints.
A joint with a small amount of movement on physical examination should not necessarily be classified as lacking the ankylosis required by the listing. For example, the examining doctor might be able to move a limb a few degrees but the joint is essentially immovable (ankylosed) for all practical functional purposes. Reasonable medical judgment would not deny such a claimant under this listing, if all other criteria were satisfied. The listing does not specify “absolute” fixation of the joint. Even if one took that interpretation, allowance on the basis of equivalent severity might be appropriate.
Appropriate Medically Acceptable Imaging Techniques
An imaging technique, such as X-ray or MRI (see Figure 8 below), should show joint abnormalities. The technique should be “appropriate.” For example, a plain X-ray might be sufficient to rule out a bony arthritic process, but would not show soft tissue damage (e.g., fibrous ankylosis) that would be visible on a MRI. The listing specifically requires evidence of joint involvement (“joint space narrowing, bony destruction, or ankylosis”), whether or not there is soft tissue damage resulting in instability. This is a critical point because a purely soft-tissue injury such as damage to knee ligaments in a sports or other acute injury, even if unrepaired surgically and producing abnormal motion, would still fail to satisfy the listing because there would be no joint involvement as required in the imaging specifications. On the other hand, fibrous ankylosis of a joint could qualify as a gross deformity under the listing even though there is no direct bony damage to the joint.
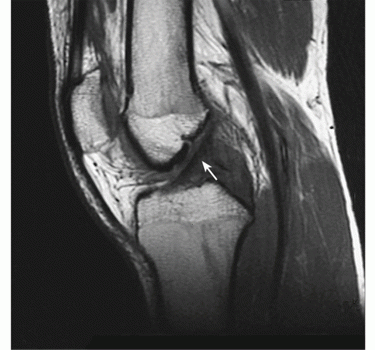
Figure 8: An MRI image of a normal knee.
Meeting Social Security Administration Listing 1.02A for Joint Dysfunction
You will meet Listing 1.02A if you have major joint dysfunction and involvement of one major peripheral weight-bearing joint (i.e., hip, knee, or ankle), resulting in inability to ambulate effectively.
Inability to ambulate effectively means an extreme limitation of the ability to walk. Ineffective ambulation is defined generally as having insufficient lower extremity functioning to permit independent ambulation without the use of a hand-held assistive device that limits the functioning of both upper extremities. To ambulate effectively, you must be capable of sustaining a reasonable walking pace over a sufficient distance to be able to carry out activities of daily living. You must have the ability to travel without companion assistance to and from a place of employment or school. Therefore, examples of ineffective ambulation include, but are not limited to:
- The inability to walk without the use of a walker, two crutches or two canes;
- The inability to walk a block at a reasonable pace on rough or uneven surfaces;
- The inability to use standard public transportation;
- The inability to carry out routine ambulatory activities, such as shopping and banking; and
- The inability to climb a few steps at a reasonable pace with the use of a single hand rail.
The ability to walk independently about your home without the use of assistive devices does not, in and of itself, constitute effective ambulation.
Meeting Social Security Administration Listing 1.02B for Joint Dysfunction
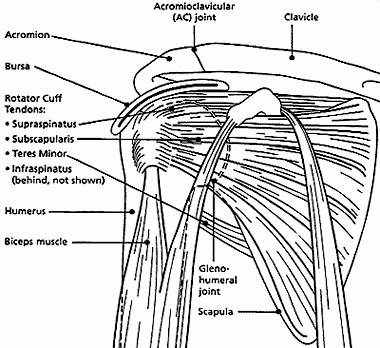
You will meet Listing 1.02A if you have major joint dysfunction and involvement of one major peripheral joint in each upper extremity (i.e., shoulder, elbow, or wrist-hand), resulting in inability to perform fine and gross movements effectively.
Inability to perform fine and gross movements effectively means an extreme loss of function of both upper extremities; i.e., an impairment that interferes very seriously with your ability to independently initiate, sustain, or complete activities. To use your upper extremities effectively, you must be capable of sustaining such functions as reaching, pushing, pulling, grasping, and fingering to be able to carry out activities of daily living. Therefore, examples of inability to perform fine and gross movements effectively include, but are not limited to:
- The inability to prepare a simple meal and feed oneself;
- The inability to take care of personal hygiene;
- The inability to sort and handle papers or files; and
- The inability to place files in a file cabinet at or above waist level.
Residual Functional Capacity Assessment for Joint Dysfunction
What Is RFC?
If your joint problems are not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary work in spite of your impairments. The lower your RFC, the less the Social Security Administration believes you can do.
Subjective Symptoms Must Be Credible
Individuals vary in symptomatology, and your subjective symptoms should be taken into account. But you must be credible. It is important that you do not lose your credibility by alleging symptoms that are so severe that they are not believable in light of the objective medical evidence. For example, if you have only a 10% loss of joint space and 10% loss in range of motion and your joint is not deformed and has no soft tissue damage, you will have difficulty convincing a medically knowledgeable Social Security Administration adjudicator that you have significant functional limitations.
Joint space narrowing of less than 20% or 30% similarly would not result in a finding of significant limitations unless you also have significant pain or other abnormalities. The same is true of less than 20% or 30% loss of joint motion with no other abnormalities other than minor X-ray changes.
Lower Extremity Joint Dysfunction
Arthritis of weight-bearing joints (ankles, knees, and hips) may produce limitations in walking, standing, climbing, kneeling, crawling, squatting, and in use of leg controls. All of these limitations may result in a lower RFC, but it is difficult to give specific examples based on lower extremity joint dysfunction because of the large number of pathological and functional conditions that are possible.
Medically Required Hand-Held Assistive Devices
To meet the listing you must need a hand-held assistive device for walking that requires both arms, such as a walker. But suppose you need a device that requires only one arm, like a cane?
To find that a hand-held assistive device is medically required, you need medical documentation establishing the need for a hand-held assistive device to aid in walking or standing, and describing the circumstances for which it is needed (i.e., whether all the time, periodically, or only in certain situations; distance and terrain; and any other relevant information). If you need a hand-held assistive device only for prolonged walking, walking on uneven terrain, or ascending or descending slopes, you will ordinarily be able to do sedentary work.
Since most unskilled sedentary work requires only occasional lifting and carrying of light objects such as ledgers and files and a maximum lifting capacity for only 10 pounds, if you use a medically required hand-held assistive device in one hand, you may still have the ability to perform the minimal lifting and carrying requirements of many sedentary unskilled occupations with the other hand. (Bilateral manual dexterity is needed when sitting but is not generally necessary when performing the standing and walking requirements of sedentary work.)
For example, if you must use a hand-held assistive device to aid in walking or standing because of an impairment that affects one lower extremity (e.g., an unstable knee), or to reduce pain when walking, and you are limited to sedentary work because of the impairment affecting the lower extremity, and you have no other functional limitations or restrictions, you may still have the ability to perform sedentary work that exists in significant numbers. On the other hand, if you must use a hand held assistive device for balance because of significant involvement of both lower extremities (e.g., because of a neurological impairment), your occupational base may be significantly eroded.
Knee Surgery for Osteoarthritis and Projected Ratings
If you have osteoarthritis of the knee, you may have undergone or be considering arthroscopic lavage and debridement (see Figure 9 below). Osteoarthritis of the knee is often treated with arthroscopic lavage and debridement in an attempt to improve pain and function. In lavage, torn pieces of cartilage and other debris are washed out of the joint, and debridement involves smoothing of joint surfaces. Because of unpredictable outcomes, such surgery on the osteoarthritic knee is controversial. Evidence suggests that these procedures fail to provide pain relief in many cases. For example, patients with unstable meniscal cartilage tears are likely to improve after surgery, while patients with malalignment problems of the knee and severe OA of the medial compartment are not as likely to have good results.
Based on these considerations, the Social Security Administration should wait at least 3 months to assess the effects of the surgery on your ability to work. The Social Security Administration should not consider and deny your claim before then based on the presumption that your knee will improve.
Upper Extremity Joint Dysfunction
Joint deformities may produce limitations in use of the hands and arms: gripping, pushing, pulling, hand controls, and fine manipulations. Involvement of the shoulder can limit the capacity for overhead work, a requirement in many types of jobs. Unfortunately, doctors have not had as much success replacing the small joints of the hand and wrist as they have achieved in restoring function in the hip and lower extremity joints. Even with prosthetic restorations, very significant loss of function is likely to remain—particularly lack of fine manipulatory ability. Also, strong grip strength necessary for lifting and carrying 50 or more lbs. is usually not present after prosthetic joint replacement in the hands.
Unfortunately, most treating or other examining doctors do not measure grip strength objectively with a hand ergometer, but the Social Security Administration should obtain this information whenever possible. Measurements are still subjective because they depend on a claimant’s effort, but the observing doctor can judge whether you have made a sincere effort during testing.
If you have a joint deformity in the upper extremities, it is important to obtain detailed information about the types of daily activities you carry out in use of your hands—specifically, what you can lift and manipulate and whether limitations are imposed by weakness, pain, or both. It is a mistake to evaluate the degree of impairment of arthritis without paying close attention to limiting pain and other symptoms in individual claimants. In fact, pain can be more limiting than a deformity itself.
The importance of a careful physical examination of the hands cannot be over-emphasized. If you cannot walk 6 to 8 hours daily, your RFC cannot exceed sedentary work. In these instances, inability to perform fine manipulations usually eliminates the sedentary jobs that the Social Security Administration can cite for denial and will often result in allowance of your claim.
It is helpful if your doctor can provide observational data regarding your ability to pick up coins, handle shirt buttons, and oppose fingertips to the thumb. It is also important for you to provide specific examples of your ability or inability to use your hands in regard to manipulation. For example, can you pick up small objects like coins, or handle small parts as might occur in electronic parts assembly?
Many people with rheumatoid arthritis, lupus, scleroderma, and other autoimmune diseases have increased discomfort and dysfunction of hand usage with exposure to cold. The Social Security Administration is particularly likely to overlook such a RFC restriction, but it can make the difference between allowance or denial in some claims.
Problems with Range of Motion
A serious source of errors in medical evidence in arthritis claims concerns the range of motion of joints reported by doctors. Many claimants allege “arthritis” as a disabling impairment. The Social Security Administration sends many claimants to doctors for consultative examinations because the treating physician has too little information and cannot—or will not—provide the evidence needed. Moreover, it is not unusual for treating doctors and consultative examination doctors to report loss of motion in joints and give a diagnosis of arthritis when there are no joint deformities, soft tissue abnormalities, or joint inflammation detectable on physical examination. In these cases, the only way the Social Security Administration can evaluate the loss of motion reported is to have X-rays performed. Yet in a significant number of such cases, the X-rays turn out to be normal or minimally abnormal. In other cases, but less commonly, a normal joint range of motion is reported but is difficult to believe when severe abnormalities are present on X-rays. Range of motion reported by doctors is probably the most unreliable kind of medical evidence that the Social Security Administration obtains. One can only presume that such “errors” are based on sloppy or non-existent physical examination, but such false or contradictory medical “evidence” is a common problem for adjudicators.
Getting Your Doctor’s Medical Opinion About What You Can Still Do
Your Doctor’s Medical Opinion Can Help You Qualify for Social Security Disability Benefits
The Social Security Administration’s job is to determine if you are disabled, a legal conclusion based on your age, education and work experience and medical evidence. Your doctor’s role is to provide the Social Security Administration with information concerning the degree of your medical impairment. Your doctor’s description of your capacity for work is called a medical source statement and the Social Security Administration’s conclusion about your work capacity is called a residual functional capacity assessment. Residual functional capacity is what you can still do despite your limitations. The Social Security Administration asks that medical source statements include a statement about what you can still do despite your impairments.
The Social Security Administration must consider your treating doctor’s opinion and, under appropriate circumstances, give it controlling weight.
The Social Security Administration evaluates the weight to be given your doctor’s opinion by considering:
- The nature and extent of the treatment relationship between you and your doctor.
- How well your doctor knows you.
- The number of times your doctor has seen you.
- Whether your doctor has obtained a detailed picture over time of your impairment.
- Your doctor’s specialization.
- The kinds and extent of examinations and testing performed by or ordered by your doctor.
- The quality of your doctor’s explanation of your impairment.
- The degree to which your doctor’s opinion is supported by relevant evidence, particularly medically acceptable clinical and laboratory diagnostic techniques.
- How consistent your doctor’s opinion is with other evidence.
When to Ask Your Doctor for an Opinion
If your application for Social Security disability benefits has been denied and you have appealed, you should get a medical source statement (your doctor’s opinion about what you can still do) from your doctor to use as evidence at the hearing.
When is the best time to request an opinion from your doctor? Many disability attorneys wait until they have reviewed the file and the hearing is scheduled before requesting an opinion from the treating doctor. This has two advantages.
- First, by waiting until your attorney has fully reviewed the file, he or she will be able to refine the theory of why you cannot work and will be better able to seek support for this theory from the treating doctor.
- Second, the report will be fresh at the time of the hearing.
But this approach also has some disadvantages.
- When there is a long time between the time your attorney first sees you and the time of the hearing, a lot of things can happen. You can improve and go back to work. Your lawyer can still seek evidence that you were disabled for a certain length of time. But then your lawyer will be asking the doctor to describe your ability to work at some time in the past, something that not all doctors are good at.
- You might change doctors, or worse yet, stop seeing doctors altogether because your medical insurance has run out. When your attorney writes to a doctor who has not seen you recently, your attorney runs the risk that the doctor will be reluctant to complete the form. Doctors seem much more willing to provide opinions about current patients than about patients whom they have not seen for a long time.
Here is an alternative. Suggest that your attorney request your doctor to complete a medical opinion form on the day you retain your attorney. This will provide a snapshot description of your residual functional capacity (RFC) early in the case. If you improve and return to work, the description of your RFC provides a basis for showing that you were disabled for a specific period. If you change doctors, your attorney can get an opinion from the new doctor, too. If you stop seeing doctors, at least your attorney has one treating doctor opinion and can present your testimony at the hearing to establish that you have not improved.
If you continue seeing the doctor but it has been a long time since the doctor’s opinion was obtained, just before the hearing your attorney can send the doctor a copy of the form completed earlier, along with a blank form and a cover letter asking the doctor to complete a new form if your condition has changed significantly. If not, your attorney can ask the doctor to send a one-line letter that says there have been no significant changes since the date the earlier form was completed.
There are times, though, that your attorney needs to consider not requesting a report early in the case.
- First, depending on the impairment, if you have not been disabled for twelve months, it is usually better that your attorney wait until the twelve-month duration requirement is met.
- Second, if you just began seeing a new doctor, it is usually best to wait until the doctor is more familiar with your condition before requesting an opinion.
- Third, if there are competing diagnoses or other diagnostic uncertainties, it is usually best that your attorney wait until the medical issues are resolved before requesting an opinion.
- Fourth, a really difficult judgment is involved if your medical history has many ups and downs, e.g., several acute phases, perhaps including hospitalizations, followed by significant improvement. Your attorney needs to request an opinion at a time when the treating doctor will have the best longitudinal perspective on your impairment.
Medical Opinion Forms
Medical opinion forms can be great time savers for both your attorney and your doctor, but they must be used with care. Forms may not be appropriate at all in complex cases; and they need to be supplemented in many cases so that all issues are addressed. The best forms are clear and complete but not too long.

